Artículo original
pnea del sueño y sistema nervioso autónomo
Geoffrey EJ Seaborn, Helen Pang, Selim G Akl, y colaboradores
Autonomic profile of patients referred to a sleep disorder clinic: impact of CPAP on the autonomic nervous system
Geoffrey EJ Seaborn, Helen Pang, Selim G Akl, Damian P Redfearn, Christopher S Simpson, Michael Fitzpatrick, Peter W Munt, Adrian Baranchuk
Correspondencia: Dr Adrian Baranchuk, MD FACC FRCPC. Associate Professor of Medicine. Cardiac Electrophysiology and Pacing. Kingston General Hospital K7L 2V7. Queen's University.
Correo electrónico: barancha@kgh.kari.net
Recibido mayo 22, 2012; aceptado junio 19, 2012.
Introducción: la apnea obstructiva del sueño (AOS) severa ha sido asociada con disfunción autonómica. La presión positiva continua en la vía aérea (CPAP) es el tratamiento estándar para la AOS, aun cuando su impacto sobre la disfunción autonómica no haya sido plenamente investigado. La variabilidad de la frecuencia cardíaca (VFC) es una técnica cuantitativa no invasiva para la evaluación de la actividad autonómica. Nuestro objetivo fue determinar si los pacientes con AOS severa presentan niveles mayores de disfunción autonómica que los pacientes con un índice de apnea-hipopnea (IAH) normal, y si la CPAP mejora los parámetros de VFC a la vez que mejora el IAH.
Métodos: todos los pacientes fueron sometidos a una polisomnografía (PSG) completa en una clínica de trastornos del sueño. Se definió como severa a una AOS que tuviera un IAH ³ 30 (eventos por hora), y se definió al grupo control como aquellos que tuvieran un IAH < 5. Se calculó la VFC antes y después de la CPAP, analizando trazados electrocardiogáficos de 10 minutos, conforme las pautas de normalización. Los pacientes con AOS severa fueron tratados con CPAP durante un período de 4-6 semanas (titulados durante la polisomnografía), y los pacientes control no recibieron ninguna intervención entre sus dos registros de electrocardiograma (ECG).
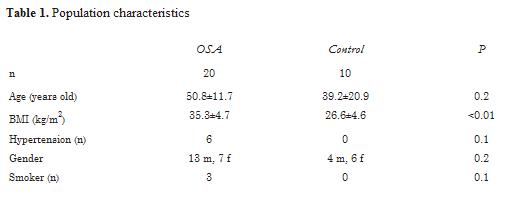
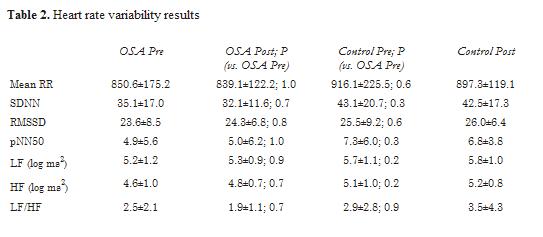
Resultados: el estudio incluyó a un total de 20 pacientes con AOS severa y 10 controles. En los pacientes con AOS severa, el IAH se redujo al utilizar CPAP de 38,0 ± 11,0 a 23,0 ± 11,0 (p<0,01). Aparte de una diferencia significativa en el índice de masa corporl (IMC) entre los paciente con AOS y los controles (35,3±4,7 versus 26,6±4,6 kg/m2, p<0,01), los grupos fueron comparables en cuanto a edad, condición de hipertensión y género. No hubo ninguna diferencia significativa (p<0,05) en ningún parámetro de VFC entre los pacientes con AOS severa y los controles, ni entre los pacientes con AOS antes y después de CPAP (tabla 2).
Conclusión: en una población derivada a una clínica de trastornos del sueño, los pacientes con AOS severa presentaron el mismo perfil autonómico que los pacientes sin AOS. La corrección de AOS mediante CPAP no se acompañó de alteraciones en la actividad autonómica.
Palabras clave:
SÍNDROMES DE LA APNEA DE SUEÑO
FRECUENCIA CARDÍACA ]]>
PRESIÓN DE LAS VÍAS AÉREAS POSITIVA CONTINUA
Summary
Introduction: severe obstructive sleep apnea (OSA) has been associated with autonomic dysfunction. Continuous positive airway pressure (CPAP) is standard treatment for OSA, although its impact on autonomic dysfunction was not fully investigated. Heart rate variability (HRV) is a non-invasive quantitative technique for assessment of autonomic activity. We aimed to determine if patients with severe OSA exhibit greater levels of autonomic dysfunction than patients with normal apnea-hypopnea index (AHI), and if CPAP improves heart rate variability (HRV) parameters while improving AHI.
