Servicios Personalizados
Revista
Articulo
Links relacionados
Compartir
Odontoestomatología
versión impresa ISSN 0797-0374versión On-line ISSN 1688-9339
Odontoestomatología vol.23 no.37 Montevideo 2021 Epub 30-Abr-2021
https://doi.org/10.22592/ode2021n37a8
Case Report
Results of mixed and immediate bleaching techniques for bleaching endodontically treated teeth - case reports
1 Hospital de Reabilitação de Anomalias Craniofaciais da Universidade de São Paulo, (HRAC/USP), Bauru, SP, Brasil. lidianep@usp.br
2 Departamento Ciências Biológicas, Faculdade de Odontologia de Bauru, Universidade de São Paulo (FOB/USP), Brasil
Introduction:
The darkening of a single anterior tooth negatively affects the smile's appearance, and several factors may cause this darkening.
Objective:
To describe the mixed and immediate bleaching techniques by reporting two clinical cases.
Case 1:
A male individual with Treacher Collins Syndrome. He complained of chromatic alteration in tooth 33, which was verified on clinical examination. X-ray imaging showed satisfactory endodontic treatment. Internal bleaching was performed with the mixed technique.
Case 2:
A male individual with Apert Syndrome reported chromatic alteration in tooth 22, observed on clinical examination. X-ray imaging showed unsatisfactory endodontic treatment. Endodontic retreatment was performed. Six months later, internal whitening was performed immediately.
Conclusion:
The use of mixed and immediate whitening techniques restores the smile’s harmony, the tooth’s ideal color, and patients’ self-esteem.
Keywords: Non-vital tooth; bleaching agents; endodontics
Introducción:
El oscurecimiento de un diente anterior interfiere negativamente en el aspecto de la sonrisa, y varias son las causas que pueden ser responsables por este oscurecimiento.
Objetivo:
Describir las técnicas de blanqueamiento mixto e inmediato a través del reporte de dos casos clínicos.
Caso 1:
Individuo de sexo masculino, con Síndrome de Treacher Collins, se quejó sobre alteración cromática del diente 33, verificada mediante examen clínico, radiográficamente presencia de tratamiento endodóntico satisfactorio. Por lo que fue planeado el blanqueamiento interno mediante técnica mixta.
Caso 2:
Individuo de sexo masculino, con Síndrome de Apert reportó cambio cromático en el diente 22, observado en el examen clínico, radiográficamente presentando tratamiento endodóntico insatisfactorio. Se realizó retratamiento endodóntico y a los 6 meses se realizó blanqueamiento interno mediante técnica inmediata.
Conclusión:
El blanqueamiento dental ejecutado con las técnicas mixtas e inmediatas, devuelve la armonía de la sonrisa, recuperando el color ideal y elevando la autoestima a los pacientes.
Descriptores: Diente no vital; agentes blanqueadores; endodoncia
Introdução:
O escurecimento de um dente anterior interfere negativamente na aparência do sorriso, e várias são as causas que podem ser responsáveis por esse escurecimento.
Objetivo:
Descrever as técnicas clareadoras mista e imediata através do relato de dois casos clínicos.
Caso 1:
Indivíduo do gênero masculino com Síndrome de Treacher Collins, queixou-se de alteração cromática no dente 33, constatado no exame clínico, radiograficamente apresentando tratamento endodôntico satisfatório. O clareamento interno foi planejado e realizado pela técnica mista.
Caso 2:
Indivíduo do gênero masculino, com Síndrome de Apert, relatou alteração cromática no dente 22, constatado ao exame clínico, apresentando tratamento endodôntico insatisfatório. Foi realizada a reintervenção endodôntica e após 6 meses, foi realizado clareamento interno pela técnica imediata.
Conclusão:
O uso das técnicas clareadoras mista e imediata, resulta na devolução da harmonia do sorriso, recuperando a coloração ideal e devolvendo a autoestima aos pacientes.
