CASO CLÍNICO
Enfisema lobar congénito, caso clínico y revista de la literatura
Congenital lobar emphysema, case report and review of the literature
Ait Idir Karim1, Boutaghane Noureddine2, Amrane Amel3, Slimani Nora4
1. Centro Especializado en Consultaciones Hussein-dey, Argel.
2. Centro Hospital Universitario Mustapha Bacha, Argel. ]]>
3. Centro Hospital Universitario Kouba, Argel.
4. Centro Hospital Universitario Nafissa Hamoud Hussein-Dey, Argel.
Centro Especializado en Consultaciones Hussein-dey Argel
Fecha recibido: 19 de agosto de 2014.
Fecha aprobado: 29 de setiembre de 2014.
Resumen
Las malformaciones congénitas broncopulmonares representan un espectro complejo de anomalías del desarrollo anatómico broncopulmonar. Son infrecuentes, aisladas o asociadas a otras malformaciones. Se pueden revelar tardíamente o en el momento del nacimiento. El enfisema lobar congénito (ELC) se manifiesta a menudo con una dificultad respiratoria temprana en el recién nacido. El diagnóstico, que es esencialmente radiológico, muestra una hiperclaridad que no debemos confundir con otras patologías con hiperclaridad, sobre todo con un neumotórax. En la mayoría de los casos el tratamiento es quirúrgico. Presentamos el caso de un recién nacido hospitalizado desde su segundo día de vida por dificultad respiratoria relacionada con un ELC.
Palabras claves:
ENFISEMA LOBAR CONGéNITO
Summary
The lobar emphysema congenital (LEC) is a rare deformation of the lung and establishes one of the causes of neonatal respiratory distress syndrome. Sometimes, it can be asymptomatic and revealed later. Its origin is undefined in half of the cases. The radiography of the thorax and X-RAY are essential for the diagnosis and treatment.The lobectomy represents the treatment for symptomatic forms. We present the case of a new born child hospitalized in the second day of life for respiratory syndrome in touch with an LEC.
Key words:
EMPHYSEMA LOBAR CONGENITAL
El enfisema lobar congénito (ELC) o hiperinsuflación lobar congénita es una malformación rara del pulmón y constituye una de las causas de las dificultades respiratorias neonatales. A veces es asintomático y se revela más tarde. Su origen está indeterminado en la mitad de los casos. La radiografía del tórax y la tomografía axial computada (TAC) son exámenes indispensables para el diagnóstico y la atención médica. La lobectomía es el tratamiento de elección del ELC sintomático.
Caso clínico
Recién nacido varón. Nacido de una pareja no consanguínea. El embarazo y el nacimiento se desarrollaron sin ningún problema. El peso al nacer fue de 3.450 g, buena adaptación primaria. Vitamina K1 recibida. Meconio y orina emitidos a tiempo. Fue hospitalizado tras una dificultad respiratoria ocurrida a las 36 horas de vida.
]]> El examen de entrada: recién nacido eutrófico, buenas constantes hemodinámicas, saturación de O2 87% bajo el aire, y 92% bajo oxígeno.Buena coloración cutáneo-mucosa, ninguna malformación craneofacial. Dificultad respiratoria con cianosis a la mamada, tiraje intercostal y en la base del tórax. Notamos también una asimetría torácica ligera con alzamiento del hemitórax izquierdo, donde no hay pasaje del murmullo vesicular. Ruidos del corazón bien percibidos pero desplazados a la derecha. El examen neurológico no muestra ninguna anomalía.
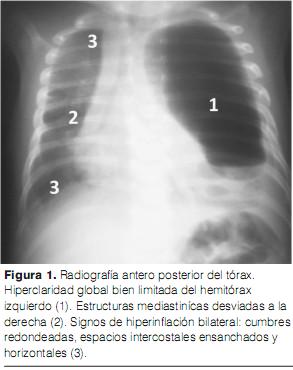
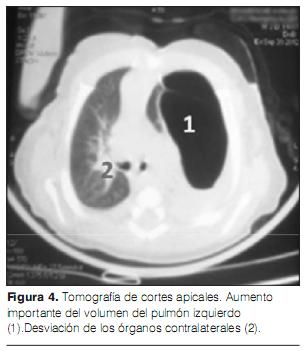
Ante este cuadro clínico, se realizan una radiografía de frente estándar (figura 1) y una TAC torácica (figuras 2, 3 y 4). La ecografía cardiaca y la ecografía abdominal son normales.
