Servicios Personalizados
Revista
Articulo
Links relacionados
Compartir
Odontoestomatología
versión impresa ISSN 0797-0374versión On-line ISSN 1688-9339
Odontoestomatología vol.22 no.35 Montevideo 2020 Epub 01-Jun-2020
https://doi.org/10.22592/ode2020n35a9
Case Report
Mucocele of Blandin Nuhn glands. Unusual case and review of the literature
1Escuela Nacional de Estudios Superiores, Unidad León, Universidad Nacional Autónoma de México, México
2Centro Mexicano de Estomatología, México
3Centro Mexicano de Estomatología, México
4Escuela Nacional de Estudios Superiores, Unidad León, Universidad Nacional Autónoma de México, México. drvillanueva.enesunam@gmail.com
The mucocele associated with the Blandin Nuhn glands is a phenomenon of mucosal extravasation that occurs in the salivary glands located in the anterior ventral surface of the tongue, are mixed type, not encapsulated, which are part of the complex of minor salivary glands of the oral cavity. Objective: The clinical case of a male patient who is in the second decade of life with peculiar clinical characteristics of a Blandin Nuhn mucocele is presented. Clinical case: A 14-year-old male adolescent presents an increase in volume located on the ventral surface of the tongue, cylindrical shape, 3 months evolution and asymptomatic. Excisional biopsy is performed for histopathological study, which reports mucosal extravasation phenomenon and histopathological clinical correlation is established. Conclusions: A correct diagnosis should be based to provide timely treatment and avoid complications in the patient that affect their quality of life.
Keywords: mucocele; minor salivary glands; tongue; treatment
El mucocele asociado a las glándulas de Blandin Nuhn es un fenómeno de extravasación mucosa que ocurre en las glándulas salivales localizadas en la superficie ventral anterior de la lengua, son de tipo mixto, no encapsuladas, que forman parte del complejo de glándulas salivales menores de cavidad bucal. Objetivo: Se presenta el caso clínico de un paciente masculino que cursa la segunda década de vida con características clínicas peculiares de un mucocele de Blandin Nuhn. Caso clínico: Adolescente masculino de 14 años de edad presenta aumento de volumen localizado en superficie ventral de lengua, forma cilíndrica, de 3 meses de evolución y asintomático. Se realiza biopsia excisional para estudio histopatológico, el cual reporta fenómeno de extravasación mucosa y se establece la correlación clínico histopatológica. Conclusiones: Se debe fundamentar un diagnóstico correcto para proporcionar un tratamiento oportuno y evitar complicaciones en el paciente que afecten su calidad de vida.
Palabras clave: mucocele; glándulas salivales menores; lengua; tratamiento
A mucocele associada às glândulas de Blandin Nuhn é um fenômeno de extravasamento de mucosa que ocorre nas glândulas salivares localizadas na superfície ventral anterior da língua, do tipo misto, não encapsuladas, que fazem parte do complexo de glândulas salivares menores da cavidade oral. Objetivo: É apresentado o caso clínico de um paciente do sexo masculino na segunda década de vida com características clínicas peculiares de uma mucocele de Blandin Nuhn. Caso clínico: Adolescente de 14 anos apresenta aumento de volume localizado na superfície ventral da língua, formato cilíndrico, evolução de 3 meses e assintomático. A biópsia excisional é realizada para estudo histopatológico, que relata o fenômeno do extravasamento da mucosa e a correlação clínica histopatológica é estabelecida. Conclusões: Um diagnóstico correto deve ser baseado para fornecer tratamento oportuno e evitar complicações no paciente que afetem sua qualidade de vida.
Palavras-chave: mucocele; glândulas salivares menores; língua; tratamento
Introduction
Mucoceles are a common lesion of the oral mucosa that occur because of a ruptured salivary gland duct and subsequent mucin leakage into the surrounding soft tissues. This leakage is often the result of local trauma, although many cases have no history of such trauma1-2.
Mucoceles are more common in children and young adults1-3, probably because they are more likely to experience trauma leading to mucin leakage; however, they have been reported in patients of all ages1.