Descritores: Dente não vital; agentes clareadores; endodontia
Introduction
Teeth bleaching is the most conservative attempt to restore standard tooth color and has clear advantages over other procedures such as avoiding tooth structure wear. It provides proven long-term satisfactory aesthetic results and is efficient, relatively simple, and inexpensive compared to prosthetics treatment1-5. Even if it fails, more invasive additional therapies can still be performed, such as veneers or full crowns6.
Factors such as trauma, pulp stones, inadequate therapeutic techniques, and failed endodontic treatment (obturation materials such as gutta-percha cones and endodontic cement when left in the pulp chamber after endodontic treatment) can lead to chromatic changes5,7-10.
The first reports in the literature on the use of bleaching agents date back to 1860, as well as the use of various substances: calcium chloride, chlorine, aluminum chloride, oxalic acid, sulfur dioxide, sodium hypochlorite, among others1. The market offers 30% to 35% hydrogen-peroxide bleaching agents that can be used separately or with sodium perborate3,5,11.
Potential external cervical resorption is one of the main concerns regarding tooth bleaching in endodontically treated teeth10,12. Other possible undesired effects are reduction of fracture resistance and dentine microhardness on account of tooth overexposure to these substances in high concentrations and/or for prolonged periods13.
This paper presents two clinical cases describing the techniques used for tooth bleaching to address darkened endodontically treated teeth in individuals attending Hospital de Reabilitação de Anomalias Craniofaciais, University of São Paulo given patients’ aesthetic requirements.
Background
Darkened teeth break a smile’s color harmony, leading patients to seek therapies to restore natural tooth color. There are several treatments for endodontically treated teeth with chromatic change. However, tooth bleaching is presented as a first option6.
Non-vital tooth bleaching should be indicated cautiously. The following factors should be evaluated: extensive restorations or insufficient remains, enamel fracture lines, tetracycline staining, quality of endodontic treatment, periapical lesions, external and internal resorptions, cause and time of chromatic change, and degree of darkening7,9,14.
Pulp removal is a dental intervention that causes bleeding in the dentin, where blood enters the dentinal tubules and then breaks down. Discoloration may occur when the pulp tissue is not entirely removed during endodontic treatment. When sodium hypochlorite and chlorhexidine are mixed, reddish-brown precipitates are formed, which can cause chromatic change. So, it is necessary to neutralize them with physiological saline or saline solution between irrigant uses. Although highly biocompatible, white, or grey mineral trioxide aggregate (MTA) can cause undesired discoloration8.
The most commonly used bleaching agents in pulpless teeth are hydrogen peroxide, carbamide peroxide and sodium perborate associated with distilled water, saline solution or 35% hydrogen peroxide. However, using sodium perborate with distilled water or physiological serum is more effective and safer when compared to hydrogen peroxide, which is considered caustic5,15-16.
Bleaching must meet some conditions to be safe: correct, complete, and total isolation of soft tissues (gingival tissues, lips, cheeks) to protect them from possible burns17-20.
One of the main concerns regarding the bleaching of endodontically treated teeth is pH level and the high permeability of bleaching agents. When these agents reach the periodontal tissues through the dentinal tubules, they can alter the cementoenamel junction. This can trigger an inflammatory reaction caused by the denaturation of dentin. Said dentin can be considered a different tissue and thus be detected as a foreign body. This can lead to external cervical resorption1,12,14,19,21. This resorption is asymptomatic and is usually diagnosed through routine radiography or clinical examination that reveals swollen papilla and a positive response to percussion22.
Therefore, it is essential to create a barrier in the cervical region, at the cementoenamel junction, between the obturating material (gutta-percha) and the pulp chamber space. This prevents the penetration of bacteria and the extrusion of the bleaching agent towards the apical periodontium, which could cause cervical resorption. Glass ionomer cement is the most widely used material to make this barrier because it is more cost-effective, among other advantages(6,14,19.
