Servicios Personalizados
Revista
Articulo
Links relacionados
Compartir
Odontoestomatología
versión impresa ISSN 0797-0374versión On-line ISSN 1688-9339
Odontoestomatología vol.21 no.33 Montevideo jun. 2019 Epub 01-Jun-2019
https://doi.org/10.22592/ode2019n33a3
Investigación
The oral component in the representations of the health-disease-care process built by institutionalized youth in the city of Córdoba, Argentina
1PROCON (equipo interdisciplinario de investigación en promoción contextualizada), Carrera de Doctorado, Facultad de Odontología, Universidad Nacional de Córdoba, Argentina. Hayas de la Torre S/N, Ciudad Universitaria, Córdoba, Argentina.marcebarnetche@yahoo.es
2PROCON (equipo interdisciplinario de investigación en promoción contextualizada), Carrera de Doctorado, Facultad de Odontología, Universidad Nacional de Córdoba, Argentina.
Health is a social construction built from different interacting dimensions: biological, environmental and social, which interact with people’s lifestyles, understood in a broader sense, as a result of decisions taken both individually and collectively.
Objective:
The aim of this research was to know the representations of the health-disease-care process in general and of the oral component in particular held by institutionalized youth housed in socio-educational centers of the Juvenile Criminal Area of the Province of Córdoba, Argentina.
Results and conclusion:
The representations of the health-disease-care process of these youth in confinement include the oral component as part of general health, from experiences of suffering, mainly through physical pain and self-care, but also given its aesthetic importance.
Keywords: adolescents’ integral health; oral health; youth; institutionalization
La salud es una construcción social elaborada desde diferentes dimensiones interactuantes: biológica, ambiental y social en interacción, con los estilos de vida de las personas; entendida en un sentido más amplio como resultante de decisiones tomadas tanto en el plano individual como colectivo.
Objetivo:
El propósito de esta investigación fue conocer las representaciones del proceso salud enfermedad atención en general y del componente bucal en particular que poseen los jóvenes en situación de encierro alojados en centros socioeducativos del Área Penal Juvenil de la Provincia de Córdoba, Argentina.
Resultados y conclusión:
Las representaciones del PSEA de estos jóvenes en situación de encierro, incluyen al componente bucal como parte de la salud general, a partir de situaciones de padecimientos, principalmente por el dolor físico y su autoatención, pero también por la importancia estética.
Palabras clave: Salud integral del adolescente; salud bucal; jóvenes; institucionalización
Introduction
Health is a social construction built from different interacting dimensions: biological, environmental and social, which interact with people’s lifestyles, understood in a broader sense, as a result of decisions taken both individually and collectively 1. Young people’s health is an essential factor in the economic and political process in all countries, especially in disadvantaged nations such as Latin American countries 2. As expressed by the WHO3, the physical, mental and social health of young people is the result of past and present experiences, which act as determinants of well-being in later life. In this sense, events and environments that disturb or favor growth and development during the fetal period, childbirth, childhood and the school stage, among others, are of interest, as they may be positive or have consequences of varying severity when reaching youth.
In turn, while oral health is essential for the quality of life and well-being of each person, it is rarely included in the health-disease-care process, both individually and collectively.
Oral health status affects people’s vital functions such as eating, communication, affection, sexuality, among other aspects of a physiological, psychological and social nature4.
The World Health Organization (WHO) 5 considers dental caries and periodontal disease among the most prevalent oral conditions. Craniofacial abnormalities and malocclusions are moderately frequent, while oral soft tissue pathologies, tooth tissue disorders, maxillofacial trauma, and dental fluorosis are of variable frequency.
Most young people in conflict with criminal law who are housed in socio-educational centers in the Juvenile Criminal Area of the Province of Córdoba become familiar with eating, hygiene, and study habits, among others, when entering these establishments. In many cases, it is in these institutions where they go to a dental appointment for the first time, where they express their needs, ailments and experiences of pain. They also state that they have never seen a doctor, let alone a dentist, highlighting the inequalities in access to healthy habits, such as periodic clinical examinations, which can prevent oral diseases 6.
The young people housed in these socio-educational centers can be considered socially vulnerable, which is understood as the result of the combination of various factors: age, gender, social and economic aspects, etc. that prevent subjects/groups from joining development and accessing better conditions of well-being7.
