Serviços Personalizados
Journal
Artigo
Links relacionados
Compartilhar
Odontoestomatología
versão impressa ISSN 0797-0374versão On-line ISSN 1688-9339
Odontoestomatología vol.25 no.42 Montevideo 2023 Epub 01-Dez-2023
https://doi.org/10.22592/ode2023n42e418
Case report
Intramuscular hemangioma with phleboliths of the tongue. Report of a clinical-pathological case
1 Cátedra y Laboratorio de Anatomía Patológica, Facultad de Odontología de la Universidad de la República. Montevideo-Uruguay. Guillermina.2671@gmail.com
2 Escuela de Graduados, Facultad de Odontología de la Universidad de la República. Montevideo-Uruguay.
We present a case of intramuscular hemangioma with tongue phleboliths in a 60-year-old woman. Clinically it corresponded to a swelling of two years of evolution, without signs that suggested its vascular origin. After her initial evaluation, an excisional biopsy of the lesion was performed for histopathological study.
In the histological study it was possible to observe a rounded and circumscribed tissue formation made up of fibrous connective tissue with abundant congestive capillaries that displaced the muscle tissue, highlighting the presence of thrombi with calcifications arranged in concentric layers (phleboliths). Based on these morphological findings, the definitive diagnosis was intramuscular capillary hemangioma with tongue phleboliths. To confirm the vascular neoplastic nature of the lesion, histochemical immunostaining was performed with the GLUT1 antibody. It is noteworthy, according to the bibliographic review carried out in PubMed, that this pathological entity is rare, particularly in the tongue.
Keywords: Hemangioma; intramuscular hemangioma; tongue
Se presenta un caso de hemangioma intramuscular con flebolitos de lengua en una mujer de 60 años. Clínicamente correspondía a una tumefacción de dos años de evolución, sin signos que sugirieran su origen vascular. Luego de su evaluación inicial se realizó biopsia excéresis de la lesión para su estudio histopatológico.
En el estudio histológico se pudo observar una formación tisular redondeada y circunscripta constituida por tejido conjuntivo fibroso con abundantes capilares congestivos que desplazaban el tejido muscular, destacándose la presencia de trombos con calcificaciones dispuestas en capas concéntricas (flebolitos). En base a estos hallazgos morfológicos, el diagnóstico definitivo fue de hemangioma capilar intramuscular con flebolitos de lengua. Para confirmar la naturaleza neoplásica vascular de la lesión se realizó inmunomarcación con el anticuerpo GLUT1. Es de destacar, de acuerdo a la revisión bibliográfica realizada en PubMed, que esta entidad patológica es rara, particularmente en la lengua.
Palabras claves: Hemangioma; Hemangioma Intramuscular; lengua
Apresentamos um caso de hemangioma intramuscular com flebólitos de língua em uma mulher de 60 anos. Clinicamente, correspondia a um inchaço com duração de dois anos, sem sinais que sugerissem sua origem vascular. Após sua avaliação inicial, foi realizada biópsia excisional da lesão para estudo histopatológico.
No estudo histológico pôde-se observar uma formação tecidual arredondada e circunscrita constituída por tecido conjuntivo fibroso com abundantes capilares congestivos que deslocavam o tecido muscular, destacando a presença de trombos com calcificações dispostos em camadas concêntricas (flebólitos). Com base nesses achados morfológicos, o diagnóstico definitivo foi de hemangioma capilar intramuscular com flebólitos de língua. Para confirmar a natureza neoplásica vascular da lesão, foi realizada imunocoloração com o anticorpo GLUT1. Ressalta-se, de acordo com a revisão bibliográfica realizada no PubMed, que esta entidade patológica é rara, principalmente na língua.
Palavras-chave: Hemangioma; Hemangioma Intramuscular; língua
Introduction
Hemangioma is a benign vascular neoplasm that is classified depending on its location as intraosseous, intramuscular, submucosal, subcutaneous, or cutaneous 1,2. It is a pathological process that is diagnosed at an early age, during early childhood, and slowly involves throughout life 1,3,4. However, it may occasionally manifest later in life, as seen in intramuscular hemangioma, due to its deep-seated location 1,3,4. Additionally, it is frequently associated with phleboliths of variable sizes, solitary or multiple 1,2,5.
