Services on Demand
Journal
Article
Related links
Share
Enfermería: Cuidados Humanizados
Print version ISSN 1688-8375On-line version ISSN 2393-6606
Enfermería (Montevideo) vol.7 no.2 Montevideo Dec. 2018
https://doi.org/10.22235/ech.v7i2.1652
Artículos originales
Consumption of medicines in health professionals and technical/ administrative staff:prescription situation
1Universidad de La Frontera. Temuco, Chile. edith.rivas@ufrontera.cl
2Universidad Autónoma de Chile. Temuco, Chile.
3CIGES. Departamento de Salud Pública. Universidad de La Frontera. Temuco, Chile.
It is concluded that there is a high prevalence of self-medication and that the associated factors (smoking and alcohol consumption) influence this practice. It is hoped that the investigation into the health status of health professionals will be promoted, thus guaranteeing the safety of their activities and the impeccability in the practice of the profession.
Keywords: Nonprescription Medications; Health Technicians; Self-Medication; Risk Group.
Se espera que se fomente la indagación en la salud del personal sanitario, garantizando la seguridad de las actividades y la impecabilidad en el ejercicio técnico profesional.
Palabras Clave: Medicamentos sin prescripción; Técnicos en Salud; Automedicación; Grupo de riesgo.
Elevada percentagem de auto-medicação, semelhante a um farmacêutico de estudo e estudantes de Ciências da Saúde (38,5%) de dados. Além disso, elevado risco associado, variáveis consistentes com estudos internacionais indicando factores exógenos associados e factores endógenos. Concluiu-se que uma elevada prevalência de auto-medicação e factores associados (consumo de tabaco e álcool), afectar esta prática. O inquérito está prevista para ser promovido a saúde dos trabalhadores de saúde, garantindo a segurança das atividades e impecabilidade em exercício técnico profissional.
Palavras-chave: Medicamentos de Balcão; Técnica de Saúde; Automedicação; Grupo de Risco.
Introduction
The study problem is framed in terms of the increased knowledge of and easier access to drugs by health care professionals, technicians and administrative staff, so that in the event of a medical condition or disease, they do not consult with a medical professional, and take drugs without a prescription instead.
This attitude may be due to the recurrence of drug indication patterns made previously by the professional and then, once the treatment is finished, the remaining drugs are at their disposal. This way, when these ailments or conditions are repeated, they resort to these drugs without the accompanying consultation. There is also access to medical samples or laboratories or medical company representatives. In their daily work, relationships of trust and direct contact are established with the medical professional, who facilitates, on the one hand, greater knowledge of pathologies and medicines; on the other hand, samples or drugs can be obtained directly from this professional.
Although there is a theoretical basis about drugs, they are not free of health risks, which added to an excessive reliance on the knowledge they possess, can cause collateral health damage.
The World Health Organization (WHO) proposes guidelines that point to a better systematic strategy of communication and sensitization for all health care personnel 1. From the legislative point of view, the unregulated sale of some drugs such as analgesics is a constant that facilitates the consumption of non-prescription drugs. In this scenario, the drug policy must ensure their quality, promoting their rational use 2, being part of the national health agenda 3. For this reason, it is important to align actions to broader public health objectives, a process that can be aided by ministerial policy-making (4-5.
Against this background, drug consumption without medical indication, the arbitrary modification of dose, frequency, and time of administration is a public health problem particularly in developed countries and, specifically, the use of drugs like benzodiazepines 6. As a result, some nations have determined that pharmacists should be the ones to safeguard their appropriate use and identify people at risk of drug abuse 7.
Chile is not free of the situation described; hence, this study examines the use of drugs without a medical prescription among health care professionals and technicians/administrative staff, a context that is approached from a social and epidemiological perspective, based on the magnitude and risks for both the professional and technician, and the service of the users.