Several tooth bleaching techniques are described in the literature. They can be classified into two groups: according to the area (internal or external) or to the time the bleaching agent remains in place (immediate, walking bleach, and mixed)(15. The main difference is the method applied by bleaching chemicals to release active oxygen. The bleaching agent is placed inside the pulp chamber in the walking bleach technique and remains there for three to seven days. It must be changed until the desired color is obtained, with a maximum of four sessions. This technique is considered the least risky regarding external cervical resorption. In the immediate technique, the bleaching agent is applied to the pulp chamber and the outer surface and left for approximately 45 minutes. Bleaching materials are potent oxidizing agents that react with the pigment compounds formed by carbon macromolecules. These molecules become compounds of lower molecular weight (carbon dioxide and water) through oxidation, and thus pigments diffuse through mineralized tissues, resulting in an oxidation bleaching action 9-10,12,19.
After achieving the desired whitening effect, calcium hydroxide medication should be applied before the final restoration for 7-14 days to alkalize the medium and wait for the residual oxygen release time. This time is necessary to promote effective sealing and avoid microfiltration, as such residues may inhibit adhesive material polymerization5,10,14-15,19.
Below we present two clinical cases, the relevant considerations, and the results obtained.
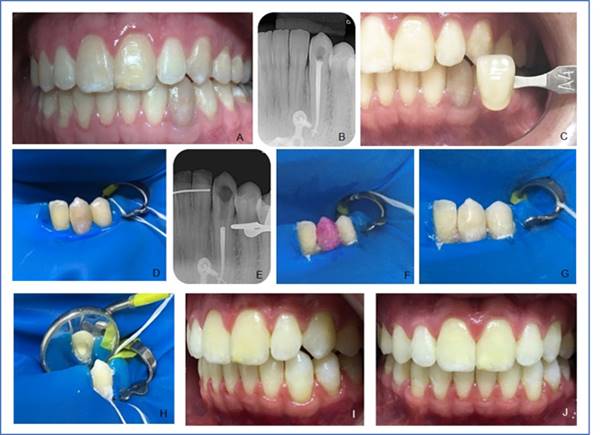
Clinical case 1 report: 23-year-old male with Treacher Collins Syndrome attending Hospital de Reabilitação de Anomalias Craniofaciais, University of São Paulo (HRAC/USP). He reports a chromatic change in the lower left canine (33) (Fig. 1, A). This was verified on clinical examination, as well as absence of painful symptoms. Satisfactory endodontic treatment was observed on radiographic examination (Fig. 1, B). Internal bleaching was performed with the mixed technique. The color (A4) was selected using the VITA scale (Wilcos do Brasil, Petrópolis RJ, Brazil). There followed an intraoral photo (Fig. 1, C), absolute isolation (Fig. 1, D), followed by access to the pulp chamber using diamond bur No. 1012 (KG Sorensen Ind. Com. Ltda, Barueri, Brazil). Endodontic obturation was removed at approximately 3 mm deep with No. 2 condensers heated at the root canal entry, the cavity was cleaned, and the cervical barrier was prepared (Figure, E) with glass ionomer cement (FGM, Joinville, SC, Brazil). Acid etching of the pulp chamber was then performed with 37% phosphoric acid (Biodynamics, Ibiporã, PR, Brazil) for 30 seconds, then washed with plenty of water for 60 seconds and dried with an air jet. This is done to remove the smear layer, open the dentinal tubules and therefore increase the dentin's permeability to the bleaching agent. We handled 35% hydrogen peroxide gel (Whiteness HP, FGM, Joinville, SC, Brazil) following the manufacturer’s guidelines and placed it inside the pulp chamber and on the buccal face with a medium-sized microbrush (KG Sorensen Ind. Com. Ltda, Barueri, Brazil) for 45 minutes (Fig. 1, F and G). The gel was removed by washing with water for 1 minute, and then a granular sodium perborate paste (Pharmacy Specific, Bauru, SP, Brazil) was handled with sterile saline solution in a sterile Dappen glass. The paste was placed inside the pulp chamber with an insertion spatula and evenly spread (Fig. 1, H). The tooth was sealed with glass ionomer cement (FGM, Joinville, SC, Brazil). A satisfactory result was observed after seven days (Figs. 1, I and J) when comparing the tooth to its past appearance. Calcium hydroxide paste (Calen) (SSWhite Duflex, São Cristovão, RJ, Brazil) was applied. The temporary restoration with glass ionomer cement (FGM, Joinville, SC, Brazil) was placed. The patient reported the yellowing of the other teeth and was then referred to the Aesthetic Dentistry sector of HRAC/USP for external whitening and for the final restoration.