Background
Hemangioma is a benign neoplasm made up of proliferated blood vessels that may occur in any vascularized tissue. Typically, it manifests in the neonatal stage and in early childhood1,2. Furthermore, its malignant transformation is rare, if it occurs at all. It can also be associated with some syndromes 1. In the head and neck, it usually manifests as a solitary lesion, and is more prevalent in females (1,3,8.
The etiology of hemangioma is not well-defined. It is thought to originate from an imbalance in the angiogenesis process, resulting from the action of different chemical mediators, such as vascular endothelial growth factor (VEGF), basic fibroblast growth factor (bFGF), and indoleamine 2,3-dioxygenase (IDO1) 1-3,8. This etiological association is inferred from the quantification of the above chemical mediators, which are found in high concentrations during the proliferative stage of the lesion and sharply decrease in the involution stage 1-3,8.
Another distinctive feature of this lesion is its evolution, presenting three clearly defined stages 1,2,4,9,10. Initially, the first stage, which in most cases occurs during the first month of extrauterine life, is marked by rapid growth, responsible for it becoming clinically apparent 1,2,4,9,10. Subsequently, in the second stage, the hemangioma usually ceases to grow, entering a phase of slow involution (1,2,4,9,10. However, it is occasionally detected in later life stages, as seen with intramuscular hemangioma, likely due to its deep-seated location 1,3,4. Less frequently, it may also exhibit rapid and expansive growth, possibly associated with trauma, infection, or endocrine changes, such as those occurring during puberty or pregnancy 2,6,7.
Intramuscular hemangioma is a relatively rare vascular tumor, representing less than 1% of all hemangiomas, and approximately 20% of these are found in the head and neck region, mainly in the masseter muscle 4,6,7,11-13. In the oral cavity, it is most frequently located in the tongue and lips, manifesting clinically as a soft swelling without alteration of the overlying mucosa 1,7). The clinical diagnosis can be difficult due to its deep-seated intramuscular location, low incidence, and the lack of specific symptoms and signs that point to a lesion of vascular origin (6,7.
As with all hemangiomas, intramuscular hemangioma is histologically classified as cavernous, capillary, and mixed 1,2,7,11,12,14. Specifically, capillary hemangioma, the most common variant, is made up of numerous small congestive vascular channels lined by proliferating endothelium, which in many cases partially or entirely occludes the vascular lumina 1,2,11,12. Another histological subtype of intramuscular hemangioma is the cavernous variant, characterized by large, irregular, dilated, and congestive endothelial channels 1,2,11,12. A capsule that circumscribes and delimits the lesion in both morphological patterns is typically identified (1,2,11,12. Additionally, the different histological variants often include other tissue components, such as adipose, fibrous, bone, and muscle tissue 1,2,11,12.
Making a definitive diagnosis of hemangioma requires differentiation from other vascular anomalies, which is challenging in most cases based solely on routine histopathological study 1,8,15. This is because hemangioma morphologically resembles pyogenic granulomas during its proliferative phase, when it can exhibit superimposed inflammation 1,8,15. Conversely, the histologic pattern observed in the involution phase is similar to that of vascular malformations 1,8,15. Therefore, a comprehensive clinical history and imaging studies are essential for an accurate, definitive diagnosis, and in some cases, routine histopathological examination must be complemented with immunohistochemical techniques 1,8,15. Particularly concerning immunohistochemical biomarkers, hemangiomas, like all vascular anomalies, test positive for antibodies expressed by endothelial cells, such as CD34, CD31, CD105, and ERG 1,8,9,15,16. However, unlike other tumors and vascular malformations, hemangioma expresses the marker GLUT1 (glucose transporter protein to endothelial cells) (1,8,9,15,16.
Particularly, intramuscular hemangioma shows phleboliths in 25% of cases, varying in size and appearing as solitary or multiple entities 5,6. Phleboliths correspond to thrombi with dystrophic calcification resulting from slowed-down blood flow, a common occurrence in this type of tumor 1,2,10-12,17. Typically, they appear as radiographic findings, visualized as circular laminar structures with concentric rings, exhibiting radiopacity and/or radiolucency. Alternatively, they may present as rings made up of a peripheral radiopaque layer and a central radiolucent nucleus 10,18. In specific cases, particularly those involving head and neck hemangiomas with phleboliths, it is crucial to make a differential diagnosis with other pathologies in the region associated with calcifications, such as salivary sialoliths, tonsilloliths, calcified lymph nodes, calcifying myositis, and carotid atherosclerotic plaques 6,12,18. An important distinguishing factor between phleboliths and salivary sialoliths is that phleboliths often manifest as small, randomly distributed multiple calcifications. In contrast, sialoliths frequently follow the linear pattern of the duct containing them 19. In some cases, the definitive diagnosis of lesions associated with phleboliths can be conclusively made through imaging studies, including computed tomography, magnetic resonance, and/or ultrasound, disregarding the histopathological examination 6,20.