These lesions have no sex predilection2-3 but may occur more frequently among females2.
Mucoceles originate primarily in the lower lip and less common sites such as the floor of the mouth, the anterior ventral surface face of the tongue (associated with the glands of Blandin-Nuhn), the oral mucosa, and the palate1,4-5.
The clinical presentation varies and depends on the depth at which the lesion appears and the keratosis degree of the mucosa3.
Additionally, histopathological examination shows mucin extravasation surrounded by granulation tissue with numerous foamy histiocytes, without surrounding epithelial lining1,6.
The main differential diagnoses considered when evaluating mucocele of the glands of Blandin-Nuhn are vascular lesions (hemangioma, lymphangioma), pyogenic granuloma, squamous papilloma and salivary gland tumors3,7.
In addition, there are multiple treatments for mucoceles of the glands of Blandin-Nuhn that are classified into surgical and conservative3.
Prognosis is excellent, although mucoceles sometimes recur, requiring further excision1.
This paper presents the clinical case of a mucocele associated with the glands of Blandin-Nuhn with specific clinical characteristics regarding histopathological findings and treatment.
Background
Unlike salivary duct cysts, mucoceles are not true cysts because they lack epithelial lining1. However, true salivary duct cysts have been included in reported series of mucoceles, sometimes classified as retention mucocele or mucous retention cyst1,8 because these authors considered salivary duct cysts a histopathological variant of the retention mucocele, as opposed to the mucous extravasation phenomenon of conventional mucoceles8.
Some authors classify mucoceles into two types according to their formation mechanism and histological characteristics: extravasation and retention mucocele9-11.
Furthermore, a recent study of 1715 cases of mucoceles found that 81.9% occurred in the lower lip (usually lateral to the midline) and the least common sites were the floor of mouth (ranulas: 5.8%), anterior ventral surface of the tongue (of the glands of Blandin-Nuhn: 5.0%), oral mucosa (4.8%), palate (1.3%) and retromolar area (0.5%)1.
Case description
A 14-year-old male patient, original from and resident of León Guanajuato, attended the Oral and Maxillofacial Pathology Clinic of Escuela Nacional de Estudios Superiores, Unidad León, UNAM, with his mother, as he had a localized volume increase on the ventral surface of the tongue (Fig. 1).
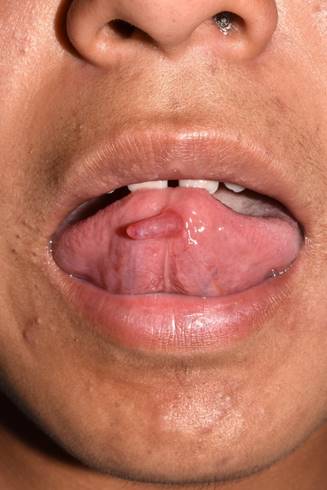
Fig. 1: Localized cylindrical increase in volume on the ventral surface of the tongue to medial on the left side, slightly more erythematous than the adjacent mucosa
In the direct interview, the patient did not report any relevant inherited family, non-pathological and pathological personal history or any history of tongue trauma.
Additionally, extraoral examination was performed and no visible alterations were found.
In the intraoral examination, the examiner found an increase in volume on the ventral surface of the tongue, pink and with erythematous areas, measuring approximately 1.5 cm, cylindrical, with a smooth surface, soft consistency, asymptomatic, of three months of evolution. The patient reported that it sometimes decreased in size (Fig. 2).