Los análisis dieron los siguientes resultados:
Se realizó lobectomía superior izquierda el décimo día de vida, sin ningún problema postoperatorio. La pieza histológica confirmó el diagnóstico. El niño ha sido visto posteriormente, con buen desarrollo psicosomático y sin problemas respiratorios.
Las malformaciones congénitas respiratorias son raras, a veces son asintomáticas, por lo que es difícil evaluar su frecuencia(1). Sobrevienen en menos de un embarazo sobre mil(2). En ciertos casos, un diagnóstico antenatal puede ser realizado(3). Sin embargo, existen algunas malformaciones cuyo diagnóstico antenatal resulta difícil como el del ELC(4,5).Esa dificultad puede explicarse por una parte por el hecho de que el aspecto ecográfico del ELC no es específico y evoca sobre todo las malformaciones adenomatoideas quísticas pulmonares (MAQP). Por otra parte, los signos ecográficos antenatales pueden retroceder incluso desaparecer totalmente al final del embarazo, haciendo que el diagnóstico sea más difícil(6). El ELC o hiperinsuflación lobar congénita corresponde a distensión o hiperinflación de los alvéolos(7-10) histológicamente sanos(11,12). Esta inflación aumenta de modo progresivo según un mecanismo valvular, que produce atrapamiento de aire. Este fenómeno, en la mayoría de los casos, concierne a un lóbulo pulmonar, raramente más(13). Esta malformación puede estar en relación con una obstrucción bronquial extrínseca secundaria a un obstáculo tal como un anillo vascular (2% de los casos) o una obstrucción intrínseca intraluminal (pliegues del epitelio bronquial, estenosis tisular, tapones mucosos) (11,14). Según la teoría de Hislop y Reid, el ELC puede resultar de una anomalía congénita del desarrollo del cartílago del bronquio del lóbulo afectado (15-17).
Otros autores incriminan un desarrollo exagerado del lóbulo de la zona concernida con un número elevado de alvéolos, sin alcanzar el árbol bronquial (17). En este caso se habla más de una patología similar llamada lóbulo polialveolar (18). No obstante, su etiología no se conoce en 50% de los casos (19). El ELC constituiría 14% de las malformaciones pulmonares(6) respectivamente detrás de las MAQP, los quistes broncógenos, y antes de las secuestraciones y digénesis pulmonares(1). Su incidencia es de 1 caso sobre 20.000 o 30.000 nacimientos vivos, con predominio masculino (la razón masculino/femenino es de 3 a 1) (11). El carácter familiar es poco descrito(1). 14%-40% de los casos pueden asociarse a otras malformaciones (renales, diafragmáticas)(11). En 12%-14% de los casos, existe una anomalía cardíaca que debemos buscar (20). La disnea -que a menudo evoluciona en un contexto sin fiebre- constituye el signo clínico más frecuente (1). El cuadro clínico puede ser de gravedad variable: puede manifestarse de golpe con una forma grave o de modo progresivo durante los primeros días o meses de vida. Según los estudios, la revelación del ELC es temprana en las primeras horas en 33% de los casos, en el primer mes en 50% y generalmente antes los 6 primeros meses de vida (1,21).
El examen físico no es específico, se nota distensión de un hemitórax, desplazamiento de los ruidos del corazón en el hemitórax contralateral, timpanismo y abolición del murmullo vesicular en el mismo lado. La gravedad de la sintomatología depende de la importancia del volumen enfisematoso, de la compresión pulmonar adyacente y del grado del desplazamiento de los órganos mediastinales (22).
La radiografía estándar del tórax es un examen esencial en el diagnóstico del ELC. Los signos a favor son hiperclaridad con signos de expulsión contralateral. Hay también signos de hiperinflación como: aspecto redondeado de las cumbres, espacios intercostales horizontales, disminución o aplanamiento de la cúpula diafragmática homolateral.
El TAC torácico es el examen complementario de elección para apoyar el diagnóstico, establecer la topografía exacta y precisar su ubicación así como las características de la distensión pulmonar y excluir también posibles anomalías mediastinales asociadas. El lóbulo afectado aparece bajo la forma de una zona pulmonar sistematizada e hipodensa, con arquitectura pulmonar a menudo conservada. El lóbulo superior izquierdo es el más afectado, seguido por el lóbulo medio derecho y el lóbulo superior derecho, con 41%, 34% y 21% respectivamente. Los lóbulos inferiores raramente padecen con menos de 3% (3,23). También puede asociarse atelectasia de las zonas pulmonares subyacentes. Se han descrito algunos casos de ELC bilateral, pero son extremadamente raros (13,24).