When we think about researching social representations in relation to health and disease, it is interesting to reflect on the concept of health and its significance.
Some authors8 understand the concept of health-disease as a collective of all the social influences and determinants that emerge in the structures and functions of the social groups we are part of. Others9 add that this process integrates biology, ecology, sociology, culture, the experience of each individual and the value they give to life. Lalonde10 introduces the idea of health fields and says that the biology of the human organism, environment and lifestyle are as important as the organization of health services.
Currently, health and disease move from categories opposed to conceptualizations articulated in a dynamic event called health-disease-care process (HDCP)11-12.
Social representations provide visibility to the processes of subjective configuration of reality. These processes are ways of understanding, judging, deciding and acting in the everyday life of individuals in fragments of a given reality, which at the time of becoming vital events, give sense to the subjects’ biographies and life stories13.
When talking about interpretations of realities in plural and singular, we assume that reality is not one, but is constructed according to the experiences, perceptions and singularities of the subjects in their collectives. The object of social representations focuses on symbolic interactions that make the senses in human expressions objective, such as places, implicit and explicit agreements, rules, words, lifestyles in agreement and conflict, which make up the way subjects think and feel. Representations are not found in an isolated subject, nor in society as a group of individuals, but are processes and products of intersubjectivity3 13.
Social representations are action guidelines and a framework for reading reality; they are systems of meanings that allow us to interpret social events and actions. They express the relationships that subjects have with each other in their context; they are programs of perception, constructions with a theoretical scope, for which they contain valid knowledge, despite having knowledge that can be demonstrated through logic14.
The concept of social representations was introduced by Moscovisi15, who defined them as a cognitive and symbolic product about a social object created by a group and used to enable communication among the group members16. Social representations are a system of values, ideas and practices that have two functions: human dominance over nature and communication among members of a community18. Jodelet19 defines social representations as the knowledge of common sense. It is knowledge that is built from experiences, also the information, knowledge and thought models that individuals receive and transmit through tradition, education and social communication.
Social representations are presented in varying and more or less complex forms. They are images that condense the meanings, reference systems that allow subjects to interpret what happens to them, and also give meaning to the unexpected. These categories allow subjects to classify the circumstances, phenomena and people with whom they relate. They are theories that allow us to design performance in everyday life, and when we understand them within a specific reality of social life, they are all this combined18.
In this context, the HDCP is a social representation, which is an individual and social construction through which subjects design their suffering, thus conditioning the types of aid to be sought. Feeling healthy or ill is not the same for all individuals: it depends on the geographical area of residence, socioeconomic level, level of education reached, perception of the world, etc. Each social group has a conception of what it is to be healthy or ill, which are the positive or negative behaviors for their health, and this determines whether or not the individual feels the need to apply the practices they have built as healthy20. According to the culture and organization of a given society, a subject develops different concepts about health, disease and how to alleviate it, as well as prevention and health promotion actions21. Kleinman22 integrates the concepts of disease, illness and sickness, pointing out that sickness is a social and cultural connotation, and that disease and illness are socially constructed, where illness precedes sickness, and is how the subject perceives, expresses and contends in the disease process. Some authors22-23 emphasize the subjectivity of individuals regarding illness, disease, and how experience and meanings are modulated according to social structure. Others24 suggest that biological and psychological states are related in the disease process, while illness is within the domain of language and meanings, so they make up the experience.
Understanding the subjective experiences that the subject goes through helps to understand the complexity of the health-disease-care process, so the role of culture and social relationships must be considered. Globally, there is little information about youth representations on the HDCP. In this regard, in the region, Lucero25 states that since there are different youths, their representations are regulated by their own contexts.
A holistic view is needed to understand and solve the complex processes involving health in order to improve people’s existence. This is why the aim of this research was to know the representations of the health-disease-care process in general and of the oral component in particular held by youth housed in socio-educational centers of the Juvenile Criminal Area of the Province of Córdoba, Argentina. The information collected will help build contextualized strategies for health care and promotion in this age group in this particular context.
