¿Se puede predecir el riesgo de muerte súbita luego de sufrir un infarto de miocardio?
Dres. Gabriel Vanerio Balbela*, Juan Luis Vidal Amaral*,
Pablo Fernández Banizi*, Gustavo López Achigar†, Daniel Banina Aguerre*, Pablo Viana*, Ana Vanerio de León‡, Juan Carlos Bagattini§
Servicio de Arritmias del Centro de Asistencia del Sindicato Médico
del Uruguay-Instituto Nacional de Cirugía Cardíaca. Montevideo, Uruguay
La muerte súbita es responsable de más de la mitad de las muertes debidas a causas cardíacas. Nuestra habilidad para reconocer a los pacientes de alto riesgo de muerte súbita se ha incrementado, pero 90% de las muertes ocurren en sujetos sin factores de riesgo identificables. Además, sabemos que la mayoría tiene enfermedad coronaria preexistente y que la muerte súbita cardíaca es fundamentalmente un problema extrahospitalario. Una población de alta mortalidad y fácil de detectar es la que ya ha sufrido un infarto de miocardio. La mortalidad posinfarto de miocardio oscila entre 5% a 11%, dentro de los seis a 12 meses luego del alta y 20% a los cinco años. Numerosos marcadores se han identificado, pero su valor predictivo positivo es relativamente bajo. El más importante es la disfunción ventricular izquierda. Otras variables: clínicas, basadas en imágenes, autonómicas, electrocardiográficas, además de algunos biomarcadores, métodos invasivos y combinación de variables, se han descripto para estratificar el riesgo y se comentan en este trabajo. Desafortunadamente, aún desconocemos cuál es la combinación que tiene la capacidad predictiva más poderosa. Actualmente, la estratificación del riesgo de muerte súbita se lleva a cabo utilizando solamente la historia clínica, la clase funcional y la fracción de eyección ventricular izquierda (FEVI). En principio, los pacientes de alto riesgo deben recibir betabloqueantes, inhibidores de la enzima convertidora, espironolactona y antitrombóticos. En casos seleccionados se deberá considerar el implante de un cardiodesfibrilador. Otras variables se incorporarán para identificar mejor a los grupos de mayor riesgo.
Palabras clave: Muerte Súbita Cardíaca.
Infarto de Miocardio.
Estratificación de Riesgo.
* Médicos Cardiólogos integrantes del Servicio de Arritmias del Centro de Asistencia del Sindicato Médico del Uruguay.
† Médico Internista colaborador.
‡ Médica Cardióloga colaboradora.
]]> § Médico Internista e Intensivista, Director, Centro de Tratamiento Intensivo del Hospital Británico. Profesor de Medicina. Facultad de MedicinaCorrespondencia: Dr. Gabriel Vanerio
Servicio de Electrofisiología del CASMU-INCC Policlínico CASMU, 8 de Octubre 3310, 2º piso. Montevideo, Uruguay
E-mail: gabvaner@mednet.org.uy
Recibido: 10/2/06.
Aceptado: 7/8/06.
Abreviaturas:
ANP: péptido natriurético auricular
BNP: péptido natriurético cerebral
n-3 PUFA: ácidos grasos poliinsaturados
]]> HF: alta frecuenciaDFA: análisis de fluctuación de tendencia
LF: baja frecuencia
DAE: desfibrilador automático externo
DPV: despolarización prematura ventricular
EBCT: electron beam computed tomography
AER: excreción de albúmina
FEVI: fracción de eyección ventricular izquierda
IM: infarto de miocardio
VLF: muy baja frecuencia
]]> NYHA: New York Heart AssociationPLF: oscilación prevalente de baja frecuencia
BNP: péptidos natriuréticos
PCR: proteína C reactiva ultrasensible
TVNS: taquicardia ventricular no sostenida
MSCT: tomografía computarizada multislice
HRT: turbulencia de la frecuencia cardíaca
ULF: ultrabaja frecuencia
VPN: valor predictivo negativo
VPP: valor predictivo positivo
]]> IntroducciónLa muerte súbita es responsable de más de 14% de todas las muertes (aproximadamente 350.000) que ocurren anualmente en Estados Unidos, y de más de la mitad de las muertes debidas a causas cardiovasculares. Nuestra habilidad para reconocer a los pacientes de alto riesgo de muerte súbita se ha incrementado, pero en 90% de los casos ocurre en sujetos sin factores de riesgo identificables. La mayoría de los pacientes tienen enfermedad coronaria preexistente, y el paro cardíaco es la primera manifestación en 50%(1).
Décadas de experiencia en las unidades de cuidados intensivos han demostrado que la desfibrilación inmediata es el tratamiento más efectivo. Los desfibriladores implantables diseñados para detectar y tratar taquicardia o fibrilación ventricular dentro de los 20 segundos restauran el ritmo sinusal en más de 98% de los episodios.
La muerte súbita cardíaca es fundamentalmente un problema extrahospitalario; aproximadamente 80% de los casos de muerte súbita ocurren en el domicilio. La tasa de éxito de resucitación es baja, promedia 2% a 5% en la mayoría de los centros urbanos. El tiempo que se demora en desfibrilar es el factor más importante de éxito. Cada minuto que se demora, se reducen 8% a 10% las chances de una eventual alta hospitalaria. Por ende, los esfuerzos por resucitar pacientes luego de ocho minutos son ineficaces o están condenados a fallar(1).
En consecuencia, tratar de identificar qué pacientes están en riesgo de morir súbitamente es un objetivo básico. Una población de alta mortalidad y relativamente fácil de detectar es la que ya ha sufrido un infarto de miocardio (IM). A continuación, analizaremos aspectos de la estratificación de riesgo en sujetos que han presentado un IM.
El proceso de estratificación en pacientes posinfarto de miocardio tiene dos componentes: la identificación temprana, intra-hospitalaria, del riesgo de eventos isquémicos recurrentes y la evaluación del riesgo de muerte arrítmica.
Nuestro trabajo se concentrará en la evaluación del riesgo de muerte arrítmica.
Numerosos marcadores han sido identificados para evaluar el riesgo de muerte arrítmica luego de un IM, pero su valor predictivo positivo (VPP) es relativamente bajo. El más importante es la disfunción ventricular izquierda. En la era pretrombolítica, la presencia de arritmia ventricular fue de utilidad, pero, actualmente, la evidencia no es contundente(2-8).
Causas de muerte posinfarto de miocardio
La causa de muerte más frecuente posinfarto de miocardio es la muerte súbita. La muerte súbita cardíaca se define como una muerte natural, precedida por la pérdida brusca de la conciencia dentro de la hora del comienzo de los síntomas, en pacientes con enfermedad conocida preexistente o no, en los cuales el modo y el tiempo de morir son inesperados o no esperados(9-12). La cadena de eventos más aceptada es la taquicardia ventricular, que deriva en fibrilación ventricular y luego en asístole(13,14). En datos de autopsias, la prevalencia de lesiones coronarias es variable, pero la isquemia miocárdica es la causa más importante(15,16). La prevalencia de enfermedad coronaria fue de 54% en sujetos que experimentaron muerte súbita(17). En la era pretrombolítica, los síntomas de isquemia eran los que precedían a la muerte súbita en 60% de los pacientes(18). La isquemia miocárdica aguda continúa siendo el disparador más frecuente de arritmias fatales.
]]> En el Maastricht Circulatory Arrest Registry, en un lapso de cuatro años, se analizaron 492 casos de muerte súbita cardíaca(19). En más de 50%, la muerte súbita fue la primera manifestación de enfermedad cardíaca. En el grupo con enfermedad cardíaca previa conocida, 77% presentaba enfermedad coronaria (de ellos, 66% ya había sufrido al menos un IM previo)(19).En relación con el tipo de IM no hay diferencias significativas: los pacientes con un infarto no Q, tienen la misma morbilidad y mortalidad que aquellos con IM Q(20).
La muerte súbita puede ocurrir por causas no arrítmicas: embolismo pulmonar masivo, complicaciones mecánicas luego del infarto (cercanas en el tiempo al IM), y la ruptura de un aneurisma de la aorta abdominal. En el grupo de pacientes con falla congestiva severa por enfermedad coronaria [fracción de eyección menor a 30%, y clase funcional II-IV de la New York Heart Association (NYHA)] el reinfarto es, probablemente, el responsable de la muerte súbita. Debe tenerse en cuenta que las arritmias pueden provocar muerte no instantánea (por ejemplo, un síncope arrítmico puede inducir daños o lesiones posteriormente fatales).
Mortalidad después del infarto de miocardio
La mortalidad después del IM ha disminuido en las últimas décadas, pero aún se mantiene elevada, oscilando entre 5% a 11% dentro de los seis a 12 meses luego del alta. La mayoría de las muertes se producen cuando el paciente comienza con síntomas y durante las fases iniciales de la hospitalización. En un seguimiento de cinco años, la mortalidad alcanza 20%(21). En registros españoles donde se estudiaron 28.357 y 6.221 sujetos con IM a fines de la década de 1990, 71% de los pacientes recibieron tratamiento de reperfusión, la mortalidad aguda fue de 9%. A los 28 y 365 días fue de 11,4% y 16,5%, respectivamente(22,23).
Hay diferencias muy importantes en relación con el sexo y la edad. Las mujeres tienen una mortalidad mayor que los hombres en los primeros 30 días (28% versus 17%)(24). La edad de los pacientes es un factor muy importante en la mortalidad: 60% de los pacientes con IM son mayores de 65 años; 80% de las muertes posinfarto de miocardio pertenecen a este grupo. Los pacientes de edad avanzada poseen mayor comorbilidad, tasas de mortalidad más elevadas, y muchos se benefician de un tratamiento agresivo. A pesar de esto, los pacientes adultos mayores reciben menos beta-bloqueantes, ácido acetilsalicílico y menor cantidad de intervenciones terapéuticas(25).
En el registro de Medicare (Estados Unidos) de 1992, se analizaron 190.000 pacientes añosos con IM(26). En este estudio se observó una mortalidad diferente según la edad del paciente(27,28). En el grupo de 65 a 74 años, la mortalidad hospitalaria y la mortalidad a 30 y 360 días fue de 13,7%, 15,1%, y 24,9%, respectivamente. En cambio, en el grupo con más de 74 años, la misma mortalidad fue de 22,9%, 26% y 43,6%, respectivamente(26,27). En estudios randomizados (comparando amiodarona y placebo) de pacientes de alto riesgo (función ventricular izquierda disminuida e inestabilidad eléctrica), la mortalidad no arrítmica en el grupo placebo osciló entre 5% a 6% a los dos años y la arrítmica 2% a 6% en el mismo plazo(28-30). El estudio ALIVE incluyó 3.700 pacientes de alto riesgo de muerte súbita después del IM [fracción de eyección ventricular izquierda (FEVI) 15% a 35%]. Con fines de estratificación se usó, además, el índice triangular, una medida de variabilidad de la frecuencia cardíaca.
La tasa de mortalidad global de los pacientes con variabilidad normal fue de 9,5% durante el año de duración del estudio. Los pacientes con variabilidad disminuida tuvieron una mortalidad de 15%. El simple agregado del índice triangular logró distinguir mejor al grupo de alto riesgo, independientemente de otras características basales (por ejemplo, función ventricular izquierda, sexo, clase funcional NYHA)(31,32).
En muchos casos, la muerte súbita ocurre en los primeros seis a 18 meses después del IM(10,33-35). En el estudio MADIT, el beneficio del desfibrilador no se observó sino después de los nueve meses del implante(36-38), o más allá de los 18 meses(39). El estudio DINAMIT demostró que el implante profiláctico del desfibrilador en el posinfarto de miocardio temprano no determinaba un aumento en la sobrevida(40).
Mortalidad en Uruguay
]]> En Uruguay, las enfermedades cardiovasculares son responsables de 33% de las muertes y ese porcentaje se ha mantenido relativamente estable desde 1999 a 2003. En números absolutos, son aproximadamente 10.000 muertes por año. En el año 2003, murieron 8.400 pacientes con más de 70 años; 2.032 sujetos entre 50 y 69 años y 355 con menos de 49 años(41).No tenemos datos del número de IM o de muerte súbita, pero si extrapolamos información de países similares al nuestro, dado que la muerte súbita es responsable de 15% de todas las muertes, en Uruguay resultarían 1.500 a 2.000 por año. Estos comentarios enfatizan la importancia de establecer un registro obligatorio para pacientes con IM, así como de muerte súbita, como ocurre con las enfermedades infecciosas transmisibles.
