Serviços Personalizados
Journal
Artigo
Links relacionados
Compartilhar
Odontoestomatología
versão impressa ISSN 0797-0374versão On-line ISSN 1688-9339
Odontoestomatología vol.24 no.39 Montevideo jun. 2022 Epub 01-Jun-2022
https://doi.org/10.22592/ode2022n39e409
Case report
Humanized dental care for a patient with neurofibromatosis type 1 in a specialized children’s dental clinic: a case report
1Facultad de Odontología, Universidad de la República. Uruguay.
2Facultad de Odontología, Universidad Federal de Rio Grande do Sul - Porto Alegre, Rio Grande do Sul, Brasil. mcf1958@gmail.com
This paper aims to report an individualized, inclusive, and humanized dental approach, emphasizing the importance of treating a child aged four years and three months with neurofibromatosis type 1. The patient was referred and treated at the Clinic of the Specialization Course in Pediatric Dentistry of the Graduate School, School of Dentistry, Universidad de la República, Montevideo, Uruguay. The clinical examination revealed scars from the surgical treatment of the plexiform neurofibroma and neck and oral muscle hypotonicity. The intraoral clinical examination showed large edentulous areas as 15 deciduous teeth were missing. The patient had active carious lesions, generalized microbial biofilm on the tooth surfaces, and gingival bleeding. A comprehensive treatment was provided, as well as restorative therapy with upper and lower removable partial dentures. We conclude that the dental educational, preventive, restorative, and rehabilitation treatment was satisfactory. Furthermore, empathy, as a dynamic process, involved cognitive, affective, and behavioral mechanisms. It also helped enhance the patient’s oral health.
Keywords: Recklinghause’s disease of the nervous system; mouth; child; maintenance of space; aesthetics; dental prosthesis
Este trabajo tiene como objetivo relatar el abordaje individualizado, inclusivo y humanizado de un niño de 4 años y tres meses, con diagnóstico de neurofibromatosis tipo 1, atendido en la Carrera de Especialización en Odontopediatria de la Escuela de Graduados, Facultad de Odontologı́a, Universidad de la República, Montevideo, Uruguay. En el examen clínico se pudo observar cicatrices derivadas del tratamiento quirúrgico del neurofibroma plexiforme en la zona cervical y la presencia de hipotonicidad muscular oral. Al examen clínico intraoral, se observaron amplias zonas desdentadas a consecuencia de exodoncias de quince dientes deciduos. Presentaba lesiones activas de caries en los dientes remanentes, acompañado de biopelícula generalizada y sangrado gingival provocado. Se realizó un abordaje integral del paciente y la terapia rehabilitadora mediante el uso de prótesis parcial removible superior e inferior. Concluímos que el tratamiento odontológico educativo, preventivo, restaurador y rehabilitador fue satisfactorio y la empatı́a, como proceso dinámico, involucró mecanismos cognitivos, afectivos y conductuales, y fue reconocida por sus efectos positivos en la promoción de la salud bucal del paciente.
Palabras clave: enfermedad nerviosa de Recklinghausen; Cavidad bucal; niño; mantenimiento del espacio; estética; prótesis dental
Este trabalho tem como objetivo relatar uma abordagem odontológica individualizada, inclusiva e humanizada, enfatizando a importância do tratamento de uma criança de 4 anos e três meses, com diagnóstico de neurofibromatose tipo 1, que foi encaminhada e tratada en la clínica de la Carrera de Especialización en Odontopediatria de la Escuela de Graduados, Facultad de Odontología, Universidad de la República. O exame clínico revelou cicatrizes decorrentes do tratamento cirúrgico do neurofibroma plexiforme que acometia o pescoço da criança e hipotonicidade muscular oral. Ao exame clínico intraoral, quinze dentes decíduos estavam ausentes e cinco com lesões de cárie na primeira infância, além de presença generalizada de biofilme microbiano nas superfícies dentais e sangramento gengival provocado. Foi realizado tratamento odontológico necessário ao paciente, com os devidos cuidados e terapia reabilitadora com prótese parcial removível superior e inferior. Concluímos que o tratamento odontológico educacional, preventivo, restaurador e reabilitador foi satisfatório e a empatia, como processo dinâmico, envolveu mecanismos cognitivos, afetivos e comportamentais e foi reconhecida por seus efeitos positivos na promoção da saúde bucal do paciente.