Non-prescription drug use by the medical professional is a subject of increasing relevance that merits review of the measures and safeguards for their control and supervision 8. Although this practice seems inevitable, the authorities and health care professionals must educate the public about the risks and seek strategies to increase safe and efficient use through interventions aimed at the health care team, pharmacies and consumers 4, raising awareness so as to avoid making use of this personal practice.
One efficient strategy has been the implementation of Clinical Guidelines to promote the consumption and suitable use of drugs as a central element in the education of professionals 9-10, which is not without disadvantages, such as the monitoring of prescription practices in health care institutions. In this respect, to achieve safe and suitable use of drugs, thought should be given to a law requiring a prescription for their sale, with the exception of narcotics and antibiotics, which are currently regulated and controlled. Omission has given rise to a daily practice of non-prescription drug use estimated to be between 43% and 55% 11. In addition, the decision to take medications must be accompanied by pertinent information, as occurs in developed countries and some nations in Latin America 12, where counseling is provided. However, there is limited investment to improve consumer knowledge and access to information about health and medications 13.
In a study on the magnitude and factors of non-prescription drug use conducted among doctors, pharmacists and health care students, 38.5% undertook this practice and the drugs were obtained in pharmacies or stores. The most frequently used included paracetamol and non-steroidal anti-inflammatories (NSAIDs). Previous experience and the disease not being serious were both main factors reported for their use 14.
A study of pharmacy students shows that 66.0% had medications in their room, 37.1% had leftover medication from previous indications such as analgesics, and only 25.8% obtained drugs with a prescription. The practice of taking non-prescription drugs was 53.2%, with no significant association with medical knowledge 14. Consistent with the above, in university students of nursing, the prevalence of that practice was 38.8%, the main reason being self-referred pain with moderate intensity, predominantly chronic and located in the head 15.
The sale of analgesics is widespread all over the world, because pain is one of the main reasons for consumption 1 and, simultaneously, it is based on drugs with no restrictions on their sale. Their availability for sale is a difficulty in the health sector 1. This situation facilitates the express treatment for self-diagnosed disorders or symptoms, which involves intermittent or continuous use of a non-prescription drug 2, increasing the risks of related complications because their indirect effect can vary widely and their excessive consumption could be detrimental 1. Health care professionals play an important role in promoting suitable use of prescribed medication and must actively endeavor to prevent the abuse of over-the-counter medications as well as their own consumption of non-prescription drugs 16.
The aim was to determine non-prescription drug use by health care professionals, technicians/administrative staff and associated factors in order to contribute to the evidence of a local public health situation, which leads to situations of policy improvements in the area.
Methodology
This is a cross-sectional study within the positivist paradigm in a hospital of high complexity in 2016. Deliberate probability sampling was used, from a total of 1254 non-medical professionals and technicians/administrative staff, who agreed to participate in the study; 760 signed the Informed Consent form (182 non-medical professionals and 578 technicians/administrative staff). Data collection was done using the questionnaire, “Self-medication among nursing workers from public hospitals” by Rocha A, Harter R, Rotenberg, L. 17, adapted for this study. A descriptive and association analysis was conducted between the socio-demographic, work and clinical variables and non-prescription drug use. The level of significance was 5%. The STATA 11.0 program was used. Approval was granted by the Ethics Committee of the Araucanía Sur Health Service.
Results
Of the 760 people who agreed to participate in the study, 24% were non-medical professionals; the average age was 36.5±12.0 years, with a range from 18 to 70 years. 23.2% were men, 19.6% Mapuche, 60.3% single, 6.7% urban, 34.2% with economic problems, 57.4% working shifts, 60.8% doing extra shifts, 32.9% with smoking habits, 35.9% with alcohol habits, and 93.3% who were satisfied with their work. Of the clinical variables, 9% had high blood pressure, 5.8% diabetes mellitus, 46.2% previous hospitalizations, 37.2% no presence of medical conditions, and 88.9% no presence of psychiatric disorders. 67.2% declared their monthly income to be below $500,000 pesos, 19.8% between $500,000 and $900,000 pesos and 13% over $900,000 pesos. Intake of non-prescription drugs was 44.9%.