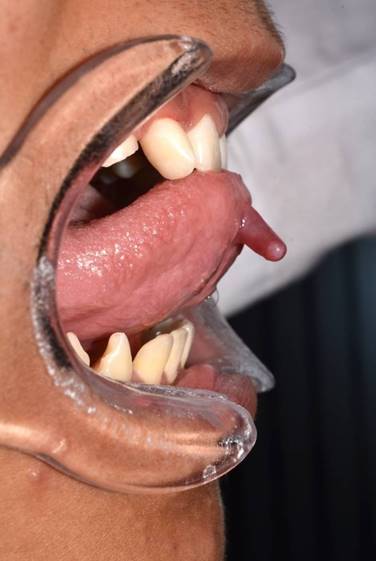
Fig. 2: Side view of cylindrical volume increase on ventral surface of the tongue, smooth surface, soft consistency, asymptomatic, with remission and exacerbation periods
The relevant informed consent was signed and the outpatient excisional biopsy was scheduled. The surgical protocol included disinfecting the surgical area with iodine povidone, sterile antisepsis, local infiltration with 1:100,000 articaine, full-thickness surgical spindle incision, hemostasis, surgical site treatment, and isolated stitches with 4-0 polyglycolic acid (Fig. 3). The specimen was then transferred for histopathological study.
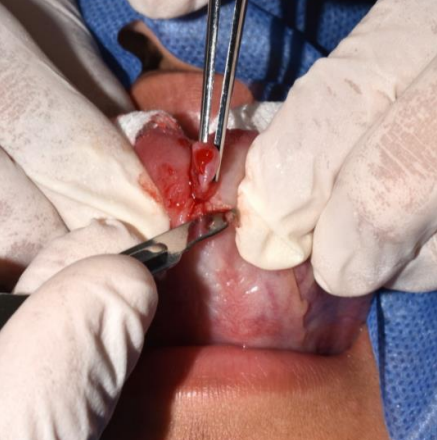
Fig. 3: Surgical excision following the established protocol, surgical spindle incision and blunt dissection approach
In the macroscopic description, a single soft tissue specimen was received from the ventral surface of the tongue, fixed with 10% formalin, measuring 0.9 cm x 0.4 cm x 0.3 cm, oval in shape, irregular surface, light brown with gray areas and firm consistency. The whole specimen was placed in the ENES 58-18 capsule for processing (Fig. 4).

Fig. 4: A single soft tissue specimen was received from the ventral surface of the tongue fixed with 10% formalin, measuring 0.9 cm x 0.4 cm x 0.3 cm, oval in shape, irregular surface, light brown with gray areas and firm consistency
The microscopic evaluation reported the following: cavity composed of amphophilic material compatible with mucin, scarce foamy macrophages, bacteria, chronic, moderate and diffuse inflammatory infiltrate and erythrocyte extravasation. The specimen is surrounded by a pseudocapsule of dense fibrous connective tissue with profuse vascularization with vessels in hemocongestion. Towards the surface, parakeratinized stratified squamous epithelium with acanthosis was observed (Fig. 5) so the diagnosis was mucosal extravasation.
According to the clinical and histopathological correlation, the diagnosis made was mucocele associated with the glands of Blandin-Nuhn.
A week later, the patient attended the post-surgical appointment. He was in good general condition, had a clean wound and was in the process of recovering; the stitches were removed and indications given.
Within one month of the surgical procedure, an assessment was made and adequate repair was observed without lesion recurrence or permanence.
Discussion
Mucoceles of the glands of Blandin-Nuhn are rare oral mucosal lesions3,6 that may be confused with other lesions given their clinical characteristics and location7.
In 1970, Heimansohn reported the first case of mucocele of the glands of Blandin-Nuhn in a 14-year-old woman12. These lesions account for approximately 2-8% of all mucoceles11. Furthermore, in the series published by Jinbu et al.13, mucoceles of the glands of Blandin-Nuhn account for 9.9% of all the oral cavity mucoceles they studied.
Therefore these mucoceles are considered uncommon in the population as they appear between the anterior and ventral muscles of the tongue, a region with greater protection and less susceptibility to physical and mechanical trauma14.
However, in 2009 Moraes et al.15) reported that the low prevalence of mucocele of the glands of Blandin-Nuhn is due to misdiagnosis, lack of diagnosis or easy rupture, so it cannot be considered a rare injury.
Andiran et al.16 stated that the age of occurrence of this type of mucocele is 10 weeks to 26 years, with a peak in the second decade, which is consistent with our case and that described by other authors. However, mucocele of the glands of Blandin-Nuhn can occur at any time during life2.