Palavras-chave: doença nervosa de Recklinghausen; cavidade bucal; criança; manutenção do espaço; estética; prótese dentária
Introduction
Neurocutaneous syndromes comprise a heterogeneous group of idiopathic pathologies characterized by alterations of the central nervous system (CNS), and integuments. One of these syndromes is neurofibromatosis (NF), an autosomal dominant disease with variable expression and a progressive multisystem pathology.1,2
This condition includes three autosomal dominant diseases: Neurofibromatosis type 1 (NF1), Neurofibromatosis type 2 (NF2), and Schawannomatosis or Neurofibromatosis type 3. These last two are rare diseases, while Neurofibromatosis type 3 is very rare.3 NF2 is known as bilateral acoustic NF and is characterized by multiple tumors and brain and spinal cord lesions.4 The first symptom is usually the growth of tumors in the auditory nerves resulting in hearing loss.5
NF1 is the most common human dominant genetic disease of the diseases caused by single-gene defects.3 Its prevalence is 1:3000 children born alive,5 which is more frequent than other diseases such as type 1 diabetes mellitus (1:13000)6 or cystic fibrosis (1:10,000).7 The first confirmed case of NF was reported in a 1768 publication, which included the description of a patient with cutaneous neurofibromas, a condition the patient had been inherited from his father. In 1882, the physician Fiedrich Von Recklinhausen described the pathology for the first time, which is why NF1 bears his name. The disease is also known as the “Elephant Man” disease, but this is a historical error since it has been proven that the “Elephant Man” had Proteus syndrome.3
The NF1 gene is located on chromosome 17, band q11.2 and encodes a GTPase-activating protein called “neurofibromin,” with a high expression level in ectodermal tissue (skin, nerves, and bone tissue). Over 500 mutations of this gene have been described. Although diagnosis is based on clinical criteria, molecular tests for the NF1 gene may be useful in some cases.2 The disease has complete penetrance, and its expression is variable, so the degree of involvement of each individual is difficult to predict even in the same family and in cases of identical twins.2,5
NF1 diagnosis is clinical, and in 1988 the specific features were defined by the US National Institute of Health as six or more light brown spots equal to or larger than 5 mm in children; two or more neurofibromas of any type, or one plexiform neurofibroma; freckling in the armpits or the groin; optic nerve glioma; lisch nodules (iris hamartomas); bone lesion defined as sphenoid dysplasia; and a first-degree relative with the disease. Finding two or more of these criteria justifies the diagnosis.2,4). Although these criteria are highly specific in adults, they do not appear in some children under eight years old.8 The disease also presents signs such as macrocephaly, hypertelorism, low-set ears, mild mental retardation, and learning difficulties that are associated with NF1 but are not considered diagnostic criteria.9 However, two common anomalies predominate in preschool children with NF1: short stature and increased head size.10
In summary, NF1 is a multisystemic pathology that can potentially affect the eyes, the musculoskeletal, cardiovascular, endocrine systems, the CNS, and the peripheral system.3 There is no cure for the condition. It is treated by managing symptoms and potential complications, especially those associated with tumor growth. It is estimated that these patients’ life expectancy is about eight years less than that of the general population.11 Between 50% and 80% of patients with the disease may have learning difficulties and behavioral disorders. Thirty percent of children with NF1 may have an ASD, and about 40% may have attention deficit or hyperactivity disorder.11 Voice and oral motor disorders have also been described in children.10
The health personnel should know these oral and maxillofacial manifestations since dentists can be essential to diagnose the disease correctly. Oral manifestations in patients with neurofibromatosis range from 3.8% to 20%. Any part of the oral cavity can be affected. The tongue is the site most frequently affected by neurofibromas, followed by the palate, gums, oral mucosa, floor of the mouth, and labial mucosa more rarely.12
Although not all patients have the most severe clinical or cosmetic complications of the disease, most NF1 patients and their families feel uncertainty about the course and evolution of the disease. This includes new tumors, aesthetic compromise, and potential transmission to their children, which greatly impacts the patients’ quality of life.10
Rezende et al.13) believe that the patient’s well-being is more important than striking a balance between meeting expectations and pain. That is to say, the patient’s well-being should be the starting point of any treatment plan.