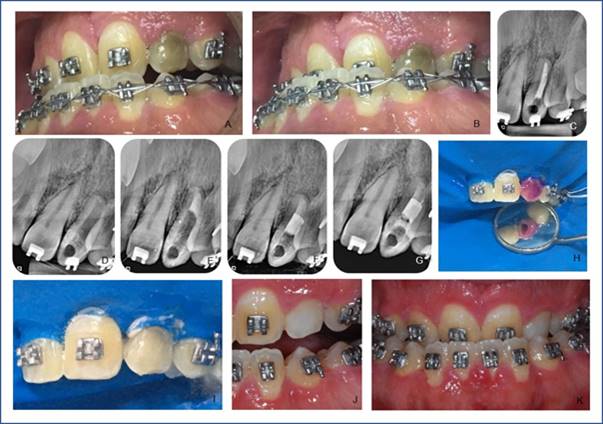
 Clinical case 2 report: 30-year-old male with Apert syndrome attending HRAC/USP. He reports chromatic change in the lower left canine (22) (Fig. 2, A and B). This was verified on clinical examination, as well as the absence of painful symptoms. Unsatisfactory endodontic treatment was observed on the radiograph (Fig. 2, C). Endodontic retreatment (Fig. 2, D, and E) was performed. It was necessary to prepare an apical barrier with MTA (Fig. 2, F) (Angelus Ind. De Productos Odontológicos S/A, Londrina, PR, Brazil). Immediate internal tooth bleaching was started six months after retreatment. The color was recorded with the intraoral photo (Fig. 2, B) because the tooth color was not identified on the VITA scale (Wilcos do Brasil, Petrópolis, RJ, Brazil) as it was darker. Absolute insulation was then placed, followed by access to the pulp chamber using diamond bur No. 1012 (KG Sorensen Ind. Com. Ltda, Barueri, Brazil), endodontic obturation removal with No. 2 condensers, root canal entry. The cavity was cleaned, and the cervical barrier was prepared with SureFil SDR flow light-curing resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil) (Fig. 2, G). Acid etching of the pulp chamber was then performed with 37% phosphoric acid (Biodynamics, Ibiporã, PR, Brazil) for 30 seconds, then removed with plenty of water for 60 seconds and dried with an air jet. We handled 35% hydrogen peroxide gel (Whiteness HP, FGM, Joinville, SC, Brazil) following the manufacturer’s instructions and placed it inside the pulp chamber and on the buccal face (Fig. 2, H and I) with a medium-sized microbrush (KG Sorensen Ind. Com. Ltda, Barueri, Brazil) with a 45-minute application. The gel was removed after washing with water for 1 minute. A second application was performed for 25 minutes and sealed with SureFil SDR flow resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil). The second session included absolute isolation, cervical barrier with Top Dam (FGM, Joinville, SC, Brazil), acid etching, washing and drying in the same way, 35% hydrogen peroxide gel (Whiteness HP, FGM, Joinville, SC, Brazil) was handled following the manufacturer’s guidelines and inserted inside the pulp chamber and on the vestibular face with a medium-sized microbrush (KG Sorensen Ind. Com. Ltda, Barueri, Brazil). The first application lasted 15 minutes. After removing the gel, the second application was performed for 15 more minutes but only externally limited to the cervical region. Satisfactory results (Fig. 2, J and K) were achieved compared to the appearance before bleaching and temporary restoration with SureFil SDR flow resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil). On his return, the patient was referred to the Aesthetic Dentistry sector, where the final restoration was performed.