Methods: all patients underwent full polysomnography (PSG) at a Sleep Disorder Clinic. Severe OSA was defined as AHI ³ 30 (events per hour), and control was defined as AHI < 5. HRV was calculated pre and post-CPAP from a 10-minute electrocardiogram (ECG) recording in accordance with guidelines for standardization. Patients with severe OSA were treated with CPAP for a period of 4-6 weeks (titrated during PSG), and control patients underwent no intervention between their two ECG recordings.
Results: a total of 20 patients with severe OSA and 10 controls were included (Table 1). In patients with severe OSA, AHI was reduced by CPAP from 38.0 ± 11.0 to 23.0 ± 11.0 (P<0.01). Aside from a significant difference in BMI between OSA patients and controls (35.3±4.7 vs. 26.6±4.6 kg/m2, P<0.01), groups were comparable in age, hypertension, and gender. There was no significant difference (P<0.05) in any HRV parameters between patients with severe OSA and controls, and between OSA patients pre- and post-CPAP (table 2).
]]> Conclusion: in a population referred to a Sleep Disorder Clinic, patients with severe OSA presented the same autonomic profile as patients with no OSA. Correction of OSA by CPAP was not associated with changes in autonomic activity.
Key words:
CONTINUOUS POSITIVE AIRWAY PRESSURE
SLEEP APNEA SYNDROMES
HEART RATEY
Introduction
]]> It is estimated that 1 in 5 adults have at least mild obstructive sleep apnea (OSA) (1), a condition that is associated with hypertension (2), cardiac arrhythmia (3), stroke (4), congestive heart failure (5), daytime sleepiness (6), abnormal brain morphology (7), diabetes mellitus (8), and autonomic dysfunction (9). Continuous positive airway pressure (CPAP) is standard treatment for OSA. Heart rate variability (HRV) analysis is a non-invasive and quantitative technique for assessment of autonomic activity. We hypothesized that patients with severe OSA may exhibit greater levels of autonomic dysfunction than patients with normal apnea-hypopnea index (AHI), and that CPAP may improve HRV parameters while improving AHI.Methods
All patients underwent full polysomnography (PSG) at a Sleep Disorder Clinic. Severe OSA was defined as an AHI ³ 30 (events per hour). Control was defined as AHI < 5. Patients with diabetes mellitus (DM), implantable devices, cardiac abnormalities, beta- and calcium-blocking medications, or anti-arrhythmic agents were excluded from the analysis. Nightly CPAP compliance was confirmed for patients with severe OSA. A 10-minute high-resolution Holter ECG recording was collected pre and post 4-6 weeks of CPAP, titrated during PSG, in OSA patients. In control subjects, a 10-minute Holter ECG was collected pre and post 4-6 weeks following PSG in order to gauge analysis reproducibility, with no intervention between the two recordings. Automated R-wave detection was performed using the Myoelectric Control Development Toolbox (10). HRV analysis was carried out in accordance with guidelines for standardization using MATLAB (2010a, The MathWorks, Nantick, MA) (11). Written, informed consent was obtained from every patient in accordance with a protocol approved by the Queen’s University Health Sciences Ethics Committee.
Statistical analysis
All results are expressed as mean ± standard deviation. The power of each frequency band is reported in log-normalized ms2. The very-low frequency (VLF) and ultra-low frequency (ULF) power-spectral components are absent due to their measurement not being appropriate in the relatively short-term recordings used in our analysis. In order to compare patient groups before and after the 4-6 week follow-up period, results were tested for normality using one-sample Kolmogorov-Smirnov tests, and, depending on the outcome, were then subjected either to unpaired t-tests or Wilcoxon rank sum tests with a minimum significant probability value of P<0.05. All statistical analysis was performed using MATLAB (2010a, The MathWorks, Nantick, MA).
Results
Patients with severe OSA (n=20 patients) and control subjects (n=10 patients) were included in the analysis. In patients with severe OSA, the AHI was reduced by CPAP from 38.0 ± 11.0 to 23.0 ± 11.0 episodes/hour; P<0.01. Aside from a significant difference in BMI between OSA patients and patients with AHI<5 (35.3 ± 4.7 vs. 26.6 ± 4.6 kg/m2; P<0.01), groups were comparable in age, gender, hypertension, and smoking (table 1). There was no significant difference in any HRV parameters between patients with severe OSA and controls, or between OSA patients before and after CPAP (table 2).