This case report describes an individualized, inclusive, and humanized dental approach emphasizing the importance of rehabilitative treatment with preventive maintenance. The patient had NF1 and was treated in 2017 at the Clinic of the Specialization Course in Pediatric Dentistry, School of Dentistry, Universidad de la República, Uruguay.
Clinical case
A male patient aged four years and three months was taken to the Clinic of the Specialization Course in Pediatric Dentistry of the School of Dentistry, University of the Republic by his parents. His usual health center had referred him to assess a potential rehabilitation treatment. The patient’s caretakers signed an informed consent to authorize all the necessary dental procedures, photographs, and the dissemination of the case.
In the medical history, both parents reported that the child was diagnosed with NF1, a disease inherited from his father, who also had the condition. The interview with the parents was not easy because the family’s socioeconomic and education levels are low: they are a vulnerable population, they do not own their house, they are tenants and have electricity and drinking water but no sanitation. Both report dental caries, gum diseases, and missing teeth in their dental histories. The mother has removable dentures.
As for personal medical history, the patient is being treated by physicians to control his condition. Her mother had a normal pregnancy, but the delivery was premature: 34 weeks. The patients’ birth weight was 2 kg 898 g, his height 46 cm, and he was breastfed exclusively until the age of 6 months. Psychomotor maturation was very slow, as he began to sit up at one and walk at two.
Regarding the dental eruption process, his mother reported that a lower incisor erupted at eight months of age. The child was breastfed until the age of two and a half, and he had the deforming habit of lip-sucking.
In terms of oral health habits, the child uses table salt and topical fluoride toothpaste as systemic fluoride. The child brushed his teeth three times a day without adult supervision and followed a cariogenic diet: frequent sugary drinks, foods, and carbohydrates that he consumed between four and up to six times during the day.
The area’s examination showed that the patient presented facial asymmetry, dark circles under his eyes, an everted and large lower lip, reduced muscle tone, and both labial commissures cracked. Upon conducting a functional exam, we detected mixed respiration, altered phonation and mastication due to missing teeth, and atypical swallowing.
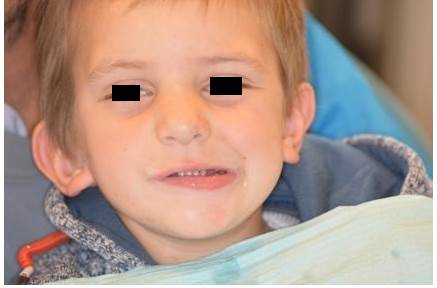
Regarding the clinical signs of NF1, the child had scarring from the surgical treatment of his plexiform neurofibroma, affecting the neck and oral muscular hypotonicity. His cognitive and communication skills were intact. The child was quite shy and had great difficulty relating to others but was cooperative in the clinical visits (Figure 1).