A. Tipo de arritmias
Si una arteria coronaria se ocluye bruscamente, la isquemia puede provocar fibrilación ventricular, bradicardia, asístole o bloqueo auriculoventricular. Luego de un IM, las arritmias que provocan la muerte súbita son taquiarritmias y, en menor proporción, bradiarritmias. Las bradiarritmias se observan en pacientes con enfermedad cardíaca más avanzada. En varios reportes la muerte súbita por bradiarritmia alcanzó 15% a 20% de la población general(8,11,12,25). En un análisis de siete series de Holter de 24 horas, se describieron 157 casos: la fibrilación ventricular fue responsable de 62% de las muertes; la taquicardia ventricular de 8%; "torsade de pointes", 13% y bradiarritmias, 16%(42).
B. Mecanismos de arritmias ventriculares después del IM
Las taquiarritmias ventriculares se generan por tres mecanismos básicos: actividad gatillada, automatismo o reentrada. El modelo más aceptado incluye un sustrato (fibrosis o la misma cicatriz del infarto), factores moduladores o eventos iniciadores transitorios (por ejemplo, disturbios del tono autonómico, disbalance electrolítico, acidosis, isquemia, efecto de drogas y factores endocrinos o psicosociales). Finalmente, el factor disparador suele ser una despolarización prematura ventricular (DPV) o variaciones bruscas de la frecuencia cardíaca. El sustrato y los factores moduladores son responsables por la inestabilidad de la membrana miocárdica(10). La sobrecarga de volumen puede producir estiramiento, enlentecer la conducción, alterar el período refractario ventricular, gatillar pospotenciales y generar despolarizaciones ventriculares ectópicas(43,44).
Estratificación de riesgo posinfarto de miocardio
Disponer de pruebas o estudios que identifiquen qué pacientes están en riesgo de morir en los próximos meses posinfarto de miocardio es esencial. Una prueba ideal debería ser no invasiva, barata, fácil de realizar y analizar después del alta hospitalaria.
A continuación analizaremos diferentes variables, todas útiles para estratificar el riesgo de presentar una muerte súbita posinfarto de miocardio. Dividiremos las variables en: clínicas, basadas en imágenes, marcadores autonómicos, electrocardiográficas, biomarcadores, métodos invasivos y, finalmente, combinación de variables.
1) Variables clínicas
]]> En numerosas series de pacientes posinfarto de miocardio, la mortalidad está relacionada con los factores de riesgo habituales, que incluyen hipercolesterolemia, hipertensión, tabaquismo, sedentarismo, etc. En un reciente metaanálisis del "brazo placebo" de los estudios EMIAT, CAMIAT, SWORD, TRACE y DIAMOND se detectaron: edad avanzada, historia de IM previo(45), que refleja mayor extensión de daño miocárdico, angina, e hipertensión arterial, asociadas a un incremento de la mortalidad global y arrítmica. La diabetes se asoció con la mortalidad global, y el sexo masculino con mortalidad arrítmica(11). Los eventos arrítmicos se observaron preferentemente en pacientes mayores de 70 años o con historia de diabetes o falla congestiva previa(28).Una historia familiar de muerte súbita prematura asociada a enfermedad coronaria es otro factor de mal pronóstico(46-48).
Los pacientes con edema pulmonar durante la internación tienen un incremento de eventos arrítmicos. Los que sufren de arritmias malignas (taquicardia ventricular o fibrilación ventricular) que provocan síncope o que han sido resucitados de un paro cardíaco más de 48 horas posinfarto de miocardio, se encuentran en alto riesgo de muerte súbita (antes debe descartarse isquemia reversible)(45).
La clase funcional según la NYHA ha probado tener un buen valor predictivo.
La mortalidad por todas las causas se incrementa de acuerdo con la clase funcional(11,25). En pacientes con clase funcional II-III la probabilidad de muerte súbita es alta; es menos importante en los pacientes en clase funcional IV, donde la principal causa de muerte es la progresión de la insuficiencia cardíaca(11,25).
La terapia trombolítica y la angioplastia primaria se asocian con reducción de mortalidad por todas las causas y, también, con menor incidencia de arritmias(45).
La presencia de insuficiencia renal severa y anemia son factores independientes de mortalidad(49,50).
2) Basadas en imágenes - Indicadores de daño miocárdico
a) Fracción de eyección ventricular izquierda
La disminución de la fracción ventricular izquierda es el índice más utilizado y debe ser determinado en todos los pacientes que sufrieron un IM(51). La función sistólica puede ser evaluada por ecocardiografía, ventriculografía o centellografía. La función ventricular sistólica disminuida es el factor de riesgo más importante para predecir la mortalidad total y súbita(2,45). La FEVI aislada tiene un VPP bajo (11%-22%) y un valor predictivo negativo (VPN) elevado (96%-98%)(52). La función ventricular izquierda también es un predictor de eventos arrítmicos tras un IM. De hecho, los pacientes con FEVI severamente deprimida mueren súbitamente en un tercio de los casos y, en ellos, la incidencia de taquiarritmias ventriculares es mayor(35,52). La sensibilidad, la especificidad, el VPP y el VPN de la FEVI para la detección de eventos arrítmicos es de 56%-71%, 74%-83%, 11%-22% y 96%-98%, respectivamente(52).
]]> En el metaanálisis de los estudios EMIAT, CAMIAT, SWORD, TRACE y DIAMOND se demostró que una fracción de eyección menor a 20% tenía una mortalidad arrítmica de 9,4%. Si estaba entre 21% y 30%, era de 7,7%; y de 3,2% si era mayor a 30%(11,12). En el brazo terapéutico del estudio SAVE se estudiaron 1.115 pacientes con fracción de eyección menor a 40%. La mortalidad fue de 20% a los 3,5 años, y la mitad se clasificó como súbita (53-56).Gosselink y colaboradores(57) analizaron pacientes tratados con trombolisis o angioplastia primaria. La mortalidad a 30 meses fue 16%, si la FEVI era menor de 40%, frente a 2%, si la FEVI era mayor de 40%. Cuando se acompañaba de signos clínicos y radiológicos de falla cardíaca congestiva, el pronóstico era significativamente peor. En el estudio de Nicod y colaboradores(58), los pacientes con FEVI igual a 40% y clínica de insuficiencia cardíaca durante el ingreso presentaron una mortalidad al año de 26% versus 12% en casos con la misma FEVI, pero sin esa clínica. Estas diferencias también se cumplían si la FEVI era 41%-50% o mayor de 50% (19% versus 6%; y 8% versus 3%, respectivamente).
El estudio MADIT 2 incluyó 1.232 pacientes posinfarto de miocardio con fracción de eyección menor de 30%. Demostró una reducción de 31% (IC95% 0,07-0,49) en la mortalidad global en los pacientes que recibieron un desfibrilador. No se observó beneficio del desfibrilador en pacientes con fracción de eyección menor de 25%(59,60).
b) Volumen ventricular
La remodelación del ventrículo izquierdo luego del IM depende de varios factores, los más importantes son el tamaño y la localización del IM y el tiempo hasta la restauración del flujo en la arteria ocluida. Pequeños incrementos del diámetro ventricular izquierdo están asociados con aumento de la mortalidad. El diámetro de fin de sístole ha demostrado ser un índice poderoso, mejor incluso que la anatomía coronaria o la fracción de eyección.(61-65)
c) Evaluación no invasiva de calcificaciones coronarias
Nuevas técnicas desarrolladas en la última década para evaluar la aterosclerosis de forma no invasiva pueden tener lugar en el proceso de estratificación primaria o secundaria. Estas incluyen la tomografía computarizada con rayo de electrones (electron beam computed tomography, EBCT), la tomografía computarizada multislice (MSCT) y la resonancia nuclear magnética. En muchos casos se utilizan para detectar enfermedad arterial coronaria subclínica precoz. La extensión de las calcificaciones coronarias predice eventos cardiovasculares futuros en pacientes sintomáticos y posee mayor valor pronóstico que la coronariografía(66,67). Aun más, hay una correlación directa entre niveles progresivos de calcio coronario y el desarrollo de eventos cardíacos subsecuentes. Numerosos estudios prospectivos randomizados han establecido el VPP de las calcificaciones coronarias para eventos coronarios futuros en individuos asintomáticos(68-76). Raggi y colaboradores, demostraron que un score de calcio elevado (igual a 1.000) en EBCT en sujetos asintomáticos conlleva un riesgo elevado de eventos cardíacos (muerte o IM) en el corto plazo (25% por año)(75).
3) Marcadores autonómicos
La frecuencia cardíaca, la variabilidad de la frecuencia cardíaca y la sensibilidad barorrefleja son marcadores del balance simpático-vagal. Un aumento de la actividad simpática o una disminución de la parasimpática están asociados con un incremento del riesgo de eventos adversos posinfarto de miocardio(12).
a) Frecuencia cardíaca
]]> La frecuencia cardíaca media se correlaciona con la variabilidad de la misma. Una frecuencia cardíaca elevada es un factor de riesgo independiente de muerte súbita en la población general e indica un incremento de la actividad simpática y pérdida de la parasimpática. Una frecuencia cardíaca elevada es un indicador de disfunción ventricular o de manejo inadecuado de los betabloqueantes. En un seguimiento de ocho años, una frecuencia cardíaca mayor de 90 ciclos por minuto se asoció a un aumento de la mortalidad por muerte súbita cinco veces mayor que cuando se comparó con pacientes con frecuencia cardíaca menor a 60 por minuto(77). En el estudio GISSI 2, con 7.831 pacientes, la frecuencia cardíaca al alta predijo en forma independiente la mortalidad total a los seis meses luego del IM. La mortalidad fue 0,6%, si la frecuencia era menor de 60 pm, comparada contra 14%, si la frecuencia cardíaca era mayor de 100 ciclos por minuto(78).b) Variabilidad de la frecuencia cardíaca
La variabilidad de la frecuencia cardíaca es un fenómeno fisiológico derivado de la variación de los intervalos RR normales durante el ritmo sinusal normal.
La variabilidad de la frecuencia cardíaca en el dominio del tiempo se basa en métodos estadísticos simples. El SDNN corresponde al desvío estándar de los intervalos RR normales o NN, en milisegundos, en estudio Holter de 24 horas. Kleiger y colaboradores, en 1987, demostraron que un SDNN menor a 50 ms, se asoció con un incremento de la mortalidad de 5,3 veces, comparado con pacientes con un SDNN mayor de 100 ms(3). En el estudio Zutphen, el grupo con SDNN menor a 70 ms mostró una mortalidad más elevada a los cinco años(79).
En el estudio GISSI-2 se utilizó un SDNN menor de 70 ms para predecir mortalidad total (riesgo relativo 3, IC 95% 1,5-5,9) y mortalidad cardiovascular (riesgo relativo 2,6, IC95% 1,3-5,3)(80). En el estudio ATRAMI, un SDNN menor de 70 ms mostró un riesgo relativo de 3,2, (IC95% 1,42-7,36) durante un período de seguimiento de 21 meses en 1.284 pacientes(4-6).
El análisis espectral de la frecuencia cardíaca utiliza los componentes de ultrabaja frecuencia (ULF), de muy baja frecuencia (VLF), de baja frecuencia (LF), y de alta frecuencia (HF) del espectro de la frecuencia cardíaca. El balance entre el componente de baja y alta frecuencia (LF/HF) se usó en un subestudio de GUSTO 1 y demostró que una relación LF/HF menor a 1,2 en 24 horas, era un poderoso predictor de mortalidad global(81).
