PEDIATRÍA
CUARTO PREMIO
Soporte respiratorio no invasivo en el fallo respiratorio agudo del niño: análisis de un grupo de pacientes asistidos en una UCIP privada
Non invasive respiratory support in child acute respiratory failure: analysis of a group of patients seen in a private PICU
Jesús Serra1, Sebastian González1, Leticia Rodríguez2, Carina Viejo2, Bernardo Alonso3
1. Pediatra Guardia CIPe.
2. Asesores estadísticos CIPe.
3. Supervisor CIPe.
Unidad de Cuidados Intensivos Pediátricos Sanatorio Casa de Galicia ]]>
Trabajo inédito.
Declaramos no tener conflictos de intereses.
Resumen
Introducción: el fallo respiratorio agudo (FRA) es la principal causa de morbimortalidad pediátrica. La ventilación mecánica no invasiva (VMNI) y la oxigenoterapia de alto flujo (CNAF) son cada vez más utilizados en las Unidades de Cuidados Intensivos pediátricos (UCIP) como alternativa a la ventilación mecánica invasiva (VMI).
Objetivo: describir el perfil clínico-evolutivo de niños ingresados a una UCIP por FRA y tratados con VMNI-CNAF entre marzo y octubre de 2014.
Metodología: corte transversal y observacional. Niños ingresados por FRA y tratados con VMNI-CNAF. Se clasificaron según éxito o fracaso (necesidad de VMI). Se calificó la gravedad según Escores PIM2 y Tal.
Resultados: de 80 casos, 39 cumplieron criterios de inclusión, 15.4% fracasaron. Las causas de fracaso: depresión neuropsíquica, fallo cardiovascular y trabajo respiratorio. La mediana de edad fue 7 meses. Los que requirieron VMI eran menores de 1 año. Los indicadores de gravedad fueron similares en ambos grupos, así como sus comorbilidades. En cuatro de cada cinco pacientes se utilizó CNAF a un flujo promedio de 1,5 l/kg/min. El 64% de los diagnósticos fue bronquiolitis. Los días de soporte respiratorio requeridos fueron menores en los niños atendidos con métodos no invasivos. Ningún paciente falleció.
Discusión: esta representa la primera descripción nacional de tratamiento ventilatorio no invasivo en el entorno de una UCIP. La VMNI-CNAF mostró ser una estrategia segura y exitosa en la gran mayoría de pacientes. Este trabajo servirá para planificación y elaboración de futuras investigaciones en UCIP en la era de los cuidados respiratorios no invasivos.
Palabras clave: ]]>
VENTILACIÓN NO INVASIVA
INSUFICIENCIA RESPIRATORIA
TERAPIA POR INHALACIÓN DE
OXÍGENO
UNIDADES DE CUIDADO INTENSIVO
PEDIÁTRICO
Summary
Introduction: acute respiratory failure (ARF) is the main cause of pediatric morbimortality. Non invasive ventilation (NIV) and high flow nasal cannula (HFNC) are increasingly being used un Pediatric Intensive Care Units (PICU) as an alternative to invasive mechanical ventilation (MV).
Aim: to describe the characteristics and clinical course of children admitted to our PICU for ARF and treated with NIV and HFNC between March and October 2014. ]]>
Methods: cross-sectional and observational study. Children admitted with ARF and treated with NIV and HFNC were included. They were classified in two groups: “responders” and “failure” (failure was defined if MV was needed). Severity was scored by PIM2 and Tal scores.
Results: of 80 patients admitted for ARF, 39 were included for analysis, failure rate was 15.4%. Failure causes were: neurological failure, cardiovascular failure and work of breathing. Median age was 7 months. All who needed MV were younger than one year. Severity scores were similar in both groups, as well as their comorbidities. 4 out of 5 patients were treated with CNAF. Mean flow was 1,5 l/kg/min. Most frequent diagnosis was Bronchiolitis in 64%. Those treated with non invasive methods needed less days of respiratory support. No patient died and no complications were recorded.
Conclusion: this represents the first national description of non invasive respiratory support in a PICU environment. NIV and HFNC showed to be a safe and successful strategy in most patients admitted with ARF. This results will help to plan and elaborate further research in the age of pediatric non invasive respiratory care.