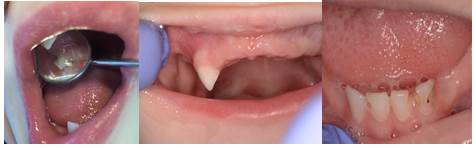
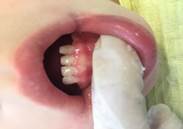
The clinical examination of the oral cavity (Figures 2, 3, and 4) showed no mucosal lesions, 15 temporary teeth missing (55-54-52-51-61-62-63-63-64-65-65-73-73-74-75-83-84-85) and 5 temporary teeth with caries lesions (53-71-72-81-81-82). We also detected biofilm on the tooth surfaces, gingival bleeding on probing, abundant saliva, a voluminous, overflowing, hypotonic tongue, and adhesions and frenulum without peculiarities.
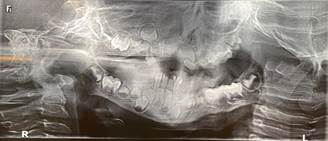
The initial panoramic radiograph (Figure 5) showed many temporary teeth missing, the germs of permanent teeth, and delayed eruption of some teeth, which required follow-up treatment.
Based on the examinations and the diagnosis of the patient’s condition, it was determined that he was a high-risk patient likely to develop new carious lesions. First, an introduction was made to explain prevention and motivational strategies for health education aimed at the child, on an individual basis, and at the entire family. We explained oral hygiene education, the importance of supervising oral brushing in children, provided food advice (a food plan was requested), and explained the use and dosage of fluoride toothpaste.
A dental visit was scheduled to perform the necessary outpatient dental procedures. The teeth with active carious lesions (53-palatal face, 71, 72, 81, and 82-mesial and distal faces) were rehabilitated by removing caries selectively, and the upper and lower removable dentures were made. In each patient visit, biofilm was controlled, and professional brushing was performed with 1450 ppm fluoride toothpaste, emphasizing the importance of brushing in the evening and after main meals to achieve a healthy behavior change. The child and his family were instructed to brush their teeth at least twice a day with 1100 ppm or over fluoride toothpaste. The patient received a hygiene kit with a toothbrush and 1450 ppm fluoride toothpaste.
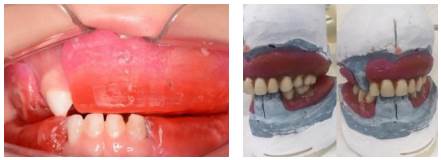
The dental restorations were made with light-curing glass-ionomer cement (FUJI IX GC Corporation) in teeth 53, 71, 72, 81, and 82 (Figure 6). The upper and lower removable dentures for space maintenance were made following the necessary steps: a) taking one-step impressions with heavy and light silicone and casting to obtain plaster models, b) registration plate and impellers, c) occlusal registration and restoration of the vertical dimension, d) dental alignment, e) tooth try-in and f) upper and lower removable dentures (Figures 7, 8, 9, 10, 11, 12, and 13).
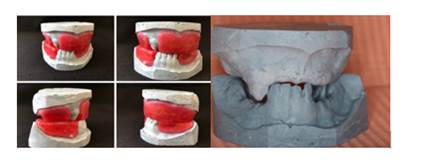
Figures 7 and 8: Taking silicone impressions and making models and plates of registration and impellers
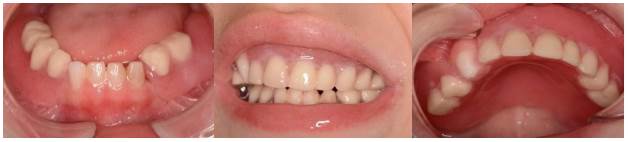
Figures 11, 12, 13: Clinical aspects of the oral cavity with the upper and lower removable dentures in the mouth. Installation

Figure 14: The child’s smile when he returned three months later for evaluation and dental examination
The patient returned for preventive dental check-ups periodically and three months after denture installation to control the infection and the space maintainers (Figure 14).
The boy, who had no intellectual disabilities, showed a positive attitude in all the appointments. The professionals responsible for his dental care used the tell-show-do technique and positive reinforcement. There was no crying or need for physical restraint.