Methodology
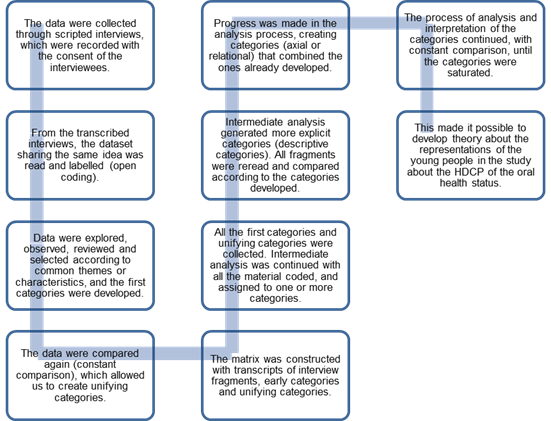
A qualitative study was conducted considering the regulations of the Council for International Organizations of Medical Sciences26. The work protocol (Fig. 1) was approved by the Advisory Council of the Doctoral Degree of the School of Dentistry of Universidad Nacional de Córdoba (UNC). To have access to the representations on HDCP in general, and on oral health status in particular, of young people institutionalized in socio-educational centers of the youth detention centers in the Province of Córdoba, a scripted interview27 was conducted with 32 young people, aged 14 to 18, of both sexes, institutionalized for at least six months in the socio-educational centers of Complejo Esperanza. The complex includes a 52-hectare plot outside the common land of the City of Córdoba; at km 14.5, on Camino de 60 cuadras, where there are four educational centers: Module I (formerly Horizons), Module II (formerly Nuevo Sol), Module III (formerly Pasos de Vida), Module IV (formerly San Jorge), which house males aged 12 to 20, in conflict with criminal law from the Province of Córdoba The center that houses young women in these circumstances is CESAM, which is currently located in Nueva Córdoba neighborhood in the city.
The interviews were conducted by a single researcher individually, on one day and in the offices of the technical teams (psychologists and social workers) of the different centers. They lasted 50 minutes. The thematic guidelines derived from the objectives of the research and the evolution of the interview were permanently in sight: sociodemographic profile, work history, leisure time, peer group, family group, customs, contextual cultural patterns, internalized perception of the body itself (real and ideal), substance consumption, health-disease-care process. The interviews were recorded, and simultaneously, during the microsituation, fieldnotes were taken to record impressions, sensations, attitudes and characteristics of the young people.
Then the lead researcher obtained the specific corpus with the verbatim transcript after transcribing the interviews.
Information was analyzed according to the Grounded Theory28. The process of data collection, processing, and analysis was performed as shown in figure 1.
Finally, alphanumeric codes were used to show the cases that support the results presented in this study.
Results
Socio-demographic characteristics of the group under study
The framework study included 70 young people, 94% male and 6% female, aged 14 to 18, with an average age of 16.91±1.11, while 37% were aged 18. Of these, 34% completed primary education, 69% live in the City of Córdoba and 69% have informal employment records1,29-31.
Of the young people participating, 29% come from nuclear families, 26% from single-parent families; only 1% stayed in public welfare institutions as per court decision. The role of head of household is the mother in 36% of cases, with a job in the informal market in 67% of cases. Thirty-six per cent of heads of household completed full primary education1,29-31.
Ninety-three per cent of the young participants live in traditional housing; 90% have water from the public network and 81% have urban transport stops close to their homes1,29-31.
The analysis of the corpus and the fieldnotes recorded showed with great richness the different ways in which institutionalized youth see, understand and construct the representations of the health-disease-care process.
Concept of health/disease
Several representations appear in the discourse of the young participants in this study. Many of them describe health as an individual state of their own, related to the absence of disease and pain:
... “to be well, not to have anything bad, when nothing hurts.” (Mr0001, male, 18 years old)
Others complement this construction associated with emotional well-being and that of the family:
“Health means that I am healthy, that my family are healthy... as we are all well now, that is, with no problem, we are all healthy... and nothing should happen to them.” (D0006, male, 17 years old)
Some young people associate being healthy with non-use of psychoactive substances and with healthy practices:
“No smoking, no taking drugs, no drinking. If you want to be healthy, you have to do some exercise, go to the gym, you have to be strong body (sic.). I always heard that. As I saw my cousin playing football, he always gets up in the morning, drinks yogurt like this, has milk from the sachet like this.” (V0016, male, 18 years old)
In contrast, they describe disease from the pain or illness and describe it from the symptoms:
“When I feel pain.” (H0002, male, 18 years old)
They expand this information by connecting the disease to the consumption of psychoactive substances, connecting health imbalances with the consequences of problematic substance use:
“...I got sick, once I was smoking cocaine base and my head boiled all over; I smoked only once and well, my head boiled, I don’t know, and I felt like fainting.” (C0020, male, 16 years old)
These positions on how these subjects define health and disease result from subjective and personal processes, influenced by a permanent exchange in their context of beliefs, values and socio-economic and cultural environment20.