Key words:
NONINVASIVE VENTILATION
RESPIRATORY INSUFFICIENCY
OXYGEN INHALATION THERAPY
INTENSIVE CARE UNITS, PEDIATRIC
La ventilación mecánica no invasiva (VMNI), definida como aquella que no requiere prótesis endotraqueal, es una terapia de soporte que ha surgido en los últimos años como una alternativa a la ventilación mecánica invasiva (VMI) en el FRA(5). La VMNI se realiza a través de diferentes interfaces (máscaras buco nasales, máscaras faciales, piezas nasales) y utiliza presión positiva de distensión continua (CPAP) o con dos niveles de presión (BIPAP).
La capacidad para evitar la intubación endotraqueal usando VMNI significa que la vía aérea superior se mantiene intacta y las funciones fisiológicas y mecanismos de defensa de las vías respiratorias se conservan. La utilización de la VMNI previene de potenciales complicaciones de la VMI, principalmente las asociadas a infecciones, daño pulmonar y bronquiolitis obliterante(6-10).
Varios trabajos en adultos han demostrado la eficacia de la VMNI en el tratamiento, reducción de la estadía hospitalaria y de la necesidad de intubación orotraqueal (IOT) en el fallo respiratorio agudo(11-14). En pediatría cada vez son más los estudios que destacan la utilización de la VMNI en la UCIP para tratamiento de la insuficiencia respiratoria, y particularmente la secundaria a bronquiolitis aguda(15-27). Estudios europeos y australianos(28-30) han demostrado que los pediatras adoptaron la VMNI como terapia de soporte estándar en el FRA, suplantando a la VMI en el último decenio, obteniendo menor morbilidad global y un adecuado balance costo- efectividad de los niños que requieren internación en UCIP.
La cánula nasal de alto flujo (CNAF) es otra terapia de soporte que en el último tiempo ha ganado su lugar en el tratamiento del fallo respiratorio en todas las edades(31-35) y al igual que con la VMNI hay varios trabajos que demuestran la reducción de los requerimientos de IOT con su uso(36-43). Recientemente Frat y colaboradores(44) demostraron que el uso de CNAF en el fallo respiratorio hipoxémico del adulto disminuye la mortalidad. La construcción de la evidencia con esta terapia en UCIP está en pleno crecimiento.
A pesar de la amplia difusión que han tenido estas terapias no invasivas en nuestro medio, no hay descripciones locales que analicen la evolución de los pacientes sometidos a estas técnicas como terapia de soporte al ingreso a UCIP.
Objetivos
Población y métodos
Este es un estudio descriptivo, y de corte transversal.
Se excluyeron: aquellos niños cuyo inicio de VMI fue previo al ingreso, con fallo respiratorio secundario (origen extrapulmonar), pacientes que no requirieran soporte respiratorio; y pacientes con orden de no reanimación y/o limitación esfuerzo terapéutico.
La fuente de información fue la historia clínica. Se elaboró una planilla Excel (Microsoft 2007 ®) donde se registraron las siguientes variables: edad, sexo, peso, morbilidad previa, diagnóstico etiológico del fallo respiratorio, germen aislado, frecuencia respiratoria al ingreso, saturación de O2, intensidad del síndrome funcional respiratorio valorado para los menores de 2 años con el escore de Tal, modificado por Bello-Sehabiague(46) y para los mayores de 2 años con el Pediatric Asthma Score(47); gasometría al ingreso y características de la radiografía de tórax (RxTx) leídas por clínico actuante (dividiéndolo en tres patrones infiltrado intersticial difuso, hiperinsuflación pulmonar y/o imagen de consolidación pulmonar). Además, se recogió información acerca del tipo de soporte respiratorio realizado duración, valores máximos de presión y flujos utilizados, así como también requerimiento de sedoanalgesia, días de internación y mortalidad. Se registraron los valores superiores de frecuencia respiratoria, frecuencia cardíaca y los inferiores de saturación de O2 durante el soporte no invasivo, así como también si había presencia en la gasometría de acidosis metabólica o respiratoria, hipercapnia o hipoxemia durante el tratamiento.
Se recogieron los criterios utilizados por el médico de guardia para iniciar VMI.
La VMNI y el CNAF fueron proporcionados por los equipos disponibles en la Unidad: equipos Resmed Stellar 150®, con máscaras buco-nasales. En los pacientes menores de 30 días se realizó CPAP con equipo Neumovent Graphnet® con prolongaciones nasales o piezas nasales BabyFlow Dräger®. El CNAF utilizado fue el elaborado por ingeniería biomédica de la institución a partir de flujómetro de aire, y de oxígeno con conexión a pieza en Y y posterior humidificación y calefaccionamiento con caldera Fisher Paykel ®. Las cánulas nasales por protocolo no superaron la mitad de ancho de las narinas. El estudio contó con la autorización institucional.