Otros marcadores autonómicos incluyen el índice triangular(82,83), que corresponde a la integral de la densidad de distribución (de todos los intervalos normales en Holter de 24 horas). Un valor menor de 20 unidades es anormal.
c) Sensibilidad barorrefleja
Es un método que mide el balance neuroautonómico. El estudio ATRAMI (estudio del tono autonómico reflejo luego del IM), demostró que una sensibilidad barorrefleja disminuida (menor de 3 milisegundos/mmHg) medida dentro de los 28 días posinfarto de miocardio, predijo la mortalidad cardíaca con un riesgo relativo de 2,8 (IC95%, 1,24-6,16) en una muestra de 1.284 pacientes durante un seguimiento de 21 meses(84). En mayores de 65 años, el valor pronóstico de la sensibilidad barorrefleja fue menor(5,6,84). En un porcentaje variable de pacientes posinfarto de miocardio no se puede realizar porque es dependiente de un ritmo regular estable (no se puede usar en fibrilación atrial o si hay actividad ectópica ventricular frecuente, o en pacientes con mala circulación periférica).
d) Turbulencia de la frecuencia cardíaca (HRT)
]]> Este método analiza el comportamiento de la frecuencia cardíaca luego de una despolarización ventricular prematura, en registros Holter de 24 horas. La turbulencia tiene dos parámetros, el comienzo de la turbulencia (turbulence onset), y la pendiente de la turbulencia (turbulence slope). En varios estudios recientes la alteración de ambos parámetros fue el predictor más poderoso de muerte total (riesgo relativo 5,9; IC95% 2,9-12), aun mejor que la FEVI(5,6,85-92). La turbulencia se correlaciona con la sensibilidad barorrefleja y representa también a la actividad vagal. La HRT se ve influenciada por la edad y la función ventricular. Los diabéticos tienen una HRT con más alteraciones que los no diabéticos(93).e) Oscilación prevalente de baja frecuencia (PLF)
Corresponde a la frecuencia de los picos detectados en el espectro de la frecuencia cardíaca en intervalos de 5 min, del componente LF sometidos a una promediación. Analizando las poblaciones de EMIAT y ATRAMI, fue la única variable, además de la FEVI, con un riesgo relativo de 3,6 (IC95%, 1,3-10,5), comparándolo con la sensibilidad barorrefleja, intervalo RR medio, SDNN, LF, HF y HRT(94).
f) Métodos dinámicos no lineales:
análisis de fluctuación de tendencia (DFA)
Esta técnica determina las propiedades de repetición o "fractales" de la frecuencia cardíaca (se refiere a la regularidad de la señal, cuán predecible es su comportamiento). Con respecto a los otros métodos descriptos más arriba, tiene ventajas considerables, es independiente o insensible a los efectos del ruido y de señales no estacionarias. Además, permite analizar los intervalos RR en pacientes con actividad ectópica frecuente. En una población con disfunción ventricular izquierda, una disminución del componente de corto tiempo ha demostrado ser un potente predictor de mortalidad cardíaca y total(95-97).
Una variable que se obtiene con esta técnica es la "entropía" aproximada (medida cuantitativa de la regularidad de los intervalos RR) que refleja la complejidad de la señal, mientras más impredecible o más compleja la señal, mayor será el valor de la "entropía" y menor el riesgo de muerte(98).
4) Electrocardiogafía
a) Anormalidades en la conducción atrioventricular o intraventricular
La medida de duración del intervalo QRS en el electrocardiograma de 12 derivaciones es un método simple y barato. En el estudio MADIT 2 se demostró beneficio del uso del desfibrilador si la duración del QRS era mayor de 120 ms(36,59,99). En pacientes con IM de cara anterior, la presencia de anormalidades de la conducción intraventricular (excepto el hemibloqueo anterior-izquierdo), esta asociada con un pronóstico desfavorable. Estos sujetos tienen un incremento de riesgo de muerte súbita y cardíaca, en parte por progresión hacia bloqueo auriculoventricular completo, pero más importante, secundario a taquiarritmias ventriculares(100,101).
]]> Los trastornos del segmento ST, sobre todo en la región lateral y anormalidades atriales cinco a siete días después del infarto, fueron predictores dependientes de muerte cardíaca en un estudio de Perkiomaki y colaboradores, que incluyó 1.034 pacientes con un seguimiento de dos años(102).El estudio Zutphen demostró que pequeñas variaciones de la onda T o del intervalo ST-T son de utilidad para predecir eventos futuros(79,103).
b) Electrocardiografía ambulatoria
Los primeros estudios con Holter de 24 horas se realizaron en la época pretrombolítica, donde se contaba el número de complejos prematuros ventriculares. Se ha utilizado como punto de corte diez o más extrasístoles por hora. En la era trombolítica, el estudio GISSI 2 incluyó 8.676 pacientes; 19,7% tenía más de diez extrasístoles ventriculares por hora. Luego de ajustar por factores de riesgo, un aumento de la actividad ectópica fue un predictor significativo de mortalidad a seis meses, con un riesgo relativo de 1,6 (IC95% 1,16-2,26) y de muerte súbita con un riesgo relativo de 2,24 (IC95% 1,22-4,08)(7), grupo del Hospital St George's de Londres, estudio de 680 sujetos, seis a diez días después de sufrir un IM, observaron que el número de extrasístoles ventriculares fue mayor en los pacientes que murieron súbitamente por causas cardíacas(104). También permitió detectar qué pacientes tuvieron más eventos arrítmicos durante el primer año de seguimiento. El VPP fue mayor en pacientes que recibieron trombolisis(104).
c) Taquicardia ventricular no sostenida (TVNS) y taquicardia ventricular sostenida
La TVNS se define como tres o más despolarizaciones consecutivas a una frecuencia superior a 100 por minuto, que termina espontáneamente y dura menos de 30 segundos. En la era trombolítica el valor de la TVNS es controversial. En el estudio GISSI 2 se observó la TVNS en 6,8% de los pacientes y su presencia no cambió el pronóstico, riesgo relativo 1,2 (IC95% 0,8-1,79)(7). En otro trabajo, la TVNS fue un marcador de riesgo en pacientes que no recibieron tratamiento de reperfusión(8). En un estudio de 325 pacientes posinfarto de miocardio, la prevalencia de la taquicardia ventricular sostenida fue 9%. La TVNS anunció taquicardia ventricular sostenida o fibrilación ventricular, pero en forma no independiente(33). Sin embargo, pacientes posinfarto de miocardio con TVNS, mala función ventricular y taquicardia ventricular inducible en el estudio electrofisiológico tienen un alto riesgo de muerte súbita(105). Los pacientes con taquicardia ventricular sintomática y taquicardia ventricular hemodinámicamente estable durante el estudio electrofisiológico representan un grupo de alto riesgo demostrado en los estudios CIDS(106,107) y AVID(108-111).
d) Prueba de esfuerzo
Sus principales indicaciones son evaluar el riesgo y pronóstico, además de medir la capacidad funcional. Se destacan dos hallazgos:
1. Isquemia inducida por el esfuerzo.
2. Arritmias ventriculares durante la prueba de esfuerzo.
La incompetencia cronotrópica durante el esfuerzo se ha relacionado con un aumento de la mortalidad en varias poblaciones(115-117). La pérdida de una respuesta apropiada de la presión arterial sistólica(118,119) y un "doble producto" bajo también están asociados con un pronóstico adverso(120).
Otro índice de utilidad es la recuperación de la frecuencia cardíaca después del ejercicio(121,122). Durante el ejercicio se incrementan el tono simpático y las catecolaminas plasmáticas. El aumento de la frecuencia cardíaca que acompaña al ejercicio se debe en parte a la reducción del tono vagal. La recuperación de la frecuencia cardíaca posesfuerzo depende de la reactivación vagal. Se define como respuesta anormal para la recuperación de la frecuencia cardíaca una reducción menor de 12 ciclos por minuto en el primer minuto posesfuerzo. En un seguimiento de seis años a 2.428 adultos, (57±12 años; 63% hombres), 26% tenía valores anormales. Demostró ser un predictor poderoso de mortalidad global (riesgo relativo 4,0; IC95% 3,0-5,2)(122).
e) Electrocardiograma de promediación de señales
La presencia de potenciales de baja amplitud al final del complejo QRS, o de potenciales tardíos detectados en un electrocardiograma (ECG) de alta resolución por la promediación de señales, refleja heterogeneidad en la repolarización ventricular(123,124). Los potenciales tardíos representan el sustrato para desarrollar taquiarritmias ventriculares. Parece predecir mejor el desarrollo de taquicardia ventricular sostenida que de fibrilación ventricular(125).
En la era pretrombolítica, la presencia de potenciales tardíos se asociaba con eventos adversos(126). En un meta-análisis, un estudio anormal tenía un riesgo seis veces mayor para desarrollar taquicardia ventricular sostenida y muerte súbita si la función ventricular era anormal(127). En varios estudios el VPP ha bajado, probablemente por los tratamientos de reperfusión y revascularización miocárdica. Pero el VPN se mantiene alto(128-130). En un subestudio del CAST, el VPP de la promediación de señales fue 21% para pacientes con arritmias ventriculares y un VPN de 97%(131). La duración del complejo QRS promediado se ha sugerido como el factor predictivo más importante(131). Si la arteria relacionada con el infarto está ocluida, la promedia-ción de señales anormales parece tener más valor(132).
f) Microalternancia de la onda T
La alternancia de la onda T (T wave alternance) es un fenómeno fisiológico y patológico. La alternancia macroscópica de la onda T se ha asociado con arritmias malignas, pero recientemente la microalternancia de la onda T (medida en microvoltios) ha demostrado ser un poderoso predictor de mortalidad posinfarto de miocardio(133-135). Esta técnica no está disponible en nuestro medio.
5) Biomarcadores
a) Péptidos natriuréticos (BNP)
]]> La determinación del BNP y el ANP parecen ser de utilidad en la estratificación de riesgo(136-142). Retterstol y colaboradores analizaron 247 pacientes posinfarto de miocardio, la medida del ANP predijo la mortalidad a largo plazo luego de diez años de seguimiento(143).El BNP parece agregar mayor información pronóstica, independiente de otras variables. Se ha demostrado que pacientes con falla cardíaca congestiva, fracción de eyección menor de 35%, y un BNP elevado (pero no el ANP), predice muerte súbita cardíaca (punto de corte: 130 pg/ml, VPP 19% y VPN de 99%)(144). En este estudio, una cantidad pequeña de pacientes recibía betabloqueantes, 18% en el grupo que murieron y 33% en el grupo que sobrevivieron(144).
El uso combinado de BNP elevado y FEVI menor de 40% fue un poderoso predictor de eventos a tres años, incluyendo muerte, falla cardíaca, e IM (37%, 18% y 26%, respectivamente)(145).
b) Proteína C reactiva ultrasensible (PCR) y otros marcadores
La determinación de la PCR parece ser un estudio valioso para estimar el riesgo posinfarto de miocardio(146-149). Marfella y colaboradores describen los efectos de la hiperglicemia por estrés que genera inflamación y disfunción ventricular izquierda durante las primeras etapas del IM (150).
Otro marcador de inflamación, como la tasa de excreción de albúmina (AER), parece ser también de utilidad(151).
6) Estratificación invasiva - Estudio electrofisiológico
El estudio electrofisiológico es un método invasivo que evalúa el riesgo de desarrollar arritmias malignas. No se utiliza en forma rutinaria por razones de disponibilidad y costos. El estudio MADIT 1 y el estudio MUSTT (Multi-center Unsustained Tachycardia Trial) demostraron el beneficio de realizar un estudio electrofisiológico en pacientes con taquicardia ventricular no sostenida y fracción de eyección menor de 35%-40%(56,152,153). Los pacientes con enfermedad coronaria, disfunción ventricular izquierda asintomática, y taquicardia ventricular no sostenida, en quienes no se pudo inducir taquiarritmia ventricular sostenida en el estudio electrofisiológico, tuvieron una mortalidad global a cinco años menor que los pacientes inducibles(154).