Use of health services
These young people say that feeling sick can be the gateway to health services, in order to ease pain and get medication.
Many respondents cite the reasons for attending health centers, describing some of the therapeutic pathways32.
“When something happened to me, it was strange that it happened to me... When I cut the tip of my finger, I tore it off with a piston, I went there too and they wanted to put it back together with glue. But they sent me to the hospital, but I didn't have the other piece of the finger. I had X-rays taken... But then for something else? Vaccines... But I haven’t been there for other reasons, no!” (B0007, male, 16 years old)
“...I brush, and here I got everything fixed so that it doesn’t hurt.” (Mr0001, male, 18 years old)
Previous experiences of the HDCP, both personal and of family members or close people, characterize the process, which lead to minimizing the importance of the process:
“... it was very difficult for me to get sick. I never got sick. Twice I had problems; one was when I had hepatitis and the other I had... No, just hepatitis.” “... I was very young and, 8 years old. And to my mom, I told my mom and they took me to the hospital...” (G0004, male, 18 years old)
Naturalization of diseases for children and the existence of control programs at this stage.
“The only disease I had, other than chickenpox, which is normal, was hepatitis; the only thing, between the ages of 11 and 12.” (F0014, male, 18 years old)
“... they take my little brother. They’ take him to the check-ups, because they’re still kids. They take him to the doctor or when they get the flu.” (F0003, male, 16 years old)
HDCP in the oral health status
The HDCP in the oral health status is of paramount importance to people. Pain is the main sign they recognize as an indicator of the imbalance in the oral health status, which leads them to believe that premature tooth extraction is a quick and effective resource.
In the different stories narrated by the young respondents, health is described as a state of absence of disease and fundamentally of pain when referring to oral health:
“... I think that health is when you’re OK, when things don’t hurt, your knee doesn’t hurt like that, or to be OK with your tooth, when your tooth doesn’t hurt, you know? When your head doesn’t hurt and you’re OK, you know? That’s what I think it is.” (I0024, male, 18 years old)
The aforementioned positions are influenced by the following emerging properties:
Naturalization that the accessible treatment for them is tooth extraction.
“because my mom doesn't have any molars here or here like this; she’d go to get her teeth pulled out. And she had her molars pulled out just like that.” (M0009, male, 15 years old)
Avoiding embarrassment motivates seeking dental care. The importance of aesthetics helps overcome the fear of seeking dental care.
“My sister went the other day because she had a problem with her front tooth and had it fixed; she didn’t like the way she had it black. Also, it broke a little and she had a party and was ashamed to have her tooth like that. And she had to go! She didn’t t like it before because of the anesthesia. The last time they had to pull out a molar, she made a big fuss.” (V0030, female, 16 years old)
They find no economic or geographical barriers, but symbolic ones, to access health services.
“I was a block away, but I didn’t go because the police were there, there was a policeman outside; and they were looking for me, I was on the run. So I wasn’t going anywhere; I was like that for a long time.” (G0032, male, 18 years old)
Self-care: beliefs, knowledge, therapeutic pathways in the process of caring for the body and the oral health status
Self-care is considered an essential component of the health-disease-care process34. The practices are aimed at caring for your body and oral health condition in order to avoid pain and disease.