Discussion
Neurofibromatosis types are a group of genetic disorders that cause nerve tissue tumors. These tumors can develop anywhere in the nervous system: the brain, the spinal cord, or the nerves.1,2 Figueiredo et al.14 wrote a clinical case of a girl who had NF1, more specifically plexiform neurofibroma (involvement of several nerve groups). The condition affected the upper eyelid of her right eye and caused ptosis, loss of vision, and facial asymmetry. In addition, she had a younger sister with the same condition. In the case of our patient, the child’s father also had clinical signs of NF1.
Working with the patient’s diet and oral hygiene was challenging. Something noteworthy is the patient’s vulnerability due to his low self-esteem. Brêtas, 2010,15 states that low self-esteem may be due to the individual’s lack of motivation regarding his personal care and thus not finding any reason to take care of himself, even if he is a 4-year-old boy. Improving motivation in the child and his relatives is essential in the care strategy to help identify their basic dental needs and alleviate their suffering.
The treatment proposed included prosthetic rehabilitation to restore function and aesthetics, improve communication and social integration with other people, as this can also be associated with improved self-esteem, confidence, and quality of life. According to Antoniazzi et al., 2018,16 quality of life is related to oral health and includes several dimensions, as it involves health status and social and behavior factors.
In addition, removable partial dentures are essential in these pediatric patients to restore their altered functions and optimize the craniofacial skeletal growth and development of the dentition. This improves mastication, swallowing, phonation, and digestion. However, Prabhakar et al. (17 and Brelaz18 reported the disadvantages of using removable partial dentures and, in some cases, the fact that it may be difficult to adjust them in young patients. This was not the case in this clinical case, as the patient was very cooperative.
As stated by Figueiredo et al. 19 and Gonçalves et al.,20 it is necessary to create a bridge between dentistry and the medical specialties involved in the care of these patients to enable treatment progress. The smile is a cause for aesthetic concern and also a way to recover one’s self-esteem.19,20 In this case, the patient’s smile was restored by making removable partial dentures.
Finally, the dentist providing care to patients with severe NF1 must empathize with them, engage with their clinical history to assess their cognitive profile, and perform procedures according to their ability.14 According to Brazilian Law no. 13.14622 on the inclusion of people with disabilities, health professionals must provide humanized dental care for people with any syndrome and base their work on psychosocial and family interaction.
They must also demonstrate proficiency in the clinical dental procedures, patience, and the enjoyment of caring for a patient with special needs, as these are essential attributes for the care of children in the clinic and to have a successful treatment, as presented in this work.
Clinical relevance and application
This clinical case presents the characteristics of a patient with NF1, in a clear, descriptive, and illustrative manner, without limitations, thus facilitating diagnosis. In addition, it shows adequate preventive, restorative, and rehabilitation treatment, highlighting the importance of the professional’s bond with and commitment to the patient and his family while providing care.
Conclusions
The main oral and general clinical characteristics of the patient reported agreed with what is described in the literature for NF1: poor muscle tone, poor oral hygiene, and active dental carious lesions. This showed the need for dental educational, preventive, restorative, and rehabilitation treatment. Dentists play an essential role in the rehabilitation and well-being of these patients and should be included in a multidisciplinary care team.
It is essential to know the comorbidities of patients with NF1 to manage their dental treatment.