Clinical case 2 report: 30-year-old male with Apert syndrome attending HRAC/USP. He reports chromatic change in the lower left canine (22) (Fig. 2, A and B). This was verified on clinical examination, as well as the absence of painful symptoms. Unsatisfactory endodontic treatment was observed on the radiograph (Fig. 2, C). Endodontic retreatment (Fig. 2, D, and E) was performed. It was necessary to prepare an apical barrier with MTA (Fig. 2, F) (Angelus Ind. De Productos Odontológicos S/A, Londrina, PR, Brazil). Immediate internal tooth bleaching was started six months after retreatment. The color was recorded with the intraoral photo (Fig. 2, B) because the tooth color was not identified on the VITA scale (Wilcos do Brasil, Petrópolis, RJ, Brazil) as it was darker. Absolute insulation was then placed, followed by access to the pulp chamber using diamond bur No. 1012 (KG Sorensen Ind. Com. Ltda, Barueri, Brazil), endodontic obturation removal with No. 2 condensers, root canal entry. The cavity was cleaned, and the cervical barrier was prepared with SureFil SDR flow light-curing resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil) (Fig. 2, G). Acid etching of the pulp chamber was then performed with 37% phosphoric acid (Biodynamics, Ibiporã, PR, Brazil) for 30 seconds, then removed with plenty of water for 60 seconds and dried with an air jet. We handled 35% hydrogen peroxide gel (Whiteness HP, FGM, Joinville, SC, Brazil) following the manufacturer’s instructions and placed it inside the pulp chamber and on the buccal face (Fig. 2, H and I) with a medium-sized microbrush (KG Sorensen Ind. Com. Ltda, Barueri, Brazil) with a 45-minute application. The gel was removed after washing with water for 1 minute. A second application was performed for 25 minutes and sealed with SureFil SDR flow resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil). The second session included absolute isolation, cervical barrier with Top Dam (FGM, Joinville, SC, Brazil), acid etching, washing and drying in the same way, 35% hydrogen peroxide gel (Whiteness HP, FGM, Joinville, SC, Brazil) was handled following the manufacturer’s guidelines and inserted inside the pulp chamber and on the vestibular face with a medium-sized microbrush (KG Sorensen Ind. Com. Ltda, Barueri, Brazil). The first application lasted 15 minutes. After removing the gel, the second application was performed for 15 more minutes but only externally limited to the cervical region. Satisfactory results (Fig. 2, J and K) were achieved compared to the appearance before bleaching and temporary restoration with SureFil SDR flow resin (Dentsply Ind. Com. Ltda, Petrópolis, RJ, Brazil). On his return, the patient was referred to the Aesthetic Dentistry sector, where the final restoration was performed.
Discussion
Aesthetic dissatisfaction appears most clearly when one or more teeth change color, leading patients to search for a treatment to restore the smile’s natural characteristics and harmony19,23. However, dental professionals must diagnose and determine the etiology of chromatic change for clinical planning, material selection, and the clinical success of the bleaching treatment24.
As several materials are often used for endodontic obturation of the pulp chamber, considerable discoloration is promoted, which intensifies in the cervical third. This is caused by cutting the obturation incorrectly, which should be done at or below the cementoenamel junction6,11. This was the leading cause of tooth darkening in the clinical cases described above.
Non-vital teeth bleaching is contraindicated in teeth with a widely restored or decayed buccal surface, tooth cracks, poor restorations, and unsatisfactory endodontic treatment. Teeth that have been intensely darkened for many years have a slight chance of restoring color successfully. In some situations, it is necessary to suggest prosthetic or restorative alternatives13. The clinical conditions in case 1 were favorable for bleaching without any endodontic intervention; in case 2, endodontic retreatment was first indicated, and then bleaching was performed.