Description
A 60-year-old woman, with no relevant medical history, consulted the oral and maxillofacial surgeon due to an asymptomatic lingual swelling of two years of evolution. On clinical examination, she exhibited an elevated lesion that altered the contour of the dorsal face and right lateral border of the tongue without affecting the overlying mucosa (Figure 1a). On palpation, a firm, soft, and mobile nodule of approximately 15 mm in diameter could be perceived, without thrill and/or pulse. Due to the absence of clinical signs suggesting a lesion of possible vascular origin, this group of lesions was not considered in the initial diagnostic hypothesis, partially explaining why imaging studies were not performed. Then, with the clinical diagnosis of the lingual nodule, we proceeded to perform an excisional biopsy of the lesion, which was sent for histopathological study (Figures 1b and 1c).
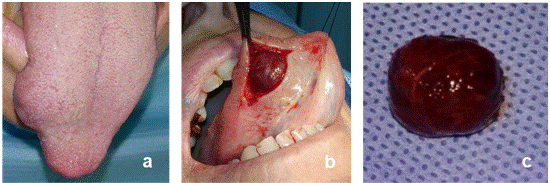
Figure 1: a. 15 mm diameter nodule altering the contour of the right lateral border of the tongue. b. Intraoperative image of the lesion, revealing its location in the lingual muscular plane. c. Fresh Macroscopic image of the resected lesion.
Macroscopic examination revealed that the specimen was made up of a rounded, firm, brownish piece of tissue measuring 14 mm in diameter. Upon cutting, it displayed a dark pasty content with whitish calcified elements (Figure 2).
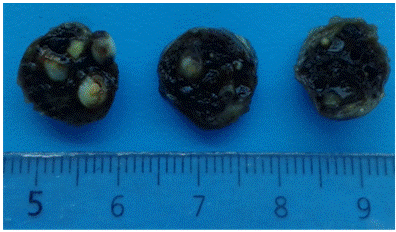
Figure 2: Macroscopic aspect of the surgical specimen sent to the Anatomic Pathology Laboratory of the Faculty of Dentistry, UdelaR.
Microscopically, the specimen revealed a rounded, well-circumscribed tissue formation displacing the bundles of muscle fibers. This formation was made up of fibrous connective tissue with abundant congestive capillaries, chronic inflammatory exudates, and interstitial hemorrhage (Figure 3a). Histologically, consistent with the macroscopic findings, calcified thrombi organized in concentric laminar structures (phleboliths) with chronic inflammatory cells and red blood cells were identified (Figure 3b and 3c). Considering these histopathologic features, the diagnosis was established as an intramuscular capillary hemangioma with tongue phleboliths.
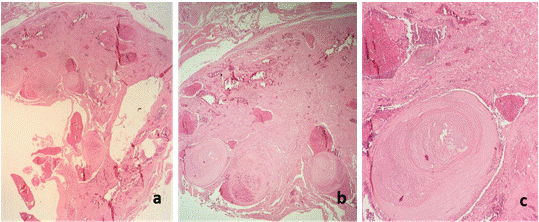
Figure 3: Microscopic study. a. Well-circumscribed tissue formation consisting of fibrous connective tissue, vascular lumina, and calcified thrombi (2x). b. Calcified thrombi (phleboliths) are evident (4x). c. Eosinophilic phlebolith made up of concentric calcified layers occupying the vascular lumen, directed towards the fibrous connective tissue periphery with inflammatory exudates and interstitial hemorrhage (10x). Stain: hematoxylin-eosin.
Complementary histochemical (Masson's trichrome) (Figure 4) and immunohistochemical techniques for the GLUT1 antibody (Figure 5) were also conducted, confirming the diagnosis of a tumor of vascular origin.