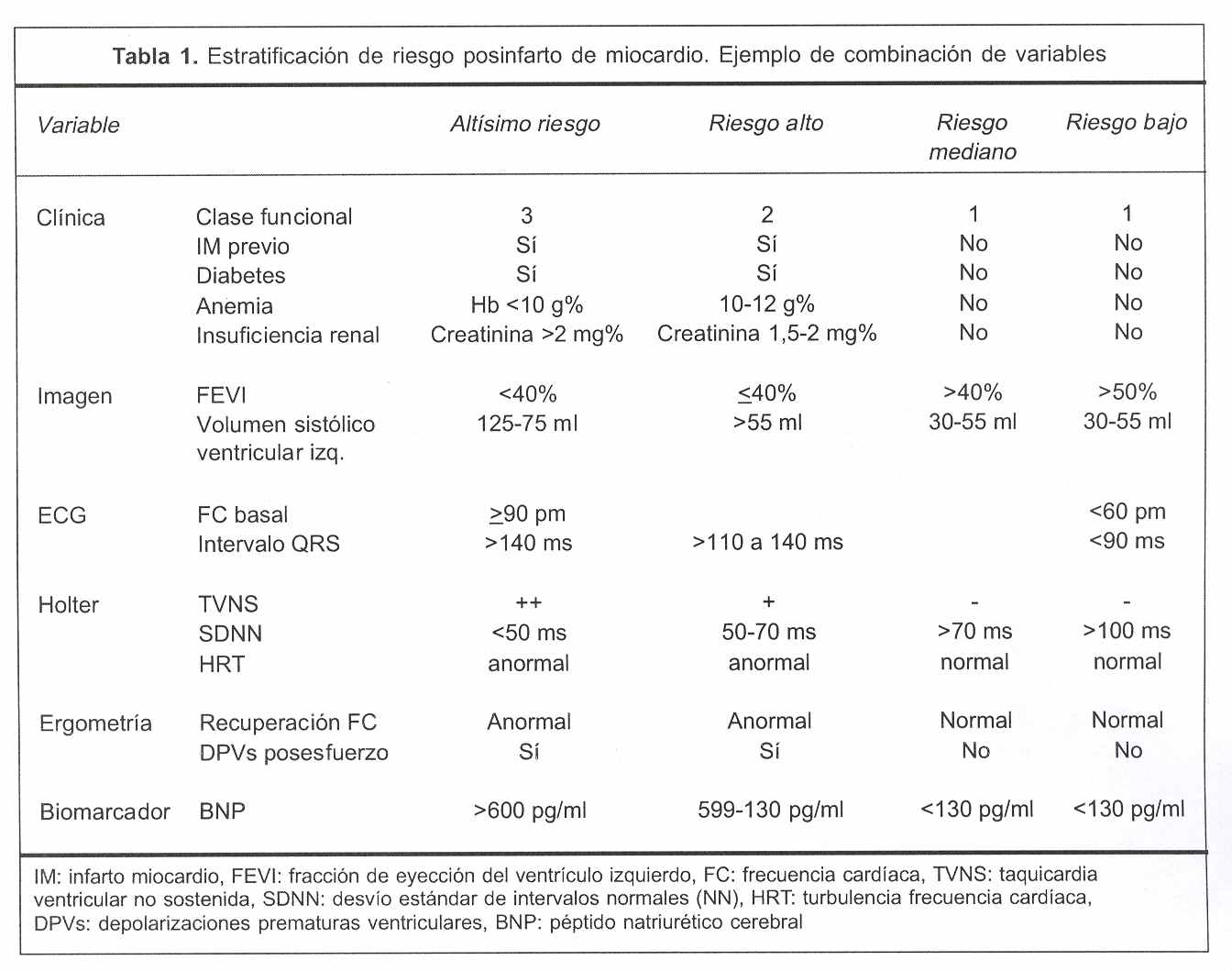
7) Combinación de variables (tabla 1)
No sabemos cuál es la combinación de factores de riesgo que tiene la capacidad predictiva más poderosa. Pero combinar variables es lógico y ha sido sugerido por varios autores(12). En la mayoría de los estudios, la simple adición de la FEVI incrementa enormemente la exactitud predictiva positiva. En el estudio ATRAMI, una combinación de sensibilidad barorrefleja disminuida, taquicardia ventricular no sostenida, y disminución de la función ventricular, implicó un incremento de 22 veces de muerte súbita(5,84). En el mismo estudio, la combinación de variabilidad de frecuencia cardíaca y sensibilidad barorrefleja bajas tenían un VPP de 15% para predecir muerte súbita en un año de seguimiento, y si se agregaba al modelo la disminución de la función ventricular, el VPP se incrementaba(25,84). Los estudios MADIT 1, MADIT 2, y MUSTT utilizaron la combinación de varios parámetros, fracción de eyección disminuida, y la presencia de taquicardia ventricular no sostenida(38,39,155,156).
]]> La proporción de pacientes con parámetros de riesgo múltiple positivo es baja. La mayoría de los eventos adversos ocurren en poblaciones de bajo riesgo, que no tienen todos estos parámetros alterados. Desafortunadamente, no disponemos de una combinación de factores que alcance un VPP mayor de 40%, con niveles razonables de sensibilidad. Una combinación efectiva debería incluir marcadores de daño cardíaco, de balance autonómico y neurohumorales (tabla 1). En el otro extremo, si todos los marcadores de riesgo están en el rango de normalidad, el paciente tiene un pronóstico favorable. En el estudio ATRAMI la mortalidad fue sólo de 1% si el SDNN o la sensibilidad barrorefleja estaban preservadas(5).¿Cómo disminuir la mortalidad luego del IM?
Tratamiento farmacológico y otras medidas
Los betabloqueantes han logrado reducir el número de eventos arrítmicos. En más de 50 estudios randomizados que incluyeron 55.000 pacientes, los betabloqueantes demostraron reducir la mortalidad total, y sobre todo la muerte súbita. Su efecto sobre la muerte súbita en alguno de estos estudios es una reducción de 30%-50%(157). Los betabloqueantes con mayor efecto son los betaselectivos y con perfil lipofílico(157).
El tratamiento también debe controlar los factores de riesgo asociados con la progresión de la enfermedad coronaria. Como el efecto de estos factores de riesgo es aditivo, se debe asegurar que el paciente reciba un tratamiento farmacológico efectivo, y terapias no farmacológicas que incluyan el control de la hiperglicemia, cese de tabaquismo, modificación de hábitos, reducción de peso, programas de ejercicio y rehabilitación cardíaca. El tratamiento de otros factores de riesgo es importante para prevenir la muerte prematura. La modificación de los factores de riesgo puede evitar la progresión de la enfermedad coronaria o enlentecerla. En referencia a la hipertensión, un metaanálisis ha demostrado que el tratamiento antihipertensivo en pacientes con hipertensión diastólica redujo 14% la muerte coronaria, y el IM no fatal(158). En el otro extremo, el tratamiento antihipertensivo de los pacientes añosos con hipertensión sistólica aislada reduce la mortalidad 17%, y la incidencia de IM, 31%(159,160).
En consecuencia, el tratamiento debe incluir:
1) Terapia antitrombótica.
2) Betabloqueantes.
3) Inhibidores de la enzima convertidora.
4) Fármacos que optimicen el perfil lipídico, elevando el HDL y disminuyendo el LDL.
]]> 5) Otros fármacos: el estudio RALES demostró que la adición de espironolactona en pacientes con disminución severa de la función ventricular logró una baja significativa de la mortalidad cardíaca y de la falla cardíaca. Sin embargo, la investigación no estudió solamente pacientes posinfarto de miocardio(161,162).6) Algunos datos sugieren que la suplementación con ácidos grasos poliinsaturados (n-3 PUFA), puede reducir la mortalidad por todas las causas luego de un IM y también la muerte súbita(163). En el estudio GISSI, los pacientes que recibieron tratamiento con n-3 PUFA, 1 g/día, mostraron una rápida divergencia en las curvas de sobrevida, luego de la randomización la mortalidad total disminuyó luego de tres meses de tratamiento (riesgo relativo 0,59, IC95% 0,36-0,97). A los cuatro meses fue aun superior (riesgo relativo 0,47, IC95% 0,21-0,99). Otros estudios han confirmado los efectos antiarrítmicos de estas sustancias(164).
]]> Tratamiento no farmacológico: el desfibrilador implantable
1) Prevención primaria
En los estudios MADIT se analizaron pacientes con IM previo, taquicardia ventricular no sostenida y fracción de eyección menor de 30%-35%. La mortalidad disminuyó 54% con el uso de un desfibrilador implantable(105). El estudio MUSTT incluyó 2.139 pacientes con enfermedad coronaria o IM previo, FEVI menor de 40%, sin síntomas y taquicardia ventricular no sostenida. La terapia con desfibrilador disminuyó significativamente el riesgo de muerte arrítmica o de paro cardíaco durante un seguimiento de cinco años, comparado con el grupo de pacientes control, sin antiarrítmicos o terapia antiarrítmica guiada por el estudio electrofisiológico(155). En el estudio CABG-PATCH, los pacientes fueron referidos para realizar revascularización miocárdica, aquellos con FEVI menor de 35%, y electrocardiograma de promediación de señales anormal, se randomizaron a recibir desfibrilador o tratamiento convencional. No se observó mejor pronóstico si el paciente recibía un desfibrilador(172,173).
El estudio MADIT-II mostró un beneficio para todos los pacientes posinfarto de miocardio con una fracción de eyección menor de 30%, logrando reducir la mortalidad en 31% durante un seguimiento de 20 meses(36-38,60).
Debe tenerse en cuenta que en la falla cardíaca avanzada una bradiarritmia puede ser la causa de muerte súbita y estas muertes pueden ser prevenidas también por el desfibrilador.
El estudio COMPANION incluyó 1.520 pacientes en ritmo sinusal, con una clase funcional III-IV, con FEVI menor de 35%, volumen telediastólico del ventrículo izquierdo igual a 60 mm, un intervalo PR mayor de 150 ms y un intervalo QRS mayor de 120 ms. Los pacientes se randomizaron en tres brazos: tratamiento farmacológico óptimo, terapia de resincronización cardíaca, o desfibrilador implantable con resincronización. Este último brazo presentó una reducción relativa de la mortalidad por todas las causas de 43%, en comparación con el brazo de tratamiento farmacológico(174,175).
Las recomendaciones de la ACC/AHA/NASPE-HRS del año 2002 (Sociedades Norteamericanas de Cardiología y Arritmias y de la Sociedad Europea de Cardiología) para implantar un desfibrilador en prevención primaria son(25,176):
Pacientes con fracción de eyección igual a 30%, al menos un mes después de IM o tres meses después de una revascularización quirúrgica, es una indicación clase 2A, con un nivel de evidencia B.
También se recomienda la terapia con desfibrilador para pacientes posinfarto de miocardio con disminución de la fracción de eyección (menor de 40%), taquicardia ventricular no sostenida clínica, o arritmias ventriculares sostenidas en el estudio electrofisiológico (recomendación clase 1 para el implante de desfibrilador, nivel de evidencia A), basada en los estudios MADIT y MUSTT(176,177).
2) Prevención secundaria
]]> En pacientes posinfarto de miocardio resucitados por muerte súbita cardíaca, sea por taquicardia ventricular polimórfica o fibrilación ventricular, la revascularización es insuficiente en prevenir arritmias malignas. La única terapia eficaz basada en evidencia es el implante de un desfibrilador. En pacientes inducibles en el preoperatorio es necesario realizar un estudio electrofisiológico posoperatorio ya que solamente 50% son suprimidos por la cirugía cardíaca. A pesar de un estudio negativo posoperatorio, el paciente puede seguir perteneciendo al grupo de alto riesgo de muerte súbita(178). En varios estudios de prevención primaria y secundaria (AVID, CASH, CIDS y SCD-Heft)(39,179-182), más de la mitad de los pacientes tenían IM previo y 80% historia de enfermedad coronaria. En consecuencia, este concepto se extiende para la mayoría de los pacientes posinfarto de miocardio con factores o perfiles de riesgo similares. El estudio AVID demostró una mortalidad menor en pacientes con desfibrilador en un seguimiento de tres años, comparado con un grupo control tratado con amiodarona. El subgrupo de pacientes con fracción de eyección normal no se benefició de la terapia con desfibrilador (181). En los estudios CASH y CIDS se observó una mayor sobrevida en aquellos pacientes que recibieron un desfibrilador. CASH y AVID incluyeron sujetos con fracción de eyección preservada además de pacientes con baja fracción de eyección(107,182). En un metaanálisis de ambos estudios, la terapia con desfibrilador se asoció significativamente a un mejor pronóstico (riesgo relativo de mortalidad 0,73, IC95% 0,59-0,89), durante un seguimiento de seis años(107).Las recomendaciones actuales para el implante de un desfibrilador establecen las siguientes indicaciones clase 1, en prevención secundaria(25,176):
- Paro cardíaco por taquicardia ventricular o fibrilación ventricular que no tuviera una causa transitoria y reversible (clase 1, nivel de evidencia A).
- Taquicardia ventricular sostenida espontánea asociada a cardiopatía estructural (clase 1, nivel de evidencia B).
- Taquicardia ventricular sostenida espontánea en personas sin cardiopatía estructural, que no sea pasible de otros tratamientos (clase 1, nivel de evidencia C).
En pacientes posinfarto de miocardio, con insuficiencia cardíaca y FEVI mayor de 35%, las arritmias ventriculares no sostenidas no deberían tratarse, salvo que sean sintomáticas.