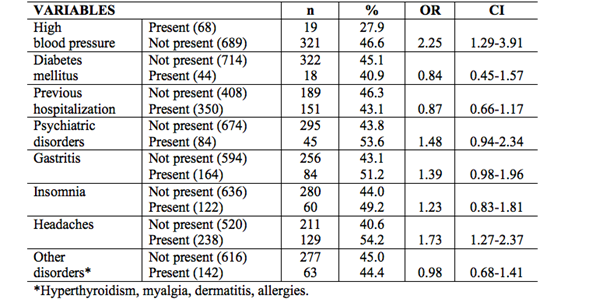
When non-prescription drug use was compared with the socio-demographic variables, there were no significant differences with: professional situation, where the non-medical professionals are 1.66 times more likely to take them; tobacco consumption, where those who smoke are 1.38 times more likely to take them; or alcohol consumption, where those who drink are 2.10 times more likely to take them. There are no significant differences with sex, ethnic group, marital status, residence, monthly income or economic problems (Table I). There was no significant association with the work variables: shift work, doing extra shifts, job satisfaction and their performance rating (Table II). No significant differences were found with the clinical variables: high blood pressure, where those who do not have hypertension are 2.25 times more likely to take them; clinical condition, where those who have some medical condition are 1.74 times more likely to take them; headaches, where those who have headaches are 1.73 times more likely to take them. There are no significant differences with diabetes mellitus, previous hospitalization, psychiatric disorders, gastritis, insomnia or other disorders (Table III).
Discussion
In our study 23.2% of the men take non-prescription drugs, studies on pharmacists and health sciences students report 38.5% self-medication 18) and the most frequently used drugs are paracetamol and NSAIDs. Previous experience and the disease not being serious were the factors reported for self-medication 18. Another study described self-medication in 53.2%, with no significant relation between having medical knowledge and self-medication 14. In our study non-prescription drug use was associated with professional situation, tobacco consumption, alcohol, hypertension and headaches.
In this respect, cognitive-social variables explain why a person adopts or rejects a particular behavior to the benefit or detriment of their own health 19, which could explain for example what is observed in pneumologists who smoke.
In this scenario, one study reports that the factors associated with self-medication in technical and nursing personnel are 88.89% exogenous and 47.22% endogenous. As an exogenous factor, unrestricted sale is indicated with 80.56% and advertising media 38.89%. Among the endogenous factors, time is mentioned at 88.89% 20.
In our study, the risk factors observed are job satisfaction, shift work or doing extra shifts, marital status, residence, monthly income and economic problems, results similar to those obtained by Llanos et al. 21.
The results obtained show the local reality, and it is recommended that strategies be sought that work towards reduction to enable a physical-mental health balance. It is hoped that this study will encourage research into the aspects of health care personnel's own health, guaranteeing the safety of the activities and achieving the highest standard in professional technical work. Important challenges persist in the consumption of medications, including the use of monitoring and assessment systems. Professionals who have an unhealthy lifestyle are an additional problem for the health of users and health care organizations.
Conclusions
It is concluded that there is a high prevalence of self-medication and that the associated factors (tobacco and alcohol consumption) affect this practice. It is hoped that health research of health personnel will be encouraged, guaranteeing the safety of activities and impeccability in the professional technical exercise.
It is suggested to continue developing research, regarding the consumption of medications, given the value of the content, the importance and relevance of this, which impacts the patient on its long-term prognosis. Situation that makes undoubted the early detection and coordination of the members of the health team
Effective management strategies must be developed in order to guarantee quality care. Research is needed to measure the effects related to drug use and its long-term impact.
ACKNOWLEDGEMENTS
To the Research Office of the Universidad de La Frontera, Chile for financing DIUFRO project 12-0039.