They seem to appear more often in females13,16-17, including what Jinbu et al. found13, who indicate that women are more affected than men in a 4:1 ratio, which contrasts with our case.
In general, mucocele associated with the glands of Blandin-Nuhn may be located anywhere on the ventral surface of the tongue6.
Joshi et al.17 found that 24 out of 30 lesions were located in the midline and only 6 occurred lateral to it; this lateral presentation is rare11,13,15.
Mucoceles vary in size from 2 mm in diameter to approximately 20 mm6.
Most cases of mucocele of the glands of Blandin-Nuhn are polypoid4,10, while other authors state they are tube-shaped14.
Color variation depends on the size of the lesion, its proximity to the mucous surface, and its elasticity18.
The histopathological study of this type of mucocele shows an area of spilled mucin without epithelial lining (pseudocapsule) surrounded by a granulation tissue response, chronic inflammatory infiltrate, foamy macrophages and in some cases a damaged salivary duct that can be identified by irrigating the area19.
Treatment of mucoceles associated with the glands of Blandin-Nuhn is variable. Surgical excision is the treatment of choice20; some authors recommend removing the minor salivary glands involved4, including their associated duct (2, but with caution to avoid iatrogenesis.
Silicone injection may be used to complement surgical therapy to effectively delimit glandular tissue that may be damaged14. However, consideration should be given to the possibility of a foreign body reaction.
Others indicate that larger lesions are treated with marsupialization and micro-marsupialization7,18, which is consistent with Banu, et. al.’s findings6.
Conservative alternative treatments include laser ablation, cryotherapy, electrocautery, and intralesional corticosteroid injections6,21-23.
Finally, the application of microwave ablation as an alternative treatment in mucoceles of salivary glands on the ventral surface of the tongue is currently being investigated, which would yield ideal results5.
Conclusions
Mucocele associated with the glands of Blandin-Nuhn is a rare lesion, so when diagnosing it, the different clinical characteristics that it may present must be taken into account, which are mainly determined by the depth of the lesion and the degree of keratinization of the lining mucosa. In addition, we must consider its histopathological characteristics, as well as the data provided by the patient such as history of trauma and periods of size variation of the lesion in order to assess the possible specific differential diagnoses based on specificities.
It is essential to make an accurate diagnosis since the lesion, depending on its characteristics, can cause alterations in certain functions, which may affect the patient’s quality of life. Therefore, treatment should be timely, appropriate and specific for each individual, considering the characteristics of the case such as exact location, size and shape of the injury, patient’s age, systemic implications and history of recurrence, in order to avoid complications.
Therefore, it is recommended that studies be conducted to determine the efficacy of each type of treatment, including newly published treatments such as microwave ablation, following certain standardized criteria.
REFERENCES
1. Neville BW, Damm DD, Allen CM, Chi AC. Oral and Maxillofacial Pathology. 4th ed. United States American: Elsevier; 2016. [ Links ]
2. Shammay N, Mandel L. Mucocele of Blandin-Nuhn. The New York State Dental Journal. March 2018: 27-29. [ Links ]
3. Krzysztof Jachewicz T, Nyrka B. Mucocele of the Glands of Blandin-Nuhn-Case Report. Dent. Med. Probl. 2016; 53 (1): 142-146. [ Links ]