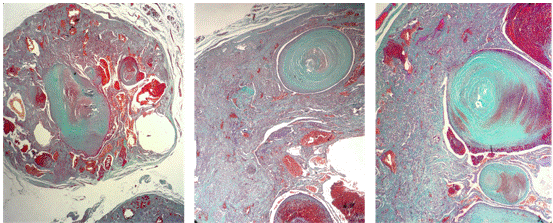
Figure 4: Masson's trichrome histochemical technique, revealing collagen fibers stained in bluish-green, red blood cells in red, and the nuclei of different cell populations within the lesion in lilac-brown.
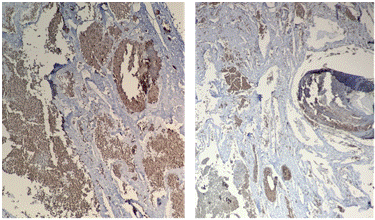
Figure 5: GLUT1 antibody positivity enabled the classification of this vascular lesion as a hemangioma. Immunohistochemical technique for GLUT1 antibody.
After 6 years of clinical follow-up, the patient remains well, without functional limitations nor recurrence of the lesion.
Discussion
Intramuscular hemangioma with tongue phleboliths represents a rare soft tissue entity, and its definitive diagnosis typically involves clinical examination supported by imaging studies, which reveal phleboliths as small, multiple, and randomly arranged calcifications (4,5,6,8-13,15,16,18-20. However, in this case, as often happens, imaging studies were not conducted due to its low incidence in the oral cavity and its deep-seated location, making recognition as a vascular lesion challenging through characteristic clinical signs such as pulse and/or thrill. Instead, an excisional biopsy of the lesion was performed 6,12. This therapeutic and diagnostic approach is based on the benign nature of the lesion-a well-circumscribed nodule on the lateral border of the tongue with no alteration of the overlying mucosa, as well as on the potential differential diagnoses required by lesions with a similar clinical presentation, including granular cell tumor, fibroma, leiomyoma, and solitary fibrous tumor 14,21.
Additionally, once the vascular nature of the lesion was established based on its microscopic characteristics, an immunohistochemical technique was employed for the GLUT1 antibody. Its positivity enabled the classification of the lesion as a vascular neoplasm, ruling out the possibility of a vascular malformation 1,8,15,17.
It is noteworthy that this case aligns with several characteristics described in the literature for intramuscular hemangiomas, such as its occurrence on the tongue-most frequent topography in the oral cavity-and its association with female patients, who exhibit the highest incidence of this pathology (1,3,8. However, it deviates in certain aspects from the typical features of this entity, justifying this publication to some extent. While the norm is its diagnosis at an early age, particularly in adolescents and young adults 1,4, the intramuscular hemangioma presented in this case was diagnosed in a 60-year-old patient. Therefore, it falls into the small group of hemangiomas typified in adulthood, likely due to its deep-seated location in the tongue at the intramuscular level 6. Additionally, its clinical presentation at an advanced age may also be attributed to local factors such as trauma and/or systemic factors like hormonal changes 2,12,16.
Conclusions
This case underscores the importance of considering intramuscular hemangioma as a potential diagnostic hypothesis when faced with a deep-seated nodular lesion in the tongue, even in adults, and in the absence of clinical signs such as pulse or thrill. Furthermore, it highlights the crucial role of imaging studies in determining the vascular nature of this type of nosological process and assessing its anatomical extension.