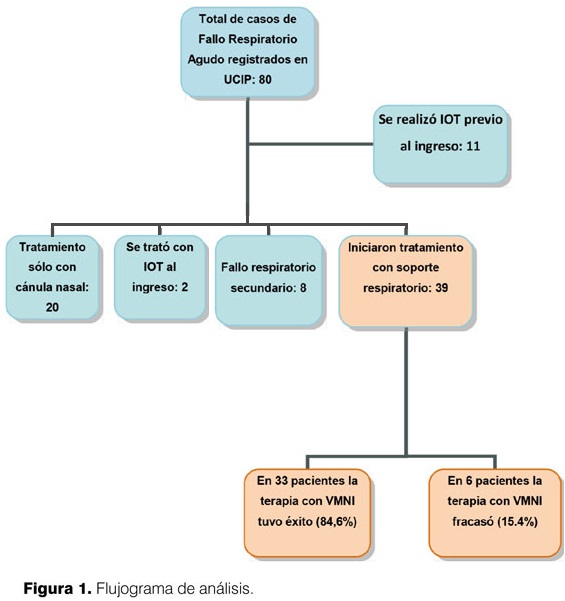
De los 80 pacientes que ingresaron a UCIP con fallo respiratorio agudo, se analizaron aquellos que cumplieron los criterios de inclusión. El flujograma de análisis se muestra en la figura 1.
La estrategia de análisis consistió en estudiar a la población tratada inicialmente con los diferentes métodos de soporte respiratorio no invasivo y describir su desempeño evaluado en “éxito” o “fracaso” del tratamiento.
Se consideró que el tratamiento tuvo éxito en aquellos pacientes que no requirieron IOT y, por el contrario, fracaso en aquellos que sí lo requirieron.
De los 39 pacientes estudiados 15,4% requirieron VMI. Las causas de inicio de VMI fueron: depresión neuropsiquica, compromiso hemodinámico, hipoxemia mantenida, obstrucción de vía aérea superior, y síndrome funcional respiratorio con signos de agotamiento. Ninguno de los pacientes falleció.
En la tabla 1 se muestran las características de la población estudiada así como los estadísticos calculados para el total de la población y para ambos grupos.
El PIM2, escore de Tal y PAS presentaron valores similares en ambos grupos. El PIM2 tuvo una mediana de 7,1 % en todos los pacientes, mientras que este valor fue de 7,4% para los pacientes que solo se trataron con métodos no invasivos y 6,2 % para los pacientes que terminaron siendo asistidos con VMI. En tanto el escore de Tal, tuvo una mediana de 8 en el total de la población, con una mediana de 9 para los pacientes que terminaron siendo asistidos con VMI y de 8 para los que solo recibieron tratamiento con soporte respiratorio no invasivo.
La mediana de frecuencia cardíaca fue de 185,5 cpm en el grupo de fracaso y de 174,5 cpm en el grupo de éxito. La mediana de frecuencia respiratoria en la población total fue de 64 rpm, nos faltan datos en el grupo de fracaso por lo que no se realizó análisis de esta variable.
La mediana de la FiO2 requerida por los pacientes que fallaron fue mayor que en los que tuvieron éxito (0,4 versus 0,3). El flujo máximo de CNAF utilizado tuvo una mediana de 1,4 l/min/kg en el grupo de éxito, y de 1,3 l/min/kg en el de fracaso, con un máximo de 3,4 l/min/kg y 2,1 l/min/kg respectivamente.
El método de soporte más utilizado en este grupo (cuatro de cada cinco pacientes) fue el CNAF.
Del total de pacientes, la patología más frecuente fue la bronquiolitis (64%), siendo el VRS el germen predominante (38%), mientras que el 15,4% ingresó con neumonía aguda y, 7,7% con crisis asmática. El diagnóstico al ingreso entre grupos tuvo una distribución similar. La mayor parte de los pacientes fue diagnosticada con bronquiolitis.
Cabe destacar que no se observaron diferencias sustanciales entre las comorbilidades entre los grupos, en cada grupo, más de la mitad de los pacientes no tenían enfermedad previa.