Discussion
Our results contrast many of those presented in the literature. Investigators have reported that over 24 hours, patients with OSA have greater sympathetic (12,13) and lesser parasympathetic influence (14) on heart rate than control subjects, as well less time-domain HRV (15). CPAP has been shown to reduce blood pressure, as well as sympathetic influence on heart rate, over 24 hours (9,16). In addition, Babaeizadeh and colleagues have described a method for detecting and quantifying apneic episodes by measuring changes in HRV over time (17). There are a number of factors that we suspect may have contributed to our unexpected results.
Our study is limited by a relatively modest sample size, with only 20 patients with severe OSA and 10 control subjects. It is conceivable that we may observe a trend in HRV over time with further enrolment. In addition, control subjects were similar to patients with severe OSA in demographic indices, apart from a difference in BMI and AHI. It may be the case that both these groups exhibit attenuated HRV compared with healthy control subjects who have not been referred for PSG. Other factors may also have played a role, such as the duration of the 4-6 week follow-up period. Perhaps if this was extended, a significant improvement in HRV indices may have taken place, possibly due to reverse autonomic remodeling. It may also be the case that changes in HRV are more pronounced during sleep, with levels returning to baseline during the day when our ECG recordings were collected for analysis. Other investigators have observed a significant improvement over a comparable follow-up during morning wakefulness, however (18). Finally, and perhaps most importantly, we employed a practical 10-minute ECG recording during clinic follow up, as opposed to the 24-hour recording more commonly reported in the literature. It has been reported that HRV results are dependent on the length of the ECG recording analyzed (11). However, it is nonetheless intriguing that short-term HRV measured during routine follow-up is not improved by CPAP in patients with severe OSA.
Conclusion
In a population referred to a sleep disorder clinic, patients with severe OSA exhibited similar heart rate variability to control subjects with normal AHI during the day. In patients with severe OSA, an improvement in AHI via 4-6 weeks of CPAP therapy was not associated with an improvement in HRV indices.
Figure 1. Results of time-domain HRV analysis. Results are listed as mean ± standard deviation.
Figure 2. Results of frequency-domain HRV analysis. Results are listed as mean ± standard deviation. ]]>Acknowledgements
Financial support to the first author from the Queen’s University Faculty of Arts and Science is gratefully acknowledged.
Bibliography
1. Young T, Peppard P, Gottlieb D. Epidemiology of obstructive sleep apnea. Am J Respir Crit Care Med 2002; 165: 1217-39.
2. Worsnop C, Naughton M, Barter C, Morgan T, Anderson A, Pierce R. The prevalence of obstructive sleep apnea in hypertensives. Am J Respir Crit Care Med 1998; 157: 111-5
3. Baranchuk A. Sleep apnea, cardiac arrhythmias and conduction disorders. J Electrocardiol. In press 2012
4. Wessendorf T, Teschler H, Wang Y, Konietzko N, Thilmann A. Sleep-disordered breathing among patients with first-ever stroke. J Neurol 2000; 247: 41-7.
5. Sin D, Fitzgerald F, Parker J, Newton G, Floras J. Risk factors for central and obstructive sleep apnea in 450 men and women with congestive heart failure. Am J Respir Crit Care Med 1999;160: 1101-6.
6. Johns M. Daytime sleepiness, snoring, and obstructive sleep apnea. the epworth sleepiness scale. Chest 1993; 103: 30-6.
7. Morrell M, McRobbie D, Quest R, Cummin A, Ghiassi R, Corfield D. Changes in brain morphology associated with obstructive sleep apnea. Sleep Med 2003; 4:4 51-4.
8. Tasali E, Mokhlesi B, Van Cauter E. Obstructive sleep apnea and type 2 diabetes: Interacting epidemics. Chest 2008; 133: 496-506.
9. Somers V, Dyken M, Clary M, Abboud F. Sympathetic neural mechanisms in obstructive sleep apnea. J Clin Invest 1995; 96: 1897-904.
10. Chan ADC, Green GC. Myoelectric control development toolbox. 30th Conference of the Canadian Medical and Biological Engineering Society. Toronto: CMBES; 2007.
11. Task force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Heart rate variability: standards of measurement, physiological interpretation, and clinical use. Circulation 1996;93: 1043-65.