En pacientes resucitados de muerte súbita por fibrilación ventricular, o que han sufrido taquicardia ventricular sostenida o síncope no explicado posinfarto de miocardio, el implante de un desfibrilador implantable es el tratamiento de elección. Si la clase funcional es mala a pesar de un tratamiento médico óptimo (y además presenta bradicardia sinusal, intervalos PR y QRS anormales), debe valorarse el uso de un desfibrilador implantable con capacidad de resincronización ventricular(175).
Conclusiones
- La mortalidad posinfarto de miocardio oscila entre 5% a 11%, dentro de los seis a 12 meses luego del alta y es de 20% a los cinco años.
- En la estratificación del riesgo de muerte súbita posinfarto de miocardio se utilizan parámetros clásicos: la historia clínica, la clase funcional de la NYHA y la FEVI. Los pacientes con función ventricular izquierda deprimida deben recibir beta-bloqueantes, inhibidores de la enzima convertidora, espironolactona y antitrombóticos.
]]> - Numerosas variables permiten identificar a los grupos de riesgo. Cuando se combinan, su poder predictivo es muy superior, pero estudios prospectivos con gran cantidad de pacientes deben ser llevados a cabo para establecer modelos sólidos de predicción.- Los pacientes con disminución de la función ventricular izquierda (menor de 40%), marcadores autonómicos y biomarcadores anormales, tienen un altísimo riesgo de muerte súbita a corto o mediano plazo.
En muchos casos nos enfrentamos a una opción relativamente simple: implantar o no un desfibrilador. La pregunta difícil es quién toma la decisión: la sociedad o un grupo de médicos expertos. Otra alternativa sería entrenar a familiares o vecinos del paciente a utilizar un desfibrilador automático externo (DAE). Las familias de pacientes en riesgo se podrían congregar en comunidades donde familiares o vecinos puedan procurar una desfibrilación rápida.
De ninguna manera debemos quedar de brazos cruzados ante la evidencia; en muchos casos podemos saber quién va a morir y, en consecuencia, podemos evitarlo.
Summary
Sudden death is responsible of more than half of cardiac related death. Prediction of patients at high risk of sudden death has improved but more than 90% of deaths coincide with unidentifying risk factors free-people. More over, we know that most of them present a previous coronary disease and also that cardiac sudden death is essentially an extrahospitalarian problem.
Myocardial arrest is a factor to easily detect groups with high mortality rates. Mortality rates after myocardial infarction range from 5 to 11%, within six to 12 months after release and 20% at five years. Although many markers have been identifying, their predictor value is relatively low. Specific markers were described and reviewed to stratify sudden death risks; left ventricular disfunction is one of the principal marker; others as follow: clinical, based on images, autonomics and electrocardiographics, besides biomarkers, invasive and combined methods.
Risk stratification is designed according to clinical history, functional class and left ventricular ejection fraction (LVEF/FEVI).
At first, patients at high risk should receive beta-blockers, enzyme converted inhibitors, spironolactone and antithrombotics. In many cases, cardiodefibrillator implantation should be considered.
Résumé
]]> La mort subite est responsable de plus de la moitié des décès à causes cardiaques. Notre habileté pour reconnaître les patients ayant un risque élevé de mort subite s'est accru, mais 90% des morts arrivent chez des gens n'ayant pas des facteurs de risque évidents. On sait d'ailleurs que la plupart ont une maladie coronaire préalable et que la mort subite cardiaque est avant tout un problème extra-hospitalier. Une population facile à détecter, à haute mortalité, est celle qui a déjà subi un infarctus du myocarde. La mortalité post-infarctus de myocarde varie entre 5 et 11%, 6 à 12 mois après l'exeat, et 20% après 5 ans. De nombreux marqueurs ont été identifiés, mais leur valeur prédictive positive reste moindre. La dysfonction ventriculaire gauche en est la plus importante. D'autres variables : cliniques, basées sur des images, autonomiques, électrocardiographiques et quelques bio-marqueurs, des méthodes envahissantes et la combinaison de variables, ont été décrites afin de stratifier le risque, et on en fait le commentaire ici.Malheureusement, on ignore encore quelle est la combinaison ayant la capacité prédictive la plus puissante. De nos jours, la stratification du risque de mort subite est faite ne tenant compte que de l'histoire clinique, la classe fonctionnelle et la fraction d'éjection ventriculaire gauche (FEVI). En principe, les patients à haut risque doivent recevoir des bêtabloquants, inhibiteurs de l'enzyme de conversion, spironolactone et anti-thrombotiques. Dans des cas particuliers, on devra envisager l'implantation d'un cardio-défibrillateur. D'autres variables seront incorporées afin de mieux identifier les groupes à grand risque.
Resumo
A morte súbida é responsável por mais de metade das mortes por causas cardíacas. Nossa capacidade de reconhecer os pacientes com alto risco de morte súbida aumentou porém 90% das mortes se dão em pacientes sem fatores de risco identificáveis. Sabemos também que a maioria tinha uma patologia coronaria pré-existente e que a morte súbida cardíaca é fundamentalmente um problema extra-hospitalar. Uma população com alta mortalidade e fácil de identificar é a que já sofreu um infarto de miocárdio. A mortalidade pós-infarto de miocardio varia entre 5% a 11% , 6 a 12 meses depois da alta e 20% depois de cinco anos. Muitos marcadores foram identificados porém seu valor preditivo positivo é relativamente baixo. O mais importante deles é a disfunção ventricular esquerda. Outras variáveis como as clínicas, as baseadas em imagens, as autonômicas, as eletrocardiográficas, além de alguns biomarcadores, métodos invasivos e combinação de variáveis foram descritas para estratificar o risco e são discutidas neste trabalho. Infelizmente, não identificamos a combinação com a melhor capacidade preditiva. Atualmente a estratificação do risco de morte súbida é feito usando somente a história clínica, a classe funcional e a fração de ejeção ventricular esquerda (FEVE). Básicamente os pacientes de alto risco devem receber betabloqueadores, inibidores da enzima conversora, espironolactona e antitrombóticos. Em algunos casos selecionados deve-se considerar a implantação de um cardiodesfibrilador. Outras variáveis serão incorporadas para melhorar a identificação dos grupos com maior risco.
Bibliografía
1. Callans DJ. Out-of-hospital cardiac arrest-the solution is shocking. N Engl J Med 2004; 351: 632-4.
2. Risk stratification and survival after myocardial infarction. N Engl J Med 1983; 309: 331-6.
]]>3. Kleiger RE, Miller JP, Bigger JT Jr, Moss AJ. Decreased heart rate variability and its association with increased mortality after acute myocardial infarction. Am J Cardiol 1987; 59: 256-62.
4. La Rovere MT, Mortara A. Assessment of the autonomic nervous system after infarction and its prognostic significance. Cardiologia 1994; 39: 225-31.
5. La Rovere MT, Bigger JT Jr, Marcus FI, Mortara A, Schwartz PJ. Baroreflex sensitivity and heart-rate variability in prediction of total cardiac mortality after myocardial infarction. ATRAMI (Autonomic Tone and Reflexes After Myocardial Infarction) Investigators. Lancet 1998; 351: 478-84.
6. La Rovere MT. Baroreflex sensitivity as a new marker for risk stratification. Z Kardiol 2000; 89 Suppl 3: 44-50.
7. Maggioni AP, Zuanetti G, Franzosi MG, Rovelli F, Santoro E, Staszewsky L, et al. Prevalence and prognostic significance of ventricular arrhythmias after acute myocardial infarction in the fibrinolytic era. GISSI-2 results. Circulation 1993; 87: 312-22.
]]>8. Ohno J, Watanabe E, Toyama J, Kawamura T, Ohno M, Kodama I. Risk stratification and survival in post myocardial infarction patients: a large prospective and multicenter study in Japan. Int J Cardiol 2004; 93: 263-8.
9. Myerburg RJ, Kessler KM, Castellanos A. Pathophysiology of sudden cardiac death. Pacing Clin Electrophysiol 1991; 14: 935-43.
10. Myerburg RJ, Kessler KM, Castellanos A. Sudden cardiac death. Structure, function, and time-dependence of risk. Circulation 1992; 85(1 Suppl): I2-10.
11. Priori SG, Aliot E, Blomstrom-Lundqvist C, Bossaert L, Breithardt G, Brugada P, et al. Task Force on Sudden Cardiac Death of the European Society of Cardiology. Eur Heart J 2001; 22: 1374-450.
12. Priori SG, Aliot E, Blomstrom-Lundqvist C, Bossaert L, Breithardt G, Brugada P, et al. Task Force on Sudden Cardiac Death, European Society of Cardiology. Summary of recommendations. Ital Heart J Suppl 2002; 3: 1051-65.
]]>13. Olshausen KV, Witt T, Pop T, Treese N, Bethge KP, Meyer J. Sudden cardiac death while wearing a Holter monitor. Am J Cardiol 1991; 67: 381-6.
14. Zipes DP, Wellens HJ. Sudden cardiac death. Circulation 1998; 98: 2334-51.
15. Di Maio VJ, Di Maio DJ. Incidence of coronary thrombosis in sudden death due to coronary artery disease. Am J Forensic Med Pathol 1993; 14: 273-5.
16. Farb A, Tang AL, Burke AP, Sessums L, Liang Y, Virmani R. Sudden coronary death: Frequency of active coronary lesions, inactive coronary lesions, and myocardial infarction. Circulation 1995; 92: 1701-9.
17. Uretsky BF, Thygesen K, Armstrong PW, Cleland JG, Horowitz JD, Massie BM, et al. Acute coronary findings at autopsy in heart failure patients with sudden death: results from the assessment of treatment with lisinopril and survival (ATLAS) trial. Circulation 2000; 102: 611-6.
]]>18. Marcus FI, Cobb LA, Edwards JE, Kuller L, Moss AJ, Bigger JT Jr, et al. Mechanism of death and prevalence of myocardial ischemic symptoms in the terminal event after acute myocardial infarction. Am J Cardiol 1988; 61: 8-15.
19. Gorgels AP, Gijsbers C, Vreede-Swagemakers J, Lousberg A, Wellens HJ. Out-of-hospital cardiac arrest-the relevance of heart failure: The Maastricht Circulatory Arrest Registry. Eur Heart J 2003; 24: 1204-9.
20. Berger CJ, Murabito JM, Evans JC, Anderson KM, Levy D. Prognosis after first myocardial infarction: Comparison of Q-wave and non-Q-wave myocardial infarction in the Framingham Heart Study. JAMA 1992; 268: 1545-51.
21. Kaul P, Armstrong P, Chang W, Naylor D, Granger GB, Lee KL, et al. Long-Term Mortality of Patients with Acute Myocardial Infarction in the United States and Canada: Comparison of Patients Enrolled in Global Utilization of Streptokinase and t-PA for Occluded Coronary Arteries (GUSTO)-I. Circulation 2004; 110: 1754-60.
22. Aros F, Loma-Osorio A, Bosch X, González AJ, López BL, Marrugat J, et al. Management of myocardial infarction in Spain (1995-99): Data from the registry of the Ischaemic Heart Disease Working Group (RISCI) of the Spanish Society of Cardiology. Rev Esp Cardiol 2001; 54: 1033-40.
]]>23. Aros F, Cunat J, Loma-Osorio A, Torrado E, Bosch X, Rodriguez JJ, et al. Management of myocardial infarction in Spain in the year 2000: The PRIAMHO II study. Rev Esp Cardiol 2003; 56: 1165-73.
24. Williams RI, Fraser AG, West RR. Gender differences in management after acute myocardial infarction: not 'sexism' but a reflection of age at presentation. J Public Health (Oxf) 2004; 26: 259-63.
25. Priori SG, Aliot E, Blomstrom-Lundqvist C, Bossaert L, Breithardt G, Brugada P, et al. Task Force on Sudden Cardiac Death, European Society of Cardiology. Europace 2002; 4: 3-18.
26. Alexander KP, Peterson ED. Evidence-based care for all patients. Am J Med 2003; 114: 333-5.
27. Alexander KP, Galanos AN, Jollis JG, Stafford JA, Peterson ED. Post-myocardial infarction risk stratification in elderly patients. Am Heart J 2001; 142: 37-42.
]]>28. Cairns JA, Connolly SJ, Roberts R, Gent M. Randomised trial of outcome after myocardial infarction in patients with frequent or repetitive ventricular premature depolarisations: CAMIAT. Canadian Amiodarone Myocardial Infarction Arrhythmia Trial Investigators. Lancet 1997; 349: 675-82.