En todos los pacientes que se asistieron con VMNI y también en aquellos con VMI requirieron la utilización de algún tipo de sedoanalgesia. En el grupo de fracaso cuatro niños desarrollaron síndrome de abstinencia. Se destaca en un paciente que estuvo en VMNI una reacción paradojal a las benzodiacepinas. No se utilizó ningún tipo de sedoanalgesia en aquellos pacientes tratados con CNAF.
En los pacientes que terminaron siendo asistidos con VMI, se observa que el valor máximo de días de soporte respiratorio requerido fue superior que el valor máximo observado en los pacientes tratados solamente con soporte respiratorio no invasivo, independientemente del tipo de tratamiento. El valor máximo observado con CNAF fue de 6 días, con CPAP 3 días y con BiPAP 5 días.
Los pacientes atendidos con VMNI-CNAF no presentaron complicaciones derivadas de la misma.
Discusión
La VMNI tiene hoy, un lugar predominante en la atención del Fallo respiratorio agudo pediátrico, siendo el estándard de cuidados de inicio en los centros mundiales con mejores resultados, mejorando la morbilidad infantil por esta causa y los costos derivados de su atención (24, 29). El rol protectivo frente a la necesidad de IOT y VMI de las diferentes técnicas de soporte no invasivos han sido probados en diferentes estudios(10,42).
Experiencias uruguayas recientes(27,31) fuera del ámbito de UCIP han mostrado que se puede hacer VMNI con seguridad y buenos resultados. En nuestra UCIP, por cada año que pasa, se utiliza menos VMI y más métodos de soporte respiratorio no invasivo, predominando la CNAF, como se muestra en la Gráfica 2 (registros históricos no publicados). Esta tendencia coincide con la tendencia mundial de los centros de referencia(28,29,30).
La experiencia que se presenta, en la que se refleja que la enorme mayoría de los niños atendidos no necesitaron VMI, nos ha enseñado que la curva de aprendizaje en VMNI y sus diferentes técnicas en nuestra UCIP (y que es compartida por muchas UCIP de nuestro medio) han posibilitado que hoy no se intuben niños que antes sí.Es de importancia destacar que el reducido número de pacientes y el hecho de que se trata de datos de una sola institución, no permite generalizar los resultados al resto de la población. El análisis estadístico realizado fue puramente descriptivo. Sin embargo, se logró realizar un profundo análisis descriptivo que nos permite afirmar que los escores de gravedad entre ambos grupos fue similar. Lo anterior permite plantear la hipótesis tentativa de que no había diferencias sustanciales en lo que a la gravedad de los pacientes se refiere. Aunque son necesarios futuros estudios que diluciden este punto, podemos observar que el criterio clínico fue el predominante para decidir el inicio de la VMI.
La duración en días de VMI promedio de los niños estudiados fue similar a la de los pacientes que ingresaron con IOT y VMI previa al ingreso a nuestra UCIP y coincide con nuestros registros históricos.
Cabe destacar el gran predominio del uso de CNAF como soporte respiratorio. Este método muy bien tolerado por los pacientes ha ido ganando cada vez más espacio en nuestra UCIP y es actualmente el más utilizado. Se puede observar que los pacientes que fallaron recibieron menos flujo promedio que los que tuvieron éxito y en ambos grupos se utilizaron flujos menores que los recomendados de 2 l/kg/min(32), razón por la cual hoy día en nuestra UCIP es estándar tener ese objetivo mínimo de flujo.
Esta serie representa la primera descripción nacional de uso de VMNI y CNAF de niños en el entorno de una UCIP. Pudimos mostrar con nuestra experiencia que es factible utilizar con seguridad y buenos resultados los diferentes métodos no invasivos de soporte respiratorio en niños con FRA de etiología heterogénea, siendo la bronquiolitis la enfermedad predominante. Podemos afirmar que la VMNI y principalmente el CNAF, es el estándar de cuidados respiratorios al ingreso de estos niños en nuestra UCIP. Serán necesarios futuros estudios clínicos randomizados controlados para determinar la efectividad clínica del método a gran escala y su perfil de seguridad. Aunque en una reciente revisión Cochrane falló en demostrar esto(49), será cuestión de tiempo para seguir construyendo evidencia en este sentido. Experiencias regionales contemporáneas en entornos similares al nuestro(50) muestran que estas técnicas son seguras y reproducibles.