Hydrogen peroxide (H2O2) is the primary bleaching agent used. It is a cytotoxic, thermally unstable free radical with a low molecular weight that penetrates enamel and dentin through diffusion and reaches the periodontium6-7,25. Hydrogen peroxide penetration was significantly higher in teeth with cement defects and/or a gap between the cement and the enamel at the cementoenamel junction1,14.
The use of heat (thermocatalytic technique) should be avoided to prevent external cervical resorption cases, which can be caused by internal bleaching of non-vital teeth. Additionally, proper cervical sealing is essential.
Cervical sealing consists of a mechanical barrier placed at the cementoenamel junction between the obturation material (gutta-percha) and the pulp chamber space, where the bleaching agent will be placed. Its function is to prevent bacteria penetration or the diffusion of bleaching agent molecules towards the apical periodontium via the dentinal tubules6. Given the above, we chose glass ionomer cement to prepare the cervical barrier in case 1, and SureFil SDR flow resin in case 2.
Different techniques were selected for these cases since the patient in case 1 was available and could return periodically to perform the bleaching; therefore, the mixed technique was selected. In addition to applying the bleaching gel during the endodontic session, both in the pulp chamber and externally on the buccal surface, a whitening paste was used internally in the pulp chamber and left for seven days. According to the literature, the bleaching agent should be changed or reassessed every seven days. As the patient in clinical case 2 could not return for these weekly changes, the immediate technique was applied in two consecutive sessions. This prevented the patient from returning to their home city with the bleaching agent inside the tooth.
The most commonly used bleaching agents are hydrogen peroxide, carbamide peroxide, and sodium perborate. The latter can be associated with distilled water, saline solution, or 35% hydrogen peroxide. However, using sodium perborate with distilled water or saline solution is more effective and safer when compared to hydrogen peroxide, which is highly caustic7,26. This was why sodium perborate was associated with saline solution in paste form in case 1, in which the mixed technique was performed.
The effectiveness of the bleaching paste also depends on the material used to seal the cavity. This material aims to prevent fluid infiltration into the pulp chamber, preventing dentin contamination and tooth recoloration24. The temporary material-glass ionomer cement-was placed to provide mechanical and displacement resistance due to the pressure exerted by the oxygen released by the bleaching paste (sodium perborate + saline solution). Patients were advised to be careful about the consistency of the food ingested and chewing with the bleached tooth throughout the bleaching period to avoid tooth fracture.
Fourteen days must elapse without adhesive alterations after bleaching to perform adhesive restorative procedures on the enamel. During this period, the pulp chamber must be filled with calcium hydroxide paste to neutralize the effect of bleaching agents, given the paste’s ability to permeate the dental tissues1. In the two clinical cases reported, we used Calen calcium hydroxide paste for the 14-day period and then referred the patient for the final restoration.
The duration of the bleaching treatment cannot be predicted. The longer the time and degree of tooth darkening, the more clinical sessions will be needed and the lower the likelihood of success. In addition to external resorption, which can occur up to seven years after the internal bleaching treatment, it is essential to perform clinical and X-ray evaluations23. Another limitation is maintaining the long-term outcome, as many cases might present recurring darkness caused by poor sealing between the tooth and the restoration23,15.
Conclusion
Internal bleaching of endodontically treated teeth with chromatic changes has several advantages: minimal wear of tooth surface, low cost and effectiveness in a short time. The use of mixed and immediate techniques-when correctly indicated-restores the smile’s harmony with a simple, effective, fast and satisfactory method. These techniques made it possible to restore patients’ self-esteem and provided a solution for the clinical cases presented.