REFERENCES
1. Orozco AJJ, Besson A, Pulido RM, Ruiz RJA, Linares TE, Sa´ez YM R. Neurofibromatosis tipo 1 (NF1). Revisión y presentación de un caso clínico con manifestaciones bucofaciales. Av. Odontoestomatol. 2005 (Fecha de acceso: 29 de julio de 2021); 21(5): 231-239 Disponible en: https://scielo.isciii.es/pdf/odonto/v21n5/original1.pdf [ Links ]
2. Gonzalo M. Neurofibromatosis tipo 1: análisis de características clínicas y tipo de complicaciones en pacientes asistidos en un Hospital de referencia nacional (Monografía de posgrado en Pediatría). (Montevideo): Universidad de la Republica, UdelaR; 2015. 20p. [ Links ]
3. Souza JF, Toledo LL, FerreIra MCM, RodrIgues LOCR, Rezende MA. Neurofibromatose Tipo 1: mais comum e grave do que se imagina. Rev Assoc Med Bras 2009;55(4):394-9. doi: https://doi.org/10.1590/S0104-42302009000400012. [ Links ]
4. Serna FLD, Usuga OAR. Neurofibromatosis:Reporte de un Caso. Rev Fac Odontol Univ Antioq. 2010 (Fecha de acceso: 29 de julio de 2021);21(2):218-225 Disponible en: http://www.scielo.org.co/pdf/rfoua/v21n2/v21n2a10.pdf [ Links ]
5. Sanabria CR, Herna´ndez GAM. Neurofibromatosis Tipo 1 Enfermedad de Von Recklinghausen. Rev Méd Costa Rica Centroamérica, San José. 2014 (Fecha de acceso: 29 de julio de 2021); 71(610):249-252. Disponible en: https://www.medigraphic.com/pdfs/revmedcoscen/rmc-2014/rmc142n.pdf [ Links ]
6. Flor LS, Campo MR. Prevalência de diabetes mellitus e fatores associados na população adulta brasileira: evidências de um inquérito de base populacional. Rev Bras Epidemiol, Rio de Janeiro. 2017; 20(1):16-29. doi:10.1590/1980-5497201700010002 . [ Links ]
7. Athanazio RA, Silva Filho LVRF, Vergara AA, Ribeiro AF, Riedi CA, Procianoy E FA, Melo SFO. Brazilian guidelines for the diagnosis and treatment of cystic fibrosis. J Bras Pneumol, São Paulo. 2017;43(3), 219-245. Doi:10.1590/s1806-37562017000000065 [ Links ]
8. Gómez M, Batista O. Neurofibromatosis tipo 1 (NF1) y su diagnóstico molecular como estrategia del diagnóstico diferencial y a edades tempranas. Rev Med Chile, Santiago. 2015;143(1):1320-1330. Doi: http://dx.doi.org/10.4067/S0034-98872015001000011 [ Links ]
9. Fernández N, Casuriaga AL, Giachetto G. Neurofibroma cervicodorsal en pediatría. Rev AnFaMed UdelaR, Montevideo. 2018;5(1):64-69. Doi: http://dx.doi.org/10.25184/anfamed2018v5n1a3 [ Links ]
10. Mieres PG. Propuesta de Intervención Logopedica en un niño con Neurofibromatosis Tipo I (Tesis de Fin de Grado). (Valladolid): Universidad de Valladolid; 2016. 57p. Disponible en: http://uvadoc.uva.es/handle/10324/19765 [ Links ]
11. Correa MF, Pasik NI. Neurofibromatosis tipos 1 y 2. Rev. Hosp. Ital. Buenos Aires. 2019 (Fecha de acceso: 29 de julio de 2021);39(4):116-127. Disponible en: https://www1.hospitalitaliano.org.ar/multimedia/archivos/noticias_attachs/47/documentos/109202_115-127-HI5-3-19-Correa-B.pdf. [ Links ]
12. Soares MSM, Costa LJ, Aragão MS, Cardoso AB, Gurgel RAS, Passos IB. Neurofibromatose tipo I com manifestação bucal. Odontologia Clin Cientif 2007. Fecha de acceso: 29 de julio de 2021; 6 (1): 91-95 Disponible en: Disponible en: http://www.luzimarteixeira.com.br/wp-content/uploads/2011/02/neurofibromatose-oral.pdf [ Links ]