Este análisis de pacientes, junto a las experiencias de intercambio con UCIP similares a la nuestra motivó la realización de un protocolo de actuación en cuidados respiratorios no invasivos para su aplicación tanto dentro como fuera de nuestra UCIP como estándar de cuidados. Estudios colaborativos en esta línea son fundamentales para la evaluación clínica de los mismos.
Conclusiones
Esta experiencia representa la primera descripción nacional de tratamiento con soporte ventilatorio no invasivo del fallo respiratorio agudo pediátrico en el entorno de una UCIP.
La VMNI-CNAF mostró ser una estrategia segura y exitosa en la gran mayoría de pacientes analizados lo que se corresponde con los resultados comunicados en los centros de referencia mundiales.
1. Ralston SL, Lieberthal AS, Meissner HC, Alverson BK, Baley JE, Gadomski AM, et al; American Academy of Pediatrics. Clinical practice guideline: the diagnosis, management, and prevention of bronchiolitis. Pediatrics 2014; 134(5):e1474-502. Disponible en: http://pediatrics.aappublications.org/content/pediatrics/134/5/e1474.full.pdf. [Consulta: 15 Mayo 2015].
2. Hasegawa K, Tsugawa Y, Brown D, Mansbach J, Camargo Jr C. Trends in Bronchiolitis Hospitalizations in the United States, 2000–2009. Pediatrics 2013; 132(1):28–36.
3. Prais D, Schonfeld T, Amir J. Admission to the Intensive Care Unit for respiratory syncytial virus bronchiolitis: a national survey before palivizumab use. Pediatrics 2003; 112(3):548-52.
4. Noli P, Geymonat M, Bustelo E, Muñoz J, Saibene S, Dall Orso P, et al. Infecciones respiratorias agudas bajas de causa viral en niños hospitalizados en el Centro Hospitalario Pereira Rossell: características clínicas y terapéuticas. Arch Pediatr Urug 2012; 83(4):244-9.
5. Menchaca A, Mercado S, Alberti M. Aplicación de ventilación no invasiva en el niño. Arch Pediatr Urug 2005; 76(3):243-51.
6. Girou E, Schortgen F, Delclaux C, Brun-Buisson C, Blot F, Lefort Y, et al. Association of noninvasive ventilation with nosocomial infections and survival in critically ill patients. JAMA 2000; 284(18):2361-7.
7. Colom AJ, Teper AM, Vollmer WM, Diette GB. Risk factors for the development of bronchiolitis obliterans in children with bronchiolitis. Thorax 2006; 61(6):503-6.
8. Cabrini L, Landoni G, Oriani A, Plumari VP, Nobile L, Greco M, et al. Noninvasive ventilation and survival in acute care settings: a comprehensive systematic review and metaanalysis of randomized controlled trials. Crit Care Med 2015; 43(4):880-8.
9. Contou D, Fragnoli C, Cordoba-Izquierdo A, Boissier F, Brun-Buisson C, Thille A. Noninvasive Ventilation for Acute Hypercapnic Respiratory Failure: Intubation Rate in an Experienced Unit. Respir Care 2013; 58(12):2045-52.
10. Yañez LJ, Yunge M, Emilfork M, Lapadula M, Alcántara A, Fernández C, et al. A prospective, randomized, controlled trial of noninvasive ventilation in pediatric acute respiratory failure. Pediatr Crit Care Med 2008; 9(5):484-9.
11. Meduri GU, Turner RE, Abou-Shala N, Wunderink R, Tolley E. Noninvasive positive pressure ventilation via face mask. First-line intervention in patients with acute hypercapnic and hypoxemic respiratory failure. Chest 1996; 109(1): 179-93.
12. Kramer N, Meyer TJ, Meharg J, Cece RD, Hill NS. Randomized, prospective trial of noninvasive positive pressure ventilation in acute respiratory failure. Am J Respir Crit Care Med 1995; 151(6):1799-806.
13. Ferrer M, Esquinas A, León M, González G, Alarcón A, Torres A. Noninvasive ventilation in severe hypoxemic respiratory failure: a randomized clinical trial. Am J Respir Crit Care Med 2003; 168(12):1438-44.
15. Beasley JM, Jones SE. Continuous positive airway pressure in bronchiolitis. Br Med J (Clin Res Ed) 1981; 283(6305): 1506-8.