29. Julian DG, Camm AJ, Frangin G, Janse MJ, Munoz A, Schwartz PJ, et al. Randomised trial of effect of amiodarone on mortality in patients with left-ventricular dysfunction after recent myocardial infarction: EMIAT. European Myocardial Infarct Amiodarone Trial Investigators. Lancet 1997; 349: 667-74.
30. Hohnloser SH, Klingenheben T, Zabel M, Schopperl M, Mauss O. Prevalence, characteristics and prognostic value during long-term follow-up of nonsustained ventricular tachycardia after myocardial infarction in the thrombolytic era. J Am Coll Cardiol 1999; 33: 1895-902.
31. Camm AJ, Pratt CM, Schwartz PJ, Al Khalidi HR, Spyt MJ, Holroyde MJ, et al. Mortality in patients after a recent myocardial infarction: a randomized, placebo-controlled trial of azimilide using heart rate variability for risk stratification. Circulation 2004; 109: 990-6.
32. Camm AJ, Karam R, Pratt CM. The azimilide post-infarct survival evaluation (ALIVE) trial. Am J Cardiol 1998; 81: 35D-39D.
]]>33. Myerburg RJ, Kessler KM, Mallon SM, Cox MM, deMarchena E, Interian A Jr, et al. Life-threatening ventricular arrhythmias in patients with silent myocardial ischemia due to coronary-artery spasm. N Engl J Med 1992; 326: 1451-5.
34. Myerburg RJ, Kessler KM, Castellanos A. Sudden cardiac death: epidemiology, transient risk, and intervention assessment. Ann Intern Med 1993; 119: 1187-97.
35. Borer JS, Miller D, Schreiber T, Charash B, Gerling B. Radionuclide cineangiography in acute myocardial infarction: role in prognostication. Semin Nucl Med 1987; 17: 89-94.
36. Moss AJ, Daubert J, Zareba W. MADIT-II: clinical implications. Card Electrophysiol Rev 2002; 6: 463-5.
37. Moss AJ. MADIT-II and implications for noninvasive electrophysiologic testing. Ann Noninvasive Electrocardiol 2002; 7: 179-80.
]]>38. Moss AJ. MADIT-II and its implications. Eur Heart J 2003; 24: 16-8.
39. Klein H, Auricchio A, Reek S, Geller C. New primary prevention trials of sudden cardiac death in patients with left ventricular dysfunction: SCD-HEFT and MADIT-II. Am J Cardiol 1999; 83: 91D-97D.
40. Hohnloser SH, Connolly SJ, Kuck KH, Dorian P, Fain E, Hampton JR, et al. The defibrillator in acute myocardial infarction trial (DINAMIT): study protocol. Am Heart J 2000; 140: 735-9.
41. Comisión Honoraria para la Salud Cardiovascular. Informe: mortalidad por enfermedades cardiovasculares en el Uruguay (1994 a 2003) Área de Epidemiología. Agosto 2004, páginas 1-8. Obtenido de: www.cardiosalud.org. (Consulta enero/2006)
42. Bayes de Luna A, Coumel P, Leclercq JF. Ambulatory sudden cardiac death: mechanisms of production of fatal arrhythmia on the basis of data from 157 cases. Am Heart J 1989; 117: 151-9.
43. Franz MR. Mechano-electrical feedback in ventricular myocardium. Cardiovasc Res 1996; 32: 15-24.
44. Brugada P, Andries EW, Mont L, Gursoy S, Willems H, Kaissar S. Mechanisms of sudden cardiac death. Drugs 1991; 41 Suppl 2: 16-23.
45. Peterson ED, Shaw LJ, Califf RM. Risk stratification after myocardial infarction. Ann Intern Med 1997; 126: 561-82.
46. Zureik M, Touboul PJ, Bonithon-Kopp C, Courbon D, Ruelland I, Ducimetiere P. Differential association of common carotid intima-media thickness and carotid atherosclerotic plaques with parental history of premature death from coronary heart disease: the EVA study. Arterioscler Thromb Vasc Biol 1999;19: 366-71.
47. Bollani G, Ferrari R, Bersatti F, Ferrari M, Cattaneo M, Zighetti ML, et al. A hyperhomocysteinemia study in a population with a familial factor for acute myocardial infarct and sudden cardiac death at a young age. Cardiologia 1999; 44: 75-81.
48. Friedlander Y, Siscovick DS, Arbogast P, Psaty BM, Weinmann S, Lemaitre RN, et al. Sudden death and myocardial infarction in first degree relatives as predictors of primary cardiac arrest. Atherosclerosis 2002; 162: 211-6.
49. Go A, Chertow G, Fan D, McCulloch C, Hsu C. Chronic kidney disease and the risk of death, cardiovascular events and hospitalization. N Engl J Med 2004; 351: 1296-05.
50. Anand I, McMurray J, Whitmore J, Warren M, Phan A, McCamish MA, et al. Anemia and its relationship to clinical outcome in heart failure. Circulation 2004; 110: 149-54.
51. Bigger JT Jr. Identification of patients at high risk for sudden cardiac death. Am J Cardiol 1984; 54: 3D-8D.
52. Villacastin J, Bover R, Castellano NP, Moreno J, Morales R, García-Espinosa A. Risk stratification and prevention of sudden death in patients with heart failure. Rev Esp Cardiol 2004; 57: 768-82.
53. Kober L, Torp-Pedersen C, Ottesen M, Burchardt H, Korup E, Lyngborg K. Influence of age on the prognostic importance of left ventricular dysfunction and congestive heart failure on long-term survival after acute myocardial infarction: TRACE Study Group. Am J Cardiol 1996; 78: 158-62.
54. Lamas GA, Pfeffer MA, Hamm P, Wertheimer J, Rouleau JL, Braunwald E. Do the results of randomized clinical trials of cardiovascular drugs influence medical practice?: The SAVE Investigators. N Engl J Med 1992; 327: 241-7.
55. Lamas GA, Flaker GC, Mitchell G, Smith SC Jr, Gersh BJ, Wun CC, et al. Effect of infarct artery patency on prognosis after acute myocardial infarction: The Survival and Ventricular Enlargement Investigators. Circulation 1995; 92: 1101-9.
56. Connors KF, Lamas GA. Postmyocardial infarction patients: experience from the SAVE trial. Am J Crit Care 1995; 4: 23-8.
57. Gosselink AT, Liem AL, Reiffers S, Zijlstra F. Prognostic value of predischarge radionuclide ventriculography at rest and exercise after acute myocardial infarction treated with thrombolytic therapy or primary coronary angioplasty: The Zwolle Myocardial Infarction Study Group. Clin Cardiol 1998; 21: 254-60.
58. Nicod P, Gilpin E, Dittrich H, Chappuis F, Ahnve S, Engler R, et al. Influence on prognosis and morbidity of left ventricular ejection fraction with and without signs of left ventricular failure after acute myocardial infarction. Am J Cardiol 1988; 61: 1165-71.
59. Moss AJ. MADIT-I and MADIT-II. J Cardiovasc Electrophysiol 2003; 14: S96-S98.
60. Moss AJ. MADIT-II: substudies and their implications. Card Electrophysiol Rev 2003; 7: 430-3.
61. Ong L, Green S, Reiser P, Morrison J. Early prediction of mortality in patients with acute myocardial infarction: a prospective study of clinical and radionuclide risk factors. Am J Cardiol 1986; 57: 33-8.
62. Madsen JK, Eliasen B. Left ventricular function and prognosis in patients suspected of acute myocardial infarction but without confirmed diagnosis: The risk of cardiac events related to echocardiography, systolic time intervals, and chest x-ray. Dan Med Bull 1988; 35: 182-5.
63. Norris RM, White HD, Cross DB, Wild CJ, Whitlock RM. Prognosis after recovery from myocardial infarction: the relative importance of cardiac dilatation and coronary stenoses. Eur Heart J 1992; 13: 1611-8.
64. Moller JE, Sondergaard E, Poulsen SH, Egstrup K. The Doppler echocardiographic myocardial performance index predicts left-ventricular dilation and cardiac death after myocardial infarction. Cardiology 2001; 95: 105-11.
65. White HD, Norris RM, Brown MA, Brandt PW, Whitlock RM, Wild CJ. Left ventricular end-systolic volume as the major determinant of survival after recovery from myocardial infarction. Circulation 1987; 76: 44-51.
66. O'Rourke RA, Brundage B, Froelicher V, Greenland P, Gruñid S, Hachamovitch R, et al. The American College of Cardiology/American Heart Association expert consensus document on electron beam computed tomography for the diagnosis and prognosis of coronary artery disease. J Am Coll Cardiol 2000; 36: 326-40.
67. Keelan PC, Bielak LF, Ashai K, Jamjoumv L, Denktas A, Rumberger J, et al. Long-term prognostic value of coronary calcification detected by electron beam computed tomography in patients undergoing coronary angiography. Circulation 2001; 104: 412-7.
68. Detrano R, Hsiai T, Wang S, Puentes G, Fallavollita J, Shields P, et al. Prognostic value of coronary calcification and angiographic stenoses in patients undergoing coronary angiography. J Am Coll Cardiol 1996; 27: 285-90.
69. Raggi P, Callister TQ, Cooil B, He ZX, Lippolis NJ, Russo DJ, et al. Identification of patients at increased risk of first unheralded acute myocardial infarction by electron beam computed tomography. Circulation 2000; 101: 850-5.
70. Detrano RC, Wong ND, Doherty TM, Shavelle R. Prognostic significance of coronary calcific deposits in asymptomatic high-risk subjects. Am J Med 1997; 102: 344-9.
71. O'Malley PG, Taylor AJ, Jaccson JL, Doherty TM, Detrano RC, et al. Prognostic value of coronary electron beam computed tomography for coronary heart disease events in asymptomatic populations. Am J Cardiol 2000; 85: 945-8.
72. Detrano RC, Wong ND, Doherty TM, Shavelle RM, Tang W, Ginzton LE, et al. Determining coronary event risk in asymptomatic high risk subjects: a risk factor vs. an anatomic approach. Circulation 1999; 99: 2633-8.
73. Arad Y, Spadaro LA, Goodman K, Lledo-Pérez A, Sherman S, Lerner G, et al. Predictive value of electron beam computed tomography of the coronary arteries: 19 month follow-up of 1,173 asymptomatic subjects. Circulation 1996; 93: 1951-3.
74. Seci A, Wong N, Tang W, Wang S, Doherty T, Detrano R. Electron beam computed tomographic coronary calcium as a predictor of coronary events: a comparison of two protocols. Circulation 1997; 96: 1122-9.
75. Raggi P, Cooil B, Callister TQ. Use of electron beam tomography data to develop models for prediction of hard coronary events. Am Heart J 2001; 141: 375-82.
76. Wayhs R, Zellinger A, Raggi P. High coronary artery calcium scores pose an extremely elevated risk for hard events. J Am Coll Cardiol 2002; 39: 225-30
77. Shaper AG, Wannamethee G, Macfarlane PW, Walker M. Heart rate, ischaemic heart disease, and sudden cardiac death in middle-aged British men. Br Heart J 1993; 70: 49-55.
78. Zuanetti G, Mantini L, Hernández-Bernal F, Barlera S, Di Gregorio D, Latini R, et al. Relevance of heart rate as a prognostic factor in patients with acute myocardial infarction: insights from the GISSI-2 study. Eur Heart J 1998; 19: F19-F26.
]]>79. Dekker JM, Schouten EG, Klootwijk P, Pool J, Swenne CA, Kromhout D. Heart rate variability from short electrocardiographic recordings predicts mortality from all causes in middle-aged and elderly men. The Zutphen Study. Am J Epidemiol 1997; 145: 899-908.
80. Zuanetti G, Neilson JM, Latini R, Santoro E, Maggioni AP, Ewing DJ. Prognostic significance of heart rate variability in post-myocardial infarction patients in the fibrinolytic era: The GISSI-2 results. Gruppo Italiano per lo Studio della Sopravvivenza nell' Infarto Miocardico. Circulation 1996; 94: 432-6.
81. Singh N, Mironov D, Armstrong PW, Ross AM, Langer A. Heart rate variability assessment early after acute myocardial infarction. Pathophysiological and prognostic correlates. GUSTO ECG Substudy Investigators. Global Utilization of Streptokinase and TPA for Occluded Arteries. Circulation 1996; 93: 1388-95.
82. Minamihaba O, Yamaki M, Tomoike H, Kubota I. Severity in myocardial dysfunction contributed to long-term fluctuation of heart rate, rather than short-term fluctuations. Ann Noninvasive Electrocardiol 2003; 8: 132-8.