4. Rajalakshmi R, Shabana Fathima S, Sajeev R. Mucous extravasation phenomenon of lingual glands of Blandin and Nuhn. Journal of Orofacial Research. July-September 2013; 3 (3): 230-232. [ Links ]
5. Feng H, Wang S, Liu Y, Liao X, Tang Y, Liang X. Microwave Ablation: A Novel Treatment for the Mucoceles of Anterior Lingual Salivary Glands. J Oral Maxillofac Surg. 2017; 75: 530-535. [ Links ]
6. Banu V, Kishor Kanneppady S, Anusha RL. Mucocele of the glands of Blandin-Nuhn. International Dentistry-African edition. 2013; 3 (6): 26-29. [ Links ]
7. García León N, Marrugo Pardo GE. Mucocele of the glands of blandin nuhn: a case report. Colomb. Med. 2013; 43 (1): 46-47. [ Links ]
8. Stojanov IJ, Malik UA, Woo SB. Intraoral Salivary Duct Cyst: Clinical and Histopathologic Features of 177 Cases. Head and Neck Pathol. 2017; 11: 469-476. [ Links ]
9. Khalekar YJ, Sande AR, Zope A, Suragimath A. Mucocele of tongue: A rare case report. J Indian Acad Oral Med Radiol. 2016; 28(4): 462-464. [ Links ]
10. Subalakshmi K, Jayakumar J, Rani SA, Justhius Fabi BA, Arun R, Bhagya Lakshmi S. Mucocele of the Glands of Blandin-Nuhn; A Rare Entity A Case Report. Journal of Dental and Medical Sciences. 2016; 15 (12): 35-37. [ Links ]
11. Shaik N, Shanbhog R, Suhas Godhi B, Krishna Degala S. Mucocele Involving the Glands of Blandin and Nuhn: A Rare Case Report. Int J Pharma Res Health Sci. 2017; 5 (6): 1915-1918. [ Links ]
12. Heimansohn HC. Mucocele of anterior lingual tongue glands: report of a case. Dent Dig. 1970; 76: 470-471. [ Links ]
13. Jinbu Y, Kusama M, Itoh H, Matsumoto K, Wang J, Noguchi T. Mucocele of the glands of Blandin-Nuhn: clinical and histopathologic analysis of 26 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003; 95: 467-470. [ Links ]
14. Silva-Santos IK, Melo de Matos JD, Pereira-Lucena FJM, Cavalcante-Pereira N, Cavalcante-Pita NI, Eversong Lucena de Vasconcelos J. Mucocele in Blandin-Nuhn Glands: Case Report and Integrative Review. International Archives of Medicine. 2016; 9 (392): 1-7. [ Links ]
15. Moraes PC, Bönecker M, Furuse C, Thomaz LA, Teixeira RG and Araújo VC. Mucocele of the gland of Blandin-Nuhn: histological and clinical findings. Clin Oral Invest. 2009; 13: 351-353. [ Links ]
16. Andiran N, Sarikayalar F, Unal OF, Baydar DE, Ozaydain E. Mucocele of the anterior lingual salivary glands from extravasation to an alarming mass with a benign course. Int J Paediatr Otorhinolaryngol. 2001; 61:143-147. [ Links ]
17. Joshi SR, Pendyala GS, Choudhari S, Kalburge J. Mucocele of the Glands of Blandin-Nuhn in Children: A Clinical, Histopathologic, and Retrospective Study. N Am J Med Sci. 2012; 4 (9): 379-383. [ Links ]
18. Baurmash HD. Mucoceles and Ranulas. J Oral Maxillofac Surg. 2003; 61: 369-378. [ Links ]
19. Adachi P, Pires AM, Horikaw FK, Shinohara EH. Mucocele of the glands of Blandin-Nuhn-clinical, pathological, and therapeutical aspects. Oral Maxillofac Surg. 2011; 15: 11-13. [ Links ]
20. Khalekar YJ, Sande AR, Zope A, Suragimath A. Mucocele of tongue: A rare case report. J Indian Acad Oral Med Radiol. 2016; 28 (4): 462-464. [ Links ]
21. Kopp WK, St-Hilaire H. Mucosal preservation in the treatment of mucocele with CO2 laser. J Oral Maxillofac Surg. 2004; 62: 1559-1561. [ Links ]
22. Twetman S, Isaksson S. Cryosurgical treatment of mucocele in children. Am J Dent 1990; 3:175-176. [ Links ]
23. Rezende K.M. Cryosurgery as an effective alternative for treatment of oral lesion in children. Braz. Dent. J. 2014; 25: 352-356. [ Links ]
Authorship contribution 1) Conception and design of study 2) Acquisition of data 3) Data analysis 4) Discussion of results 5) Drafting of the manuscript 6) Approval of the final version of the manuscript
Received: October 12, 2019; Accepted: January 06, 2020











 texto en
texto en