16. Lazner MR, Basu AP, Klonin H. Non-invasive ventilation for severe bronchiolitis: analysis and evidence. Pediatr Pulmonol 2012; 47(9):909-16.
17. Cambonie G, Milési C, Jaber S, Amsallem F, Barbotte E, Picaud JC, et al. Nasal continuous positive airway pressure decreases respiratory muscles overload in young infants with severe acute viral bronchiolitis. Intensive Care Med 2008; 34(10):1865-72.
18. Milési C, Matecki S, Jaber S, Mura T, Jacquot A, Pidoux O, et al. 6 cmH2O continuous positive airway pressure versus conventional oxygen therapy in severe viral bronchiolitis: a randomized trial. Pediatr Pulmonol 2013; 48(1):45-51.
19. Oñoro G, Pérez Suárez E, Iglesias Bouzas M, Serrano A, Martínez De Azagra A, García-Teresa MA, et al. Bronquiolitis grave. Cambios epidemiológicos y de soporte respiratorio. An Pediatr (Barc) 2011; 74(6):371-6.
20. Essouri S, Durand P, Chevret L, Balu L, Devictor D, Fauroux B, et al. Optimal level of nasal continuous positive airway pressure in severe viral bronchiolitis. Intensive Care Med 2011; 37(12):2002-7.
21. Balfour-Lynn RE, Marsh G, Gorayi D, Elahi E, LaRovere J. Non-invasive ventilation for children with acute respiratory failure in the developing world: literature review and an implementation example. Paediatr Respir Rev 2014; 15(2):181-7.
22. Borckink I, Essouri S, Laurent M, Albers MJ, Burgerhof JG, Tissières P, et al. Infants with severe respiratory syncytial virus needed less ventilator time with nasal continuous airways pressure then invasive mechanical ventilation. Acta Paediatr 2014; 103(1):81-5.
23. Nizarali Z, Cabral M, Silvestre C, Abadesso C, Nunes P, Loureiro H, et al. Ventilação não invasiva na insuficiência respiratória aguda na bronquiolite por vírus sincicial respiratorio. Rev Bras Ter Intensiva 2012; 24(4):375-80.
24. Javouhey E, Barats A, Richard N, Stamm D, Floret D. Non-invasive ventilation as primary ventilatory support for infants with severe bronchiolitis. Intensive Care Med 2008; 34(9):1608-14.
25. James CS, Hallewell CP, James DP, Wade A, Mok QQ. Predicting the success of non-invasive ventilation in preventing intubation and re-intubation in the paediatric intensive care unit. Intensive Care Med 2011; 37(12):1994-2001.
26. Girault C, Briel A, Hellot MF, Tamion F, Woinet D, Leroy J, et al. Noninvasive mechanical ventilation in clinical practice: a 2-year experience in a medical intensive care unit. Crit Care Med 2003; 31(2):552-9.
27. Alonso B, Boulay M, Dall’Orso P, Allegretti M, Berterretche R, Solá L, et al. Ventilación no invasiva en menores de dos años internados en sala con infección respiratoria aguda baja: posibles factores predictivos de éxito y de fracaso. Arch Pediatr Urug 2012; 83(4):250-5.
28. Ganu SS, Gautam A, Wilkins B, Egan J. Increase in use of non-invasive ventilation for infants with severe bronchiolitis is associated with decline in intubation rates over a decade. Intensive Care Med 2012; 38(7):1177-83.
29. Essouri S, Laurent M, Chevret L, Durand P, Ecochard E, Gajdos V, et al. Improved clinical and economic outcomes in severe bronchiolitis with pre-emptive nCPAP ventilatory strategy. Intensive Care Med 2014; 40(1):84-91.
30. Toledo del Castillo B, Fernández Lafever S, López Sanguos C, Díaz-Chirón Sánchez L, Sánchez da Silva M, López-Herce J. Evolución de la ventilación mecánica no invasiva en la bronquiolitis. An Pediatr (Barc) 2015; 83(2):117-22.
31. Alonso B, Tejera J, Dall´Orso P, Boulay M, Ambrois G, Guerra L, et al. Oxigenoterapia de alto flujo en niños con infección respiratoria aguda baja e insuficiencia respiratoria. Arch Pediatr Urug 2012; 83(2):111-6.