La escintigrafía pulmonar de perfusión y de inhalación se indica en busca de trastornos de ventilación y de perfusión en la zona enferma. También puede aportar información para diferenciar el ELC de un enfisema compensador. Por otro lado, la broncoscopía tiene interés en el caso de una malformación bronquial o también en la busca de un obstáculo. Esta técnica no está libre de riesgo y puede agravar la sintomatología respiratoria.
Los diagnósticos diferenciales que pueden ser evocados son la MAQP (1); neumotórax (en casos de hiperclaridad radiológica y carácter convexo de los límites, a veces se coloca drenaje torácico en una burbuja de ELC confundida con un neumotórax); síndrome de Swyer-James, quiste broncogénico y hernia diafragmática (25-27).
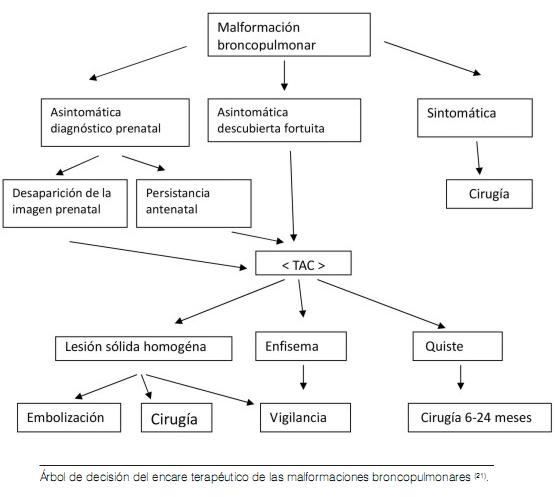
La terapéutica depende de la evolución espontánea de las lesiones, y del carácter sintomático o no. Así, se indica vigilancia estricta clínica y radiológica cuando se trata de un ELC asintomático, sin riesgo vital (respiratorio y/o cardiovascular) (1,11,21) o sobre todo si la exploración broncoscópica es normal (28). En la literatura se describe un caso de seguimiento de un niño con ELC hasta la edad de 17 años (25).
]]> Sin embargo, cuando se trata de un ELC sintomático, una lobectomía por toracotomía y/o toracoscopía con cuidado en reanimación son necesarios (1, 11, 21,28). La evolución es a menudo favorable con expansión pulmonar hasta de 90%. A veces se puede ver hipertensión arterial pulmonar secundaria (25-27).Conclusión
El ELC es una malformación pulmonar rara que puede poner en peligro el pronóstico vital del recién nacido afectado. El diagnóstico es sobre todo radiológico. La TAC torácica informa con precisión las características y topografía de las lesiones. La biopsia confirma el diagnóstico. La lobectomía está indicada cuando el niño es sintomático. En el caso de un paciente asintomático, el manejo conservador es el tratamiento de elección.
Referencias bibliográficas
1. Boussetta K, Aloui Kasbi N, Fitouri Z, Sammoud A, Becher SB, Hammou A, et al. Malformations pulmonaires congénitales : apport de l’imagerie. J Pédiatr Puéric 2004; 17(7):370-9.
2. Hourrier S, Salomon LJ, Bault JP, Dumez Y, Ville Y. Malformations pulmonaires congénitales> diagnostic et prise en charge anténataux. Rev Mal Respir 2011; 28(8):1017-24 .
3. Berteloot L, Bobbio A, Millischer-Bellaiche AE, Lambot K, Breton S, Brunelle F. Malformations pulmonaires congénitales, le point de vue du radiologue. Rev Mal Respir 2012; 29(6):820-35.
4. Olutoye OO, Coleman BG, Hubbard AM, Adzick NS. Prenatal diagnosis and management of congenital lobar emphysema. J Pediatr Surg 2000; 35(5):792-5.
5. Pariente G, Aviram M, Landau D, Hershkovitz R. Prenatal diagnosis of congenital lobar emphysema: case report and review of the literature. J Ultrasound Med 2009; 28(8):1081-4.
6. Konan Blé R, Coste K, Blanc P, Bœuf B, Lecomte B, Labbe A, et al. Une étiologie rare du poumon hyperéchogène: l’emphysème géant congénital. Gynécol Obst Fert 2008; 36(5):529-31.