12. Mansfield D, Kaye D, La Rocca H, Solin P, Esler M, Naughton M. Raised sympathetic nerve activity in heart failure and central sleep apnea is due to heart failure severity. Circulation 2003;107: 1396-400.
13. Shimizu T, Takahashi Y, Kogawa S, Takahashi K, Kanbayashi T, Saito Y, et al. Muscle sympathetic nerve activity during apneic episodes in patients with obstructive sleep apnea syndrome. Electroencephalogr Clin Neurophysiol. 1994;93:345-52.
14. Jo J, Blasi A, Valladares E, Juarez R, Baydur A, Khoo M. Model-based assessment of autonomic control in obstructive sleep apnea syndrome during sleep. Am J Respir Crit Care Med 2003; 167: 128-36.
15. Narkiewicz K, Somers V. Sympathetic nerve activity in obstructive sleep apnoea. Acta Physiol Scand 2003; 177: 385-90.
16. Roche F, Court-Fortune I, Pichot V, Duverney D, Costes F, Emonot A, et al. Reduced cardiac sympathetic autonomic tone after long-term nasal continuous positive airway pressure in obstructive sleep apnea syndrome. Clin Physiol 1999; 19: 127-34.
17. Babaeizadeh S, White D, Pittman S, Zhou S. Automatic detection and quantification of sleep apnea using heart rate variability. J Electrocardiol 2010; 43: 535-41.
18. Gilman M, Floras J, Kengo U, Yasuyuki K, Leung R, Bradley T. Continuous positive airway pressure increases heart rate variability in heart failure patients with obstructive sleep apnoea. Clin Sci (Lond) 2008; 114: 243-9.
Perfil autonómico de los pacientes derivados a una clínica de trastornos
del sueño: impacto de la CPAP
en el sistema nervioso autónomo
Geoffrey EJ Seaborn, Helen Pang, Selim G Akl, Damian P Redfearn,
Christopher S Simpson, Michael Fitzpatrick, Peter W Munt, Adrián Baranchuk
Introducción
Se estima que uno de cada cinco adultos tiene por lo menos una apnea del sueño obstructiva (AOS) leve (1), una afección que se acompaña de hipertensión (2), arritmia cardíaca (3), accidente cerebrovascular (4), insuficiencia cardíaca congestiva (5), somnolencia diurna (6), morfología encefálica anormal (7), diabetes mellitus (8), y disfunción autonómica (9). La presión positiva continua en la vía aérea (CPAP) es el tratamiento estándar para la AOS. El análisis de la variabilidad de la frecuencia cardíaca (VFC) es una técnica no invasiva y cuantitativa para la evaluación de la actividad autonómica. Nuestra hipótesis fue que los pacientes con AOS severa pueden presentar mayores niveles de disfunción autonómica que los pacientes con un índice de apnea-hipopnea (IAH) normal, y que la CPAP puede mejorar los parámetros de VFC a la vez que mejora el IAH.
Todos los pacientes fueron sometidos a una polisomnografía (PSG) en una clínica de trastornos del sueño. La AOS severa fue definida como aquella que tuviera un IAH ³ 30 (eventos por hora). El control fue definido como aquel que presentara un IAH < 5. No se incluyó en el análisis a los pacientes portadores de diabetes mellitus (DM), dispositivos implantables, anomalías cardíacas, o que estuvieran recibiendo medicación betabloqueante, bloqueantes del calcio o agentes antiarrítmicos. Para los pacientes con AOS severa se confirmó el cumplimiento nocturno de CPAP. En los pacientes con AOS se registró un trazado de ECG Holter de alta resolución de 10 minutos de duración antes y después de las 4-6 semanas de CPAP, titulándose durante la PSG. En los sujetos control se recogió un ECG Holter de 10 minutos antes y después de las 4-6 semanas luego de PSG, para medir la reproducibilidad del análisis sin que mediara ninguna intervención entre los dos trazados. Se realizó la detección automatizada de la onda R utilizando la batería de desarrollo de control mioeléctrico (10). El análisis de la VFC se realizó siguiendo las directrices para normalización, utilizando MATLAB (2010a, The MathWorks, Nantick, MA) (11). Se obtuvo consentimiento informado escrito de todos los pacientes, conforme el protocolo aprobado por el Comité de Ética de las Ciencias de la Salud de la Universidad de Queen’s.