13. Rezende MCRA, Nascimento MRAN, Lopes E, Gonçalves DA, Zavanelli AC, Fajardo RS. Acolhimento e bem-estar no atendimento odontológico humanizado: o papel da empatia. Arch Health Invest Aracatuba. 2015 (Fecha de acesso: 31 de julio de 2021);4(3):57-61. Disponible en: https://www.archhealthinvestigation.com.br/ArcHI/article/view/904/1190 [ Links ]
14. Figueiredo MC, Potrich ARV, Gouvea DB, Melgar XC. Atencio´n odontolo´gica a paciente pedia´trico con neurofibromatosis tipo 1: relato de caso clínico. Odontoestomatologi´a. 2020;22(36):87-93. Doi: http://dx.doi.org/10.22592/ode2020n36a10. [ Links ]
15. Bre^tas JRS. Vulnerabilidade e adolesce^ncia. Rev Soc Bras Enferm Ped. 2010;10(2):89-96.doi: http://dx.doi.org/10.31508/1676-3793201000011 [ Links ]
16. Antoniazzi RP, Zanatta FB, Ardenghi TM, Feldens CA. The use of crack and other illicit drugs impacts oral health - related quality of life in Brazilians. Oral Diseases. 2018; 24(15):482-488. doi: https://doi.org/10.1111/odi.12786. [ Links ]
17. Prabhakar AR, Sugandhan R, Roopa KB, Akanksha G. Esthetic management of an anterior avulsed tooth: A case report. Int J Clin Pediatr Denti. 2009;2(3):35-8. Doi: 10.5005/jp-journals-10005-1016. [ Links ]
18. Brelaz KLAT,Vena^ncio GN, Almeida MC, Augusto CR. Pro´tese parcial removivel tempora´ria em Odontopediatria: relato de caso. Arch Health Invest. 2016;5(1):13-17. Doi: http://dx.doi.org/10.21270/archi.v5i1.1295 [ Links ]
19. Figueiredo MC, Crispin T, Fontes V, Gouvêa DB, Potrich ARV. Atendimento odontológico ao paciente com Síndrome de Apert: relato de caso. Revista da Associacao Paulista de Cirurgioes Dentistas. 2021(Fecha de acceso: 31 de julio de 2021);75(1):38-44. Disponible en: Disponible en: http://www.sgponline.com.br/apcd/sgp/autor/detalhe_lista.asp?status1=7&status2=0&Tipo=Publicado%20na%20Revista . [ Links ]
20. Gonc¸alves CL, Ju´nior MFS, Andrade LS, Miclos PV, Gomes MJ. Odontologia hospitalar nos hospitais de grande porte da região metropolitana da Grande Vito´ria, Espi´rito Santo. Rev. Bras. Pesq. Saúde, Vitória. 2014;16(1):75-81. [ Links ]
22. República Federativa do Brasil. Lei no 13.146, de 06 de julho de 2015. Institui a Lei Brasileira de Inclusao da Pessoa com Deficie^ncia (Estatuto da Pessoa com Deficiencia) (Internet). Planalto. Brasilia: Diário Oficial da Republica Federativa do Brasil. 2015(Fecha de acceso: 18 de octubre 2021); 1:2. Disponible en: Disponible en: http://www.planalto.gov.br/ ccivil_03/_Ato2015-2018/2015/Lei/L13146.htm [ Links ]
Authorship contribution 1. Conception and design of study 2. Acquisition of data 3. Data analysis 4. Discussion of results 5. Drafting of the manuscript 6. Approval of the final version of the manuscript SFL has contributed in 1, 2, 3, 4, 5. IS has contributed in 1, 2, 3, 4. VG has contributed in 1, 2, 3, 4. LV has contributed in 1, 2, 3, 4. MCF has contributed in 1, 2, 3, 4, 5, 6.
Received: June 13, 2021; Accepted: December 08, 2021











 texto em
texto em