REFERENCES
1. Matthews F., Beratto O, Lamar JG. Hemangioma Intramuscular. Revista de la Facultad de Odontología Universidad Andrés Bello. 2012; 4(1): 5-8 [ Links ]
2. de Avila ÉD, de Molon RS, Conte Neto N, Gabrielli MAC, Hochuli-Vieira E. Lip cavernous hemangioma in a young child. Braz Dent J. 2010;21(4):370-4. [ Links ]
3. Kamatani T, Kondo S, Saito T, Shintani S, Shirota T, Hamada Y. Intramuscular hemangioma with phleboliths of the tongue. Indian J Dent. 2014;5(2):100. [ Links ]
4. Bayarogullari H, Çokkeser Y, Akbay E, Karaoglu E, Karaoglu E, Çevik C. Intramuscular cavernous hemangiomas arising from masseter muscles. J Clin Exp Investig. 2013;3(3):404-8. [ Links ]
5. Odedra PA, Patel SB, Goswami KG, Patel DD. Radiology Quiz, HeadHead and Neck. Indian J Radiol Imaging. 2007; 17(3):225-6. [ Links ]
6. Zengin AZ, Celenk P, Sumer AP. Intramuscular hemangioma presenting with multiple phleboliths: A case report. Oral Surg Oral Med Oral Pathol Oral Radiol. 2013;115(1):e32-6. [ Links ]
7. DeGiovanni JC, Simmonds J, Lang-Orsini M, Lee A. Recurrent Intramuscular Hemangioma (Infiltrating Angiolipoma) of the Lower Lip: A Case Report and Review of the Literature. Ear, Nose Throat J. 2022;101(5):306-11. [ Links ]
8. Kamra S, Chhaparwal Y. Intramuscular Hemangioma: Enigmatic Dilemma in Diagnosis. J Heal Sci Res. 2016;7(2):67-70. [ Links ]
9. Gouvêa Lima G de M, Moraes RM, Cavalcante ASR, Carvalho YR, Anbinder AL. An Isolated Phlebolith on the Lip: An Unusual Case and Review of the Literature. Case Rep Pathol. 2015;2015:1-5. [ Links ]
10. Uzun C, Celenk P, van der Stelt PF. Venous malformation with multiple phleboliths: A case report. Quintessence Int (Berl). 2017;48(1):51-6. [ Links ]
11. Altug HA, Büyüksoy V, Okçu KM, Dogan N. Hemangiomas of the head and neck with phleboliths: Clinical features, diagnostic imaging, and treatment of 3 cases. Oral Surgery, Oral Med Oral Pathol Oral Radiol Endodontology. 2007;103(3):60-4. [ Links ]
12. Kanaya H, Saito Y, Gama N, Konno W, Hirabayashi H, Haruna S ichi. Intramuscular hemangioma of masseter muscle with prominent formation of phleboliths: A case report. Auris Nasus Larynx. 2008;35(4):587-91. [ Links ]
13. Ho C, Judson BL, Prasad ML. Vascular malformation with phleboliths involving the parotid gland: A case report with a review of the literature. Ear, Nose Throat J. 2015;94(10-11):E1. [ Links ]
14. Lescura CM, de Andrade BAB, Bezerra KT, Agostini M, Ankha MVA, de Castro F, et al. Oral intramuscular hemangioma: Report of three cases. J Cutan Pathol. 2019;46(8):603-8. [ Links ]
15. Nayak SK, Nayak P. Intramuscular hemangioma of the oral cavity - A case report. J Clin Diagnostic Res. 2014;8(8):41-2. [ Links ]
16. Amin DR, Hegde DP, Shetty DP, Makannavar DJ. Intraoral Venous Malformation With Phleboliths - a Case Report With Review of the Literature. Int J Adv Res. 2017;5(2):663-6. [ Links ]
17. Prakash S, Naik V JD. Multiple Low Flow Vascular Malformation with Phleboliths - A Case Report. J Young Pharm. 2017;9(3):446-50. [ Links ]
18. Blei F. Medical and Genetic Aspects of Vascular Anomalies. Tech Vasc Interv Radiol (Internet). 2013;16(1):2-11. Available from: http://dx.doi.org/10.1053/j.tvir.2013.01.002 [ Links ]
19. Babu D, Bhamre R, Katna R, Pai P. Intramuscular haemangioma of the tongue. Ann R Coll Surg Engl. 2014;96(6):e15-7. [ Links ]
20. Sham ME, Sultana N. Journal of Oral and Maxillofacial Surgery , Medicine , and Pathology Vascular anomalies in maxillofacial region - Review. 2012;24(37):137-46. [ Links ]
21. Hwang MJ, Lee YP, Jin YT, Chiang CP. Granular cell tumor of the tongue: Case report. J Dent Sci (Internet). 2023;18(3):1431-2. Available from: https://doi.org/10.1016/j.jds.2023.04.007 [ Links ]
Conflict of interest statement The authors have no conflict of interest in the publication of the article.
Authorship and contribution statement Conception and design of the study Data acquisition Data analysis Results discussion Manuscript drafting Approval of the final version of the manuscript MNGU has contributed in: 1, 2, 3, 4, 5, 6 NFTC contributed in: 1, 2, 3, 4, 5, 6 CAAD has contributed in: 2, 3, 5, 6 AVBC has contributed in: 1, 2, 3, 4, 5, 6
Received: August 22, 2023; Accepted: November 07, 2023











 texto em
texto em 