REFERENCES
1. WHO. Noncommunicable diseases. Fact sheet updated Junio 2018. (en linea). consultado 30 de octubre de 2018. Disponible en: Disponible en: http://www.who.int/mediacentre/factsheets/fs355/en/ [ Links ]
2. Uruguay. Ministerio de Salud Pública. Enfermedades No Transmisibles. (en línea). consultado 30 de octubre de 2018 Disponible en:Disponible en:http://www.msp.gub.uy/noticia/enfermedades-no-transmisibles [ Links ]
3. Eke PI, Wei L, Thornton-Evans GO, Borrell LN, Borgnakke WS, Dye B, Genco RJ. Risk indicators for periodontitis in US adults: NHANES 2009 to 2012. J Periodontol 2016 Oct;87(10):1174-85 [ Links ]
4. Janket S-J, Baird AE, Chuang S-K, Jones JA. Meta-analysis of periodontal disease and risk of coronary heart disease and stroke. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003; 95(5): 559-569. [ Links ]
5. Uruguay. Ministerio de Salud Pública. Segunda Encuesta Nacional de Factores de Riesgo de Enfermedades No Transmisibles. PPENT. Montevideo, 2013. (en línea) (consultado 30 de octubre de 2018) Disponible en: Disponible en: http://www.msp.gub.uy/publicaci%C3%B3n/2%C2%AA-encuesta-nacional-de-factores-de-riesgo-de-enfermedades-no-transmisibles . [ Links ]
6. Lorenzo-Erro S, Blanco S, Álvarez R, Massa F, Fabruccini-Fager A, Olmos P, Musto M, Ourens M. Primer Relevamiento Nacional de Salud Bucal de jóvenes y adultos uruguayos 2011. Facultad de Odontología. Universidad de la República. Montevideo, marzo 2018. Disponible:https://www.colibri.udelar.edu.uy/jspui/handle/20.500.12008/18508 [ Links ]
7. Álvarez L, Liberman J, Abreu S, Mangarelli C, Correa MB, Demarco FF, Lorenzo S, Nascimento GG.-Dental caries in Uruguayan adults and elders: findings from the first Uruguayan NationalOral Health Survey. Cad Saude Publica. 2015 Aug; 31(8):1663-72. doi: 10.1590/0102-311X00132214. [ Links ]
8. Lorenzo SM, Álvarez R, Andrade E, Piccardo V, Francia A, Massa F, Correa MB, Peres MA. Periodontal conditions and associated factors among adults and the elderly: findings from the first National Oral Health Survey in Uruguay.Cad Saude Publica. 2015 Nov; 31(11):2425-36. doi: 10.1590/0102-311X00012115. [ Links ]
9. Lorenzo-Erro SL, Skapino E , Musto M, Olmos P, Álvarez R, Fabruccinni A, Massa F, Moliterno P, Piovesán S, Cosetti L, Pisón F. Salud Bucal y Enfermedades no transmisibles en pacientes de un centro de enseñanza terciaria, Montevideo, Uruguay 2016. Parte 1. Odontoestomatología. 2020; 22(36). [ Links ]
10. World Health Organization. Oral Health Surveys. Basic Methods. 5th Edition (Internet).Geneva; 2013. [ Links ]
11. Vettore MV, Marques RA, Peres MA. Social inequalities and periodontal disease: multilevel approach in SB (Brasil 2010 survey). Rev Saude Publica. 2013;47 Suppl 3:29-39 [ Links ]
12. Nicola-Laguzzi P, Silveira-Schuch H, Derrégibus-Medina L, Rodríguez-de Amores A, Demarco FF, Lorenzo S. Tooth loss in the elderly in Uruguay. J Public Health Dent 2016; 76: 143-151. doi:10.1111/jphd.12123 [ Links ]
13. Cardoso RM, Cardoso RM, Junior PCM, Filho PFM. Clareamento interno: uma alternativa para discromia de dentes tratados endodonticamente. Odontol. Clín.-Cient. (online) 2011; 10 (2). Fecha de acesso: 4 de octubre de 2019. Disponíble en: Disponíble en: http://revodonto.bvsalud.org/scielo.php?script=sci_arttext&pid=S1677-388820110002 00016 [ Links ]