Análisis estadísticos
Todos los resultados están expresados como media ± desviación estándar. El poder de cada banda de frecuencia se informa en ms2 normalizados logarítmicamente. Faltan los componentes del espectro de potencia de frecuencia muy baja (FMB) y frecuencia ultra baja (FUB) debido a que su medición no es apropiada en los registros de los plazos relativamente cortos utilizados en nuestro análisis. Para comparar los grupos de pacientes antes y después del período de seguimiento de 4-6 semanas, se confirmó la anormalidad de los resultados utilizando pruebas de Kolmogorov-Smirnov de una muestra, y, según fuera el resultado, luego se los sometió, ya sea a pruebas de suma de los rangos de Wilcoxon o a pruebas no apareadas con un valor de probabilidad significativo mínimo de p<0,05. Todos los análisis estadísticos se realizaron utilizando MATLAB (2010a, The MathWorks, Nantick, MA).
Resultados
En el análisis se incluyeron pacientes con AOS severa (n=20 pacientes) y sujetos control (n=10 pacientes). En pacientes con AOS severa, al utilizar CPAP, se redujo el IAH desde 38,0 ± 11,0 a 23,0 ± 11,0 episodios/hora; p<0,01. Aparte de la diferencia significativa en el IMC entre los pacientes con AOS y los pacientes con IAH<5 (35,3 ± 4,7 versus 26,6 ± 4,6 kg/m2; p<0,01), los grupos fueron comparables en cuanto a edad, género, hipertensión y tabaquismo (tabla 1). No hubo diferencia significativa en ninguno de los parámetros de la VFC entre los pacientes con AOS severa y los controles, o entre los pacientes con AOS antes y después de CPAP (tabla 2).
Discusión
]]> Nuestros resultados contrastan muchos de los resultados presentados en la literatura. Otros investigadores han comunicado que en el transcurso de 24 horas, la frecuencia cardíaca de los pacientes con AOS tiene una mayor influencia simpática (12,13) y una menor influencia parasimpática (14) que la de los sujetos control, así como menos dominio VFC-tiempo (15). Se ha demostrado que CPAP reduce la presión arterial, así como su influencia simpática sobre la frecuencia cardíaca en el transcurso de 24 horas (9,16). Además, Babaeizadeh y colaboradores han descrito un método para detectar y cuantificar episodios apneicos midiendo cambios en la VFC con el tiempo (17). Hay una serie de factores que sospechamos puedan haber contribuido a nuestros resultados inesperados.Nuestro estudio se ve acotado por un tamaño de muestra relativamente modesto: solo 20 pacientes con AOS severa y 10 sujetos control. Es concebible que si siguiéramos registrando pacientes en la evaluación, observaríamos una tendencia en la VFC con el tiempo. Además, los sujetos control fueron similares a los pacientes con AOS severa en lo que respecta a sus índices demográficos, aparte de su diferencia en IMC y en el IAH. Es posible que ambos grupos presenten una VFC atenuada comparado con sujetos-control sanos que no han sido derivados para PSG. También es posible que hayan incidido otros factores, tales como la duración del período de seguimiento de 4-6 semanas. Tal vez si esto se extendiera podría observarse una mejoría significativa de los índices de VFC, posiblemente debido a una remodelación autonómica inversa. También puede ser que los cambios de la VFC sean más pronunciados durante el sueño, retornando los niveles al nivel basal durante el día, que es cuando se recogieron nuestros registros de ECG utilizados en el análisis. (18) Sin embargo, otros investigadores han observado una mejoría significativa en un seguimiento comparable durante la vigilia matutina. Finalmente, y tal vez lo que es más importante, es que empleamos un trazado de ECG durante solo 10 minutos, en vez del registro de 24 horas utilizado más comúnmente en la literatura. Está descrito que los resultados de la VFC dependen de la duración del trazado de ECG analizado (11). Sin embargo, no deja de ser intrigante que en pacientes con AOS severa, la VFC de corto plazo medida durante un seguimiento de rutina no mejore con CPAP.
Conclusión
En una población derivada a una clínica de trastornos del sueño los pacientes con AOS severa presentaron una variabilidad de la frecuencia cardíaca similar a la de los sujetos control con un IAH normal durante el día. En pacientes con AOS severa, la mejoría del IAH con CPAP por 4-6 semanas de duración, no se acompañó de una mejoría de los índices de VFC.
Agradecimientos
Queremos agradecer el apoyo financiero que recibió el primer autor por parte de Queen’s University Faculty of Arts and Science.
]]>