7. Biyyam DR, Chapman T, Ferguson MR, Deutsch G, Dighe MK. Congenital lung abnormalities: embryologic features, prenatal diagnosis, and postnatal radiologic-pathologic correlation. Radiographics 2010; 30(6):1721-38.
8. Donnelly LF, Frush DP. Localized radiolucent chest lesions in neonates: causes and differentiation. AJR Am J Roentgenol 1999; 172(6):1651-8.
9. Stigers KB, Woodring JH, Kanga JF. The clinical and imaging spectrum of findings in patients with congenital lobar emphysema. Pediatr Pulmonol 1992; 14(3):160-70.
]]>10. Saeedi R, Rahmani S. Congenital lobar emphysema: a case report. Iran J Neonatol 2013; 4(1):36-7.
11. Vásquez RM, Aguirre SC. Enfisema lobar congénito en los lóbulos superiores y medio del pulmon derecho en una paciente de 2 meses. Bol Med Hosp Infant Mex 2011; 68(4):302-7.
12. Andersen JB, Mortensen J, Damgaard K, Skov M, Sparup J, Petersen BL, et al. Fourteen-year-old girl with endobronchial carcinoid tumour presenting with asthma and lobar emphysema. Clin Respir J 2010; 4(2):120-4.
13. Ghribi A, Mekki M, Krichene I, Jouini R, Maazoun K, Sahnoun L, et al. Congenital bilobar emphysema. J Pediatr Surg 2008; 43(8):e5-7.
14. Rothenberg S. Malformaciones pulmonares congénitas: actualización y tratamiento. Rev Méd Clín Condes 2009; 20(6):739-43.
]]>15. Acitores Suz E, Lalinde Fernández M, Lamela Lence MT. Enfisema lobar congénito, causa de dificultad respiratoria en un neonato. Pediatr Aten Prim 2007; 9(33):41-6.
16. Álvarez Muñoz V. Patología torácica quirúrgica en la infancia. Bol Pediatr 2001; 41:131-6.
17. Giudici R, Leào L, Moura L, Wey S, Ferreira R, Crotti P. Polialveolose: patogenese do enfisema lobar congénito? Rev Ass Med Bras 1998; 44(2):99-105.
18. Aldunate RM. Malformaciones pulmonares congénitas. Rev Chil Pediatr 2001; 72(1):52-7.
19. Abdellah O, Mohamed H, Youssef B, Abdelhak B. A case of congenital lobar emphysema in the middle lobe. J Clin Neonatol 2013; 2(3):135-7.
]]>20. Berrocal T, Madrid C, Novo S, Gutiérrez J, Arjonilla A, Gómez-León N. Congenital anomalies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics 2004; 24(1):e17.
21. Khen-Dunlop N, Révillon Y. Malformations congénitales du poumon: quand opérer? Rev Mal Respir 2012; 29(2):328-36.
22. Tempe DK, Virmani S, Javetkar S, Banerjee A, Puri SK, Datt V. Congenital lobar emphysema: pitfalls and management. Ann Card Anaesth 2010; 13(1):53-8.
23. Saghir J, Tasneem S, Khan N. Congenital lobar emphysema. Anaesth Pain Intensive Care 2008; 12(1):16-8.
24. Abushahin AM, Tuffaha AS, Khalil NK, Ismeal AM. Bilateral congenital lobar emphysema: A rare cause for respiratory distress in infancy. Ann Thorac Med 2012; 7(4):250-2.
]]>25. Ozçelik U, Göçmen A, Kiper N, Doðru D, Dilber E, Yalçin EG. Congenital lobar emphysema: evaluation and long-term follow-up of thirty cases at a single enter. Pediatr Pulmonol 2003; 35(5):384-91.
26. Nadeem M, Elnazir B, Greally P. Congenital pulmonary malformation in children. Scientifica (Cairo) 2012; 2012:209896.
27. Mei-Zahav M, Konen O, Manson D, Langer JC. Is congenital lobar emphysema a surgical disease? J Pediatr Surg 2006; 41(6):1058-61.
28. Hermoso Torregrosa C, Moreno Mendinilla E, Pérez Ruiz E, Caro Aguilera PM, Pérez Frías FJ. Hiperinsuflación lobar congénita: manejo conservador como alternativa terapéutica. An Pediátr (Barc) 2014; 81(1):45-8.
Correspondencia: Ait Idir Karim. ]]> Correo electrónico: aitidirkarim@yahoo.fr
]]>