83. Ziegler D, Piolot R, Strassburger K, Lambeck H, Dannehl K. Normal ranges and reproducibility of statistical, geometric, frequency domain, and non-linear measures of 24-hour heart rate variability. Horm Metab Res 1999; 31: 672-9.
]]>84. La Rovere MT, Pinna GD, Hohnloser SH, Marcus FI, Mortara A, Nohara R, et al. Baroreflex sensitivity and heart rate variability in the identification of patients at risk for life-threatening arrhythmias: implications for clinical trials. Circulation 2001; 103: 2072-7.
85. Berkowitsch A, Zareba W, Neumann T, Erdogan A, Nitt SM, Moss AJ, et al. Risk stratification using heart rate turbulence and ventricular arrhythmia in MADIT II: usefulness and limitations of a 10-minute holter recording. Ann Noninvasive Electrocardiol 2004; 9: 270-9.
86. Wessel N, Malberg H, Walther T. Heart rate turbulence: higher predictive value than other risk stratifiers?. Circulation 2004; 109: e150-e151.
87. Bauer A, Schmidt G. Heart rate turbulence. J Electrocardiol 2003; 36 Suppl: 89-93.
88. Schwab JO, Shlevkov N, Grunwald K, Schrickel JW, Yang A, Lickfett L, et al. Influence of the point of origin on heart rate turbulence after stimulated ventricular and atrial premature beats. Basic Res Cardiol 2004; 99: 56-60.
]]>89. Melenovsky V, Wichterle D, Simek J, Malik J. Heart rate turbulence-a new ECG predictor for risk of sudden death. Vnitr Lek 2002; 48: 150-4.
90. Sade E, Aytemir K, Oto A, Nazli N, Ozmen F, Ozkutlu H, et al. Assessment of heart rate turbulence in the acute phase of myocardial infarction for long-term prognosis. Pacing Clin Electrophysiol 2003; 26: 544-50.
91. Schmidt G, Malik M, Barthel P, Schneider R, Ulm K, Rolnitzky L, et al. Heart-rate turbulence after ventricular premature beats as a predictor of mortality after acute myocardial infarction. Lancet 1999; 353: 1390-6.
92. Barthel P, Schneider R, Bauer A, Ulm K, Schmitt C, Schomig A, et al. Risk stratification after acute myocardial infarction by heart rate turbulence. Circulation 2003; 108: 1221-6.
93. Jeron A, Kaiser T, Hengstenberg C, Lowel H, Riegger GA, Holmer S. Association of the heart rate turbulence with classic risk stratification parameters in postmyocardial infarction patients. Ann Noninvasive Electrocardiol 2003; 8: 296-301.
]]>94. Wichterle D, Simek J, La Rovere MT, Schwartz PJ, Camm AJ, Malik M. Prevalent low-frequency oscillation of heart rate: novel predictor of mortality after myocardial infarction. Circulation 2004; 110: 1183-90.
95. Makikallio TH, Hoiber S, Kober L, Torp-Pedersen C, Peng CK, Goldberger AL, et al. Fractal analysis of heart rate dynamics as a predictor of mortality in patients with depressed left ventricular function after acute myocardial infarction: TRACE Investigators. TRAndolapril Cardiac Evaluation. Am J Cardiol 1999; 83: 836-9.
96. Makikallio TH, Huikuri HV, Makikallio A, Sourander LB, Mitrani RD, Castellanos A, et al. Prediction of sudden cardiac death by fractal analysis of heart rate variability in elderly subjects. J Am Coll Cardiol 2001; 37: 1395-402.
97. Huikuri HV, Makikallio TH, Peng CK, Goldberger AL, Hintze U, Moller M. Fractal correlation properties of R-R interval dynamics and mortality in patients with depressed left ventricular function after an acute myocardial infarction. Circulation 2000; 101: 47-53.
98. Pincus SM, Goldberger AL. Physiological time-series analysis: what does regularity quantify?. Am J Physiol 1994; 266: H1643-H1656.
]]>99. Moss AJ, Vyas A, Greenberg H, Case RB, Zareba W, Hall WJ, et al. Temporal aspects of improved survival with the implanted defibrillator (MADIT-II). Am J Cardiol 2004; 94: 312-5.
100. Dhingra RC, Deedwania PC. Significance of fascicular block complicating acute myocardial infarction. Indian Heart J Teach Ser 1980; 159-66.
101. Lie KI, Durrer D. Common arrhythmias in acute myocardial infarction. Cardiovasc Clin 1980; 11: 191-201.
102. Perkiomaki JS, Zareba W, Greenberg HM, Moss AJ. Usefulness of standard electrocardiographic parameters for predicting cardiac events after acute myocardial infarction during modern treatment era. Am J Cardiol 2002; 90: 205-9.
103. Dekker JM, Schouten EG, Klootwijk P, Pool J, Kromhout D. ST segment and T wave characteristics as indicators of coronary heart disease risk: the Zutphen study. J Am Coll Cardiol 1995; 25: 1321-6
104. Statters DJ, Malik M, Redwood S, Hnatkova K, Staunton A, Camm AJ. Use of ventricular premature complexes for risk stratification after acute myocardial infarction in the thrombolytic era. Am J Cardiol 1996; 77: 133-8.
105. Moss AJ. Background, outcome, and clinical implications of the Multicenter Automatic Defibrillator Implantation Trial (MADIT). Am J Cardiol. 1997; 80: 28F-32F.
106. Connolly SJ, Gent M, Roberts RS, Dorian P, Roy D, Sheldon RS, et al. Canadian implantable defibrillator study (CIDS): a randomized trial of the implantable cardioverter defibrillator against amiodarone. Circulation 2000; 101: 1297-302.
107. Connolly SJ, Hallstrom AP, Cappato R, Schron EB, Kuck KH, Zipes DP, et al. Meta-analysis of the implantable cardioverter defibrillator secondary prevention trials. AVID, CASH and CIDS studies. Antiarrhythmics vs Implantable Defibrillator study. Cardiac Arrest Study Hamburg . Canadian Implantable Defibrillator Study. Eur Heart J 2000; 21: 2071-8.
108. The AVID Investigators. Antiarrhythmics Versus Implantable Defibrillators (AVID)-rationale, design, and methods. Am J Cardiol 1995; 75: 470-5.
109. The AVID Investigators. Causes of death in the Antiarrhythmics Versus Implantable Defibrillators (AVID) Trial. J Am Coll Cardiol 1999; 34: 1552-9.
110. Steinberg JS, Martins J, Sadanandan S, Goldner B, Menchavez E, Domanski M, et al. Antiarrhythmic drug use in the implantable defibrillator arm of the Antiarrhythmics Versus Implantable Defibrillators (AVID) Study. Am Heart J 2001; 142: 520-9.
111. Klein RC, Raitt MH, Wilkoff BL, Beckman KJ, Coromilas J, Wyse DG, et al. Analysis of implantable cardioverter defibrillator therapy in the Antiarrhythmics Versus Implantable Defibrillators (AVID) Trial. J Cardiovasc Electrophysiol 2003; 14: 940-8.
112. Elhendy A, Chandrasekaran K, Gersh BJ, Mahoney D, Burger KN, Pellikka PA. Functional and prognostic significance of exercise-induced ventricular arrhythmias in patients with suspected coronary artery disease. Am J Cardiol 2002; 90: 95-100.
113. Frolkis JP, Pothier CE, Blackstone EH, Lauer MS. Frequent ventricular ectopy after exercise as a predictor of death. N Engl J Med 2003; 348: 781-90.
114. O'Neill JO, Young JB, Pothier CE, Lauer MS. Severe frequent ventricular ectopy after exercise as a predictor of death in patients with heart failure. J Am Coll Cardiol 2004; 44: 820-6.
115. Dresing TJ, Blackstone EH, Pashkow FJ, Snader CE, Marwick TH, Lauer MS. Usefulness of impaired chronotropic response to exercise as a predictor of mortality, independent of the severity of coronary artery disease. Am J Cardiol 2000; 86: 602-9.
116. Lauer MS, Francis GS, Okin PM, Pashkow FJ, Snader CE, Marwick TH. Impaired chronotropic response to exercise stress testing as a predictor of mortality. JAMA 1999; 281: 524-9.
117. Lauer MS. Chronotropic incompetence: ready for prime time. J Am Coll Cardiol 2004; 44: 431-2.
118. Arnold AE, Simoons ML, Detry JM, von Essen R, Van de WF, Deckers JW, et al. Prediction of mortality following hospital discharge after thrombolysis for acute myocardial infarction: is there a need for coronary angiography? European Cooperative Study Group. Eur Heart J 1993; 14: 306-15.
119. Shaw LJ, Peterson ED, Kesler K, Hasselblad V, Califf RM. A metaanalysis of predischarge risk stratification after acute myocardial infarction with stress electrocardiographic, myocardial perfusion, and ventricular function imaging. Am J Cardiol 1996; 78: 1327-37.
120. Villella M, Villella A, Barlera S, Franzosi MG, Maggioni AP. Prognostic significance of double product and inadequate double product response to maximal symptom-limited exercise stress testing after myocardial infarction in 6296 patients treated with thrombolytic agents: GISSI-2 Investigators Grupo Italiano per lo Studio della Sopravvivenza nell-Infarto Miocardico. Am Heart J 1999; 137: 443-52.
121. Cole CR, Blackstone EH, Pashkow FJ, Snader CE, Lauer MS. Heart-rate recovery immediately after exercise as a predictor of mortality. N Engl J Med 1999; 341: 1351-7.
122. Lauer MS. Exercise electrocardiogram testing and prognosis: Novel markers and predictive instruments. Cardiol Clin 2001; 19: 401-14.
123. Breithardt G, Cain ME, el-Sherif N, Flowers N, Hombach V, Janse M, et al. Standards for analysis of ventricular late potentials using high resolution or signal-averaged electrocardiography: A statement by a Task Force Committee between the European Society of Cardiology, the American Heart Association and the American College of Cardiology. Eur Heart J 1991; 12: 473-80.
124. Breithardt G, Borggrefe M, Fetsch T, Budde T. New approaches to risk stratification after myocardial infarction. J Cardiovasc Pharmacol 1991; 17 (Suppl 6): S82-S86.
125. Vaitkus PT, Kindwall KE, Marchlinski FE, Miller JM, Buxton AE, Josephson ME. Differences in electrophysiological substrate in patients with coronary artery disease and cardiac arrest or ventricular tachycardia: Insights from endocardial mapping and signal-averaged electrocardiography. Circulation 1991; 84: 672-8.
126. Simson MB. Use of signals in the terminal QRS complex to identify patients with ventricular tachycardia after myocardial infarction. Circulation 1981; 64: 235-42.
127. Steinberg JS, Regan A, Sciacca RR, Bigger JT Jr, Fleiss JL. Predicting arrhythmic events after acute myocardial infarction using the signal-averaged electrocardiogram. Am J Cardiol 1992; 69: 13-21.
128. McClements BM, Adgey AA. Value of signal-averaged electrocardiography, radionuclide ventriculography, Holter monitoring and clinical variables for prediction of arrhythmic events in survivors of acute myocardial infarction in the thrombolytic era. J Am Coll Cardiol 1993; 21: 1419-27.
129. El-Sherif N, Denes P, Katz R, Capone R, Mitchell LB, Carlson M, et al. Definition of the best prediction criteria of the time domain signal-averaged electrocardiogram for serious arrhythmic events in the postinfarction period: The Cardiac Arrhythmia Suppression Trial/Signal-Averaged Electrocardiogram (CAST/SAECG) Substudy Investigators. J Am Coll Cardiol 1995; 25: 908-14.
130. El-Sherif N, Turitto G. Nonsustained ventricular tachycardia in ischemic heart disease: when and which pharmacological treatment?. Arch Mal Coeur Vaiss 1996; 89 (Spec No 1): 29-32.
131. Denes P, el-Sherif N, Katz R, Capone R, Carlson M, Mitchell LB, et al. Prognostic significance of signal-averaged electrocardiogram after thrombolytic therapy and/or angioplasty during acute myocardial infarction (CAST substudy): Cardiac Arrhythmia Suppression Trial (CAST) SAECG Substudy Investigators. Am J Cardiol 1994; 74: 216-20.
132. Chandrasekaran S, Hochman JS, Slater JN, Palazzo AM, Morgan CD, Steinberg JS. Relation between infarct artery patency at late angiography after acute myocardial infarction and signal-averaged electrocardiography. Am J Cardiol 1999; 84: 734-6, A8.