REFERENCES
1. World Health Organization. Everybody’s business: Strengthening health systems to improve health outcomes. WHO’s framework for action. Geneva, WHO. [ Links ]
2. Organización Mundial de la Salud. Cómo desarrollar y aplicar una política farmacéutica nacional. 2da edición. Ginebra, Suiza: OMS, 2002. [ Links ]
3. Fundación Mexicana para la Salud, A.C. trabajando por la salud de la población: Propuestas de política para el sector farmacéutico. Versión para el diálogo. México, DF: Funsalud, 2011. Disponible en: http://funsalud.org.mx/portal/wp-content/uploads/2013/08/Doc-PolPublSFarm-vFDigital-060511.pdf [ Links ]
4. Wirtz,V., Dreser, A. & Heredia-Pi, Il.x Retos y oportunidades para el desarrollo de la política farmacéutica nacional en México. Salud Púb Mex 2013; 55(3):329-336. consultado 2016 noviembre 4. Disponible en: Disponible en: http://www.saludyfarmacos.org/boletin-farmacos/ [ Links ]
5. Organización Panamericana de Salud Pública. Políticas Farmacéuticas Nacionales y Subregionales. 2011 (sitio en Internet). Washington: OPS consultado 2016 noviembre 4. Disponible en: Disponible en: http://new.paho.org/hq/index.php?option=com_content&task=view&id=1903&Itemid=1177 [ Links ]
6. López A, Aroche A, Bestard J & Ocaña N. Uso y abuso de las benzodiacepinas. 2010. Disponible en: http://bvs.sld.cu/revistas/san/vol_14_4_10/san17410.htm [ Links ]
7. BOE. BOLETÍN OFICIAL DEL ESTADO. 2012. (consultado 2016 noviembre 4). Disponible en: Disponible en: https://www.boe.es/boe/dias/2012/12/29/pdfs/BOE-A-2012-15711.pdf [ Links ]
8. Ministerio de Economía de Chile, Proyecto de Ley Venta de medicamentos fuera de Farmacias, publicado el 21 de marzo de 2012. (consultado 2016 noviembre 4). Disponible en: Disponible en: http://www.economia.gob.cl/proyecto-de-ley-mejor-acceso-a-medicamentos/ [ Links ]
9. Organización Mundial de la Salud. Cómo desarrollar y aplicar una política farmacéutica nacional . 2da edición. Ginebra, Suiza: OMS, 2002. [ Links ]
10. Laing R, Hogerzeil H & Ross-Degnan D. Ten recommendations to improve use of medicines in developing countries. Health Policy Plan 2001; 16(1):13-20. (consultado 2016 noviembre 4). Disponible en: Disponible en: http://www.ncbi.nlm.nih.gov/pubmed/11238425 [ Links ]
11. Wirtz V, Reich M, Leyva R & Dreser A. Medicines in México, 1990-2004: a systematic review of research on access and use. Salud Pub Mex 2008; 50:S470-S479. [ Links ]
12. ANMAT. Prospectos: advertencia por incumplimiento de normativas vigentes . Buenos Aires. ANMAT, 2008.(2016 noviembre 4) Disponible en: Disponible en: http://www.anmat.gov.ar/webanmat/Comunicados/Comunicado_Prospecto_IncumplimientoNormativas.pdf [ Links ]
13. González P & Barraza-Lloréns M. Trabajando por la salud de la población: Propuestas de política para el sector farmacéutico. Versión para el diálogo. México, DF: Funsalud, 2011. [ Links ]
14. Auta A; Banwat S, , Medicines in Pharmacy Students' Residence and Self-medication Practices. 2012; 4(2):119-23. (consultado 2016 noviembre 4) Disponible en: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3385216/ [ Links ]