32. Lee JH, Rehder KJ, Williford L, Cheifetz IM, Turner DA. Use of high flow nasal cannula in critically ill infants, children, and adults: a critical review of the literature. Intensive Care Med 2013; 39(2):247-57.
33. Frat JP, Brugiere B, Ragot S, Chatellier D, Veinstein A, Goudet V, et al. Sequential application of oxygen therapy via high-flow nasal cannula and noninvasive ventilation in acute respiratory failure: an observational pilot study. Respir Care 2015; 60(2):170-8.
34. Messika J, Ben Ahmed K, Gaudry S, Miguel-Montanes R, Rafat C, Sztrymf B, et al. Use of High-Flow Nasal Cannula Oxygen Therapy in Subjects With ARDS: A 1-Year Observational Study. Respir Care 2015; 60(2):162-9.
35. Yoder BA, Stoddard RA, Li M, King J, Dirnberger DR, Abbasi S. Heated, humidified high-flow nasal cannula versus nasal CPAP for respiratory support in neonates. Pediatrics 2013; 131(5):e1482-90.
36. Hough JL, Pham TM, Schibler A. Physiologic effect of high-flow nasal cannula in infants with bronchiolitis. Pediatr Crit Care Med 2014; 15(5):e214-9.
37. Rubin S, Ghuman A, Deakers T, Khemani R, Ross P, Newth CJ. Effort of breathing in children receiving high-flow nasal cannula. Pediatr Crit Care Med 2014; 15(1):1-6.
38. Milési C, Baleine J, Matecki S, Durand S, Combes C, Novais AR, et al. Is treatment with a high flow nasal cannula effective in acute viral bronchiolitis?: a physiologic study. Intensive Care Med 2013; 39(6):1088-94.
39. McKiernan C, Chua LC, Visintainer PF, Allen H. High flow nasal cannulae therapy in infants with bronchiolitis. J Pediatr 2010; 156(4):634-8.
40. González Martínez F, González Sánchez M, Rodríguez Fernández R. Impacto clínico de la implantación de la ventilación por alto flujo de oxígeno en el tratamiento de la bronquiolitis en una planta de hospitalización pediátrica. An Pediatr (Barc) 2013; 78(4):210-5.
41. Mayfield S, Bogossian F, O’Malley L, Schibler A. High-flow nasal cannula oxygen therapy for infants with bronchiolitis: pilot study. J Paediatr Child Health 2014; 50(5):373-8.
43. Haq I, Gopalakaje S, Fenton AC, McKean MC, J O’Brien C, Brodlie M. The evidence for high flow nasal cannula devices in infants. Paediatr Respir Rev 2014; 15(2):124-34.
44. Frat JP, Thille AW, Mercat A, Girault C, Ragot S, Perbet S, et al; FLORALI Study Group; REVA Network. High-flow oxygen through nasal cannula in acute hypoxemic respiratory failure. N Engl J Med 2015; 372(23):2185-96.
45. Goldstein B, Giroir B, Randolph A; International Consensus Conference on Pediatric Sepsis. International pediatric sepsis consensus conference: definitions for sepsis and organ dysfunction in pediatrics. Pediatr Crit Care Med 2005; 6(1):2-8.
46. Tal A, Bavilski C, Yohai D, Bearman J, Gorodischer R, Moses S, et al. Dexamethasone and Salbutamol in the treatment of acute wheezing in infants. Pediatrics 1983; 71(1): 13-8.
47. Qureshi F, Pestian J, Davis P, Zaritsky A. Effect of nebulized ipratropium on the hospitalization rates of children with asthma. N Engl J Med. 1998;339(15):1030-5.
48. Slater A, Shann F, Pearson G; Paediatric Index of Mortality (PIM) Study Group. PIM2: a revised version of the Paediatric Index of Mortality. Intensive Care Med. 2003 Feb;29(2):278-85.
49. Mayfield S, Jauncey-Cooke J, Hough JL, Schibler A, Gibbons K, Bogossian F. High-flow nasal cannula therapy for respiratory support in children. Cochrane Database Syst Rev. 2014 Mar 7; 3: CD009850.
50. Wegner A, Cespedes F P, Godoy M ML, Erices B P, Urrutia C L, Venthur U C, et al. High flow nasal cannula in infants: Experience in a critical patient unit. Rev Chil Pediatr. 2015 May-Jun; 86(3):173-81.
Correspondencia: Dr. Jesús Serra.
Correo electrónico: jesusalbertoserra@gmail.com