“...protect yourself from the cold, from diseases. And I take care of myself, you have to keep warm, everything.” (F0003, male, 16 years old)
“I brush my teeth, try to eat little candy and gum. I like that a lot. I always bought lollipops, also chocolate sandwich biscuits.” (V0030, 16 years old)
Care is only given in situations of illness, otherwise if there is no disease, there are no self-care practices:
“In the street you don’t really do anything to be healthy, yes, I did drugs, everything, what I didn’t do was smoke cigarettes or drink alcohol, nothing.” (I0010, 18 years old)
Eating practices are subject to practices that affect health:
“... I don’t like to eat throughout the day; because I'm smoking weed all day, and I don’t like eating when I smoke because you lose the high (laughing). (He interrupts and clarifies:) Here I eat every day, but not on the street. I only like to eat in the evening. I don't like breakfast, tea, nothing, I don’t like to have lunch. Only dinner.” (K0022, male, 18 years old)
Intentional self-care practices for the HDCP in the oral health status appear when there is pain and illness:
“I put on ice, I put on something, I couldn’t, I couldn’t stand it... No! (he smiles) Then, with the ‘muelita’, that’s what it’s called... I don’t know what it’s like... it’s like a red paste, I used to apply it. Oh, and I also got tired of healing myself with a toad. I put the toad’s belly like this (points to area of face), I washed the toad and put it like this... I did it a lot, and now my tooth no longer hurts. After I rubbed the toad, it didn’t hurt anymore... I brushed my teeth and it went away. I prayed and asked God to help me to be healthy...” (F0008, male, 18 years old)
“...you buy pills to calm you down, you smoke a joint, everything (he laughs).” (H0002, male, 17 years old)
“... when my tooth ached, maybe I put drugs there... It goes numb.” (I0024, male, 18 years old)
The woman in the mother role is responsible for guiding the self-care process:
“... I was telling my mom, look, I feel bad, I don’t know, I’m about to catch the flu. And well, my mom would buy me something for the flu or something. She could tell. Because a mother notices when you feel bad. She would help me like this or buy something so it would go away or do something.” (K0022, male, 18 years old)
Practices that affect people’s health
In the discourses associated with unhealthy practices, most young people considered they were associated with harmful factors such as psychoactive substance (PAS) use:
“... you get skinny like that, because it consumes you! If you eat a plate of food and eat fruit, everything, you go and get drugged it does nothing to you, it’s as if you hadn’t done it. I realized this because the arm, here, I had it like this. I would grab here and do like this (surrounds wrist with thumb and index finger), and I had nothing like this.” (M0009, male, 15 years old)
They describe the different effects of each PAS:
“Smoking weed is like I’m laughing my ass off all day, I don't think about anything. And cocaine, because I liked it. One, I love the taste of cocaine, I love it; and it depends on where you take it, because if you take it at the dance club, if it's good, everything becomes a party. But you take it when we’re sitting, at some of the boys’ place, you stay like that, still, still. Cocaine tastes bitter.” (B0007, male, 16 years old)
Most report starting PAS use at an early age:
“At 12, first with joints, then with drugs and then with pills. At 12, everything together.” (K0022, male, 18 years old)
Some justified PAS use to gain the acceptance of peer group:
“I tried and I didn’t like them. It was the typical thing that some assholes do to say everyone does it. I also want to do it to feel older and you try it, and I didn’t like it and I quit...” (F0014, male, 18 years old)
None of the participants mentioned barriers to accessing psychoactive substances:
“... there in the neighborhood, as if nothing. If you were going to a neighborhood, you would ask where they sell this (he touches his nose) and they would tell you...” “And the pills? I never went to buy a pill myself. We would take them from the eldest guy’s aunt, she had them prescribed... And we would take her pills. But buying pills, or withdrawal because of a pill… Never!” (B0007, male, 16 years old)
Young people mention the use of marijuana associated with increased frequency of sugar consumption:
“In the street, when you smoke marijuana, you feel something in your gut (points to stomach) like this, you get hungry for sweet things, like your blood pressure goes up and you get hungry for sweet things. And well, I’d buy candy, it was always like that.” (M0009, male, 15 years old)
“... you feel like you’re starving... I don’t know why. You feel like eating sweet things, like this, or savory, whatever you like, what you want to eat. You get hungry like this… and I don’t know why.” (F0003, male, 16 years old)
Tobacco consumption is mentioned among the practices that affect health. This habit is associated with the circumstances experienced: they smoke in their current confinement situation:
“Not outside, I started smoking here.” (G0004, male, 18 years old)
They smoke out of anxiety and boredom:
“...I smoked two packets a day, three when I was bored.” (N0005, male, 15 years old)
And some also say they consume tobacco socially:
“On the weekend, I could smoke everything, two or three packets a night.” (B0007, male, 16 years old)
Regarding alcohol consumption, most young people refer