14. Attin T, Paque F, Ajam F, Lennon AM. Review of the current status of tooth whitening with the walking bleach technique. Int Endod J 2003; 36: 313-329 [ Links ]
15. Júnior AOS, Mateo-Castillo JF, Neves LT, Nishiyama CK, Pinto LC. Recuperação da coloração de dentes tratados endodonticamente através das técnicas clareadoras imediata e mista. Salusvita (online) 2018; 37(1): 77-91. (fecha de acceso: 4 de octubre de 2019). Disponíble en: Disponíble en: https://secure.usc.br/static/biblioteca/salusvita/salusvita_v37_n1_2018_art_06.pdf [ Links ]
16. Sampaio MD, Freitas AP, Araujo RPC. Análise espectrofotométrica do clareamento dental interno / Spectrophotometric analysis of internal dental bleaching effect. RGO, Rev. gaúch. Odontol. (online) 2010; 58(3): 363-368. Fecha de acceso: 4 de octubre de 2019. Disponíble en: Disponíble en: http://revodonto.bvsalud.org/scielo.php?script=sci_arttext&pid=S1981-86372010000300014&lng=es&nrm=iso&tlng=pt [ Links ]
17. Moraru I, Tuculinã M, Bãtãiosu M, Gheorghitã L, Diaconu O. Whitening non vital teeth - a case report. Curr Health Sci J 2012; 38(3): 132-135 [ Links ]
18. Dahl JE, Pallesen U. Tooth bleaching-a critical review of the biological aspects. Crit Rev Oral Biol Med, 2003; 14(4):292-304. [ Links ]
19. Coelho, AS. et al. Non-Vital Tooth Bleaching Techniques: A Systematic Review. Coatings 2020, 10(1), 61; https://doi.org/10.3390/coatings10010061 [ Links ]
20. Rodrigues LM, Vansan LP, Pécora JD, Marchesan MA. Permeability of different groups of maxillary teeth after 38 percent hydrogen peroxide internal bleaching. Braz. Dent. J, 2009; 20 (4): 303-6. [ Links ]
21. Badole GP, Warhadpande MM, Bahadure RN, Badole SG. Aesthetic Rehabilitation of Discoloured Nonvital Anterior tooth with Carbamide Peroxide Bleaching: Case Series. J Clin Diagn Res. 2013; 7 (12): 3073-3076. [ Links ]
22. Nagaveni NB, Umashankara KV, Radhika NB, Satisha TS. Management of tooth discoloration in non-vital endodontically treated tooth - A report of 6 year follow-up. J Clin Exp Dent. 2011; 3(2): 180-183. [ Links ]
23. Bortolatto JF, Corsi CE, Presoto CD, Cioffi SS, Júnior OBO. Clareamento interno em dentes despolpados como alternativa a procedimentos invasivos: relato de caso. Rev. Odontol. Univ. Cid. São Paulo, São Paulo, 2012; 24 (2): 142-52. [ Links ]
24. Kasuya AVB, Favarão IN, Souza JL, Cardoso SA, Fonseca RB, Hoeppner MG. Longevidade de clareamento em dente não vital com associação de técnicas: relato de caso. Estética 2012; 9 (2): 104-113. [ Links ]
25. Fernandes AM, Marques MM, Camargo SEA, Cardoso PE, Camargo HR, Valera MC. Cytotoxicity of non-vital dental bleaching agents in human gingival fibroblasts. Braz Dent. Sci 2013; 16 (1): 59-65. [ Links ]
26. Valera MC, Camargo CH, Carvalho CA, de Oliveira LD, Camargo SE, Rodrigues CM. Effectiveness of carbamide peroxide and sodium perborate in non-vital discolored teeth. J Appl Oral Sci. (Online) 2009; 17(3):254-61. Fecha de acceso: 4 de octubre de 2019. Disponíble en: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-77572009000300024 [ Links ]
Received: February 14, 2020; Accepted: January 28, 2021











 texto en
texto en 
 Curriculum ScienTI
Curriculum ScienTI