15. Ferreira L; Damázio da Silva C; Carvalho G; Faleiros F; Varanda L. Prevalencia y caracterización de la práctica de automedicación para alivio del dolor entre estudiantes universitarios de enfermería Rev. Latino-Am. Enfermagem. 2011; 19 (2) (consultado 2016 noviembre 4) Disponible en: Disponible en: https://www.revista-portalesmedicos.com/revista-medica/automedicacion-riesgo-para-la-salud/3/ [ Links ]
16. Yakugaku, T.. Pharmacist As Gatekeeper Of Prescription Drug Abuse: Return To "Community Scientists" 2016; 136 (1): 79-87. (consultado 2016 noviembre 4) Disponible en: Disponible en: https://www.jstage.jst.go.jp/article/yakushi/136/1/136_15-00228-3/_article [ Links ]
17. Rocha R, Harter A Rotenberg R. Automedicação entre os trabalhadores de enfermagem de hospitais públicos. Rev. Latinoam. Enfermagem. 2009; 17(6). Universidade São Paulo. São Paulo, Brasil. (consultado 2016 septiembre 30). Disponible en: Disponible en: http://redalyc.uaemex.mx/src/inicio/ArtPdfRed.jsp?iCve=281421912014 [ Links ]
18. Abay S & Amelo W. Assessment of self-medication practices among medical, pharmacy, and health science students in gondar university, ethiopia. J Young Pharm. 2010; 2(3):306-10. (consultado 2016 noviembre 4) Disponible en: Disponible en: http://www.ncbi.nlm.nih.gov/pubmed/17565044 [ Links ]
19. Conner M. The role of social cognition in health behaviours en: Conner M., Norman P., editors. Predicting Health Behaviour: Research Practice with Social Cognition Models. 1993. (consultado 2016 septiembre 30). Disponible en: Disponible en: http://onlinelibrary.wiley.com/doi/10.1111/j.15591816.1998.tb01685.x/abstract;jsessionid=8741CC654617A0425E1C207AD8836C79.f02t04?deniedAccessCustomisedMessage=&userIsAuthenticated=false [ Links ]
20. Higa S. Los factores asociados a automedicación en personal técnico de enfermería en los servicios de medicina. 2015 (consultado 2016 septiembre 30). Disponible en: Disponible en: http://cybertesis.unmsm.edu.pe/handle/cybertesis/4764 [ Links ]
21. Llanos Zavalaga, L et al. Automedicación en cinco provincias de Cajamarca. Rev Med Hered 2001; 12: 127-133. (consultado 2016 noviembre20). Disponible en: Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_arttext&pid=S1018130X2001000400004&lng=es&nrm=iso [ Links ]
ANNEXESTable I Table II Table III
Table I; Table II; Table III
Table I: Drug use in health care professionals, technicians/administrative staff according to socio-demographic variables. High-complexity hospital in 2016.
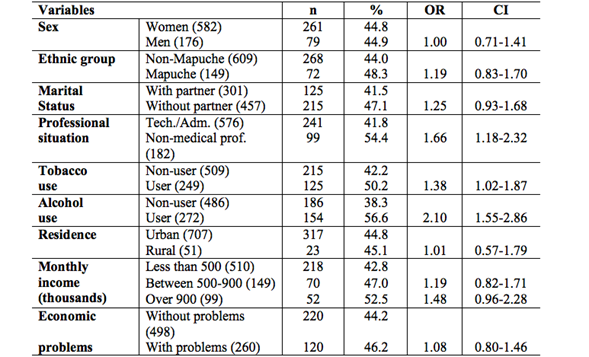
Source: Personal Collection (2016).
Table II: Drug use in health care professionals, technicians/administrative staff according to work variables. High-complexity hospital, Chile 2016.
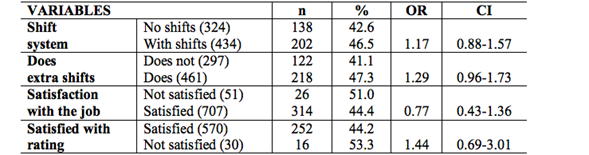
Source: Personal Collection (2016).
Received: July 13, 2017; Accepted: April 22, 2018











 text in
text in