133. Hohnloser SH, Klingenheben T, Li YG, Zabel M, Peetermans J, Cohen RJ. T wave alternans as a predictor of recurrent ventricular tachyarrhythmias in ICD recipients: prospective comparison with conventional risk markers. J Cardiovasc Electrophysiol 1998; 9: 1258-68.
134. Rosenbaum DS, Jackson LE, Smith JM, Garan H, Ruskin JN, Cohen RJ. Electrical alternans and vulnerability to ventricular arrhythmias. N Engl J Med 1994; 330: 235-41.
135. Rosenbaum DS, Albrecht P, Cohen RJ. Predicting sudden cardiac death from T wave alternans of the surface electrocardiogram: promise and pitfalls. J Cardiovasc Electrophysiol 1996; 7: 1095-111.
136. Motwani JG, McAlpine H, Kennedy N, Struthers AD. Plasma brain natriuretic peptide as an indicator for angiotensin-converting-enzyme inhibition after myocardial infarction. Lancet 1993; 341: 1109-13.
137. Hall C, Rouleau JL, Moye L, de Champlain J, Bichet D, Klein M, et al. N-terminal proatrial natriuretic factor: An independent predictor of long-term prognosis after myocardial infarction. Circulation 1994; 89: 1934-42.
138. Omland T, Aakvaag A, Bonarjee VV, Caidahl K, Lie RT, Nilsen DW, et al. Plasma brain natriuretic peptide as an indicator of left ventricular systolic function and long-term survival after acute myocardial infarction: Comparison with plasma atrial natriuretic peptide and N-terminal proatrial natriuretic peptide. Circulation 1996; 93: 1963-9.
139. Darbar D, Davidson NC, Gillespie N, Choy AM, Lang CC, Shyr Y, et al. Diagnostic value of B-type natriuretic peptide concentrations in patients with acute myocardial infarction. Am J Cardiol 1996; 78: 284-7.
140. Richards AM, Nicholls MG, Yandle TG, Ikram H, Espiner EA, Turner JG, et al. Neuroendocrine prediction of left ventricular function and heart failure after acute myocardial infarction: The Christchurch Cardioendocrine Research Group. Heart 1999; 81: 114-20.
141. Talwar S, Squire IB, Downie PF, Davies JE, Ng LL. Plasma N terminal pro-brain natriuretic peptide and cardiotrophin 1 are raised in unstable angina. Heart 2000; 84: 421-4.
142. Crilley JG, Farrer M. Left ventricular remodelling and brain natriuretic peptide after first myocardial infarction. Heart 2001; 86: 638-42.
143. Retterstol L, Djurovic S, Bohn M, Bakken A, Erikssen J, Berg K. Plasma N-terminal pro-atrial natriuretic peptide predicts death after premature myocardial infarction, but not as well as radionuclide ejection fraction: A ten-year follow-up study. Scand Cardiovasc J 2001; 35: 373-8.
144. Berger R, Huelsman M, Strecker K, Bojic A, Moser P, Stanek B, et al. B-type natriuretic peptide predicts sudden death in patients with chronic heart failure. Circulation 2002; 105: 2392-7.
145. Richards AM, Nicholls MG, Espiner EA, Lainchbury JG, Troughton RW, Elliott J, et al. B-type natriuretic peptides and ejection fraction for prognosis after myocardial infarction. Circulation 2003; 107: 2786-92.
146. Kinjo K, Sato H, Ohnishi Y, Hishida E, Nakatani D, Mizuno H, et al. Impact of high-sensitivity C-reactive protein on predicting long-term mortality of acute myocardial infarction. Am J Cardiol 2003; 91: 931-5.
147. Anzai T, Yoshikawa T, Takahashi T, Maekawa Y, Okabe T, Asakura Y, et al. Early use of beta-blockers is associated with attenuation of serum C-reactive protein elevation and favorable short-term prognosis after acute myocardial infarction. Cardiology 2003; 99: 47-53.
148. Gheno G, Libardoni M, Zeppellini R, Cucchini F. C-reactive protein on admission as a predictor of in-hospital death in the elderly with acute myocardial infarction. Cardiologia 1999; 44: 1023-8.
149. Griselli M, Herbert J, Hutchinson WL, Taylor KM, Sohail M, Krausz T, et al. C-reactive protein and complement are important mediators of tissue damage in acute myocardial infarction. J Exp Med 1999; 190: 1733-40.
150. Marfella R, Siniscalchi M, Esposito K, Sellitto A, De Fanis U, Romano C, et al. Effects of stress hyperglycemia on acute myocardial infarction: role of inflammatory immune process in functional cardiac outcome. Diabetes Care 2003; 26: 3129-35.
151. Berton G, Cordiano R, Palmieri R, De Toni R, Guarnieri GL, Palatini P. Albumin excretion in diabetic patients in the setting of acute myocardial infarction: association with 3-year mortality. Diabetologia 2004; 47(9): 1511-8.
152. Berton G, Palatini P. Risk stratification after acute myocardial infarction: role of neurohormones, inflammatory markers and albumin excretion rate. Ital Heart J 2003; 4: 295-304.
153. Zimetbaum PJ, Buxton AE, Batsford W, Fisher JD, Hafley GE, Lee KL, et al. Electrocardiographic predictors of arrhythmic death and total mortality in the multicenter unsustained tachycardia trial. Circulation 2004; 110: 766-9.
154. Buxton AE, Lee KL, Hafley GE, Wyse DG, Fisher JD, Lehmann MH, et al. Relation of ejection fraction and inducible ventricular tachycardia to mode of death in patients with coronary artery disease: an analysis of patients enrolled in the multicenter unsustained tachycardia trial. Circulation 2002; 106: 2466-72.
155. Wyse DG, Talajic M, Hafley GE, Buxton AE, Mitchell LB, Kus TK, et al. Antiarrhythmic drug therapy in the Multicenter UnSustained Tachycardia Trial (MUSTT): drug testing and as-treated analysis. J Am Coll Cardiol 2001; 38: 344-51.
156. Bailey JJ, Berson AS, Handelsman H, Hodges M. Utility of current risk stratification tests for predicting major arrhythmic events after myocardial infarction. J Am Coll Cardiol 2001; 38: 1902-11.
157. Hjalmarson A. Prevention of sudden cardiac death with beta blockers. Clin Cardiol 1999; 22 (Suppl 5): V11-V15.
158. Collins R, Peto R, MacMahon S, Hebert P, Fiebach NH, Eberlein KA, et al. Blood pressure, stroke, and coronary heart disease. Part 2, Short-term reductions in blood pressure: overview of randomised drug trials in their epidemiological context. Lancet 1990; 335: 827-38.
159. Staessen JA, Thijs L, Birkenhager WH, Bulpitt CJ, Fagard R. Update on the systolic hypertension in Europe (Syst-Eur) trial: The Syst-Eur Investigators. Hypertension 1999; 33: 1476-7.
160. Staessen JA, Wang JG, Thijs L. Cardiovascular protection and blood pressure reduction: a meta-analysis. Lancet 2001; 358: 1305-15.
161. Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Pérez A, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure: Randomized Aldactone Evaluation Study Investigators. N Engl J Med 1999; 341: 709-17.
162. Pitt B. Aldosterone blockade in patients with acute myocardial infarction. Circulation 2003; 107: 2525-7.
163. Albert CM, Hennekens CH, O'Donnell CJ, Ajani UA, Carey VJ, Willett WC, et al. Fish consumption and risk of sudden cardiac death. JAMA 1998; 279: 23-8.
164. Marchioli R. Omega-3 polyunsaturated fatty acids and cardiovascular diseases. Minerva Cardioangiol 2003; 51: 561-76.
165. Naccarelli GV, Wolbrette DL, Patel HM, Luck JC. Amiodarone: clinical trials. Curr Opin Cardiol 2000; 15: 64-72.
166. Yap YG, Camm AJ. Lessons from antiarrhythmic trials involving class III antiarrhythmic drugs. Am J Cardiol 1999; 84: 83R-89R.
167. Halawa B. Antiarrhythmic agents in the prevention of sudden cardiac death. Pol Merkuriusz Lek 1999; 6: 117-20.
168. Cairns JA. Antiarrhythmic therapy in the post-infarction setting: update from major amiodarone studies. Int J Clin Pract 1998; 52: 422-4.
169. Jafri SM, Borzak S, Goldberger J, Gheorghiade M. Role of antiarrhythmic agents after myocardial infarction with special reference to the EMIAT and CAMIAT trials of amiodarone: European Myocardial Infarct Amiodarone Trial Canadian Amiodarone Myocardial Infarction Trial. Prog Cardiovasc Dis 1998; 41: 65-70.
170. Zamorski M. Amiodarone and mortality in CHF and post-MI. J Fam Pract 1998; 46: 196-7.
171. Amiodarone Trials Meta-Analysis Investigators. Effect of prophylactic amiodarone on mortality after acute myocardial infarction and in congestive heart failure: meta-analysis of individual data from 6500 patients in randomised trials Amiodarone Trials Meta-Analysis Investigators. Lancet 1997; 350: 1417-24.
172. Bigger JT Jr. Prophylactic use of implanted cardiac defibrillators in patients at high risk for ventricular arrhythmias after coronary-artery bypass graft surgery: Coronary Artery Bypass Graft (CABG) Patch Trial Investigators. N Engl J Med 1997; 337: 1569-75.
173. Bigger JT Jr, Whang W, Rottman JN, Kleiger RE, Gottlieb CD, Namerow PB, et al. Mechanisms of death in the CABG Patch trial: a randomized trial of implantable cardiac defibrillator prophylaxis in patients at high risk of death after coronary artery bypass graft surgery. Circulation 1999; 99: 1416-21.
174. Zareba W. Implantable cardioverter defibrillator therapy in postinfarction patients. Curr Opin Cardiol 2004; 19: 619-24.
175. Salukhe TV, Dimopoulos K, Francis D. Cardiac resynchronisation may reduce all-cause mortality: meta-analysis of preliminary COMPANION data with CONTAK-CD, InSync ICD, MIRACLE and MUSTIC. Int J Cardiol 2004; 93: 101-3.
176. Gregoratos G, Abrams J, Epstein AE, Freedman RA, Hayes DL, Hlatky MA, et al. ACC/AHA/NASPE 2002 guideline update for implantation of cardiac pacemakers and antiarrhythmia devices: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (ACC/AHA/NASPE Committee to Update the 1998 Pacemaker Guidelines). Circulation 2002; 106: 2145-61.
177. Antman EM, Anbe DT, Armstrong PW, Bates ER, Green LA, Hand M, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction-executive summary. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to revise the 1999 guidelines for the management of patients with acute myocardial infarction). J Am Coll Cardiol 2004; 44: 671-719.
178. Daoud EG, Niebauer M, Kou WH, Man KC, Horwood L, Morady F, et al. Incidence of implantable defibrillator discharges after coronary revascularization in survivors of ischemic sudden cardiac death. Am Heart J 1995; 130: 277-80.
179. Cleland JG, Ghosh J, Freemantle N, Kaye GC, Nasir M, Clark AL, et al. Clinical trials update and cumulative meta-analyses from the American College of Cardiology: WATCH, SCD-HeFT, DINAMIT, CASINO, INSPIRE, STRATUS-US, RIO-Lipids and cardiac resynchronisation therapy in heart failure. Eur J Heart Fail 2004; 6: 501-8.
180. Grimm W, Alter P, Maisch B. Arrhythmia risk stratification with regard to prophylactic implantable defibrillator therapy in patients with dilated cardiomyopathy: Results of MACAS, DEFINITE, and SCD-HeFT. Herz 2004; 29: 348-52.
181. Domanski MJ, Sakseena S, Epstein AE, Hallstrom AP, Brodsky MA, Kim S, et al. Relative effectiveness of the implantable cardioverter-defibrillator and antiarrhythmic drugs in patients with varying degrees of left ventricular dysfunction who have survived malignant ventricular arrhythmias: AVID Investigators1 Antiarrhythmics Versus Implantable Defibrillators. J Am Coll Cardiol 1999; 34: 1090-5.
182. Siebels J, Cappato R, Ruppel R, Schneider MA, Kuck KH. Preliminary results of the Cardiac Arrest Study Hamburg (CASH): CASH Investigators. Am J Cardiol 1993; 72: 109F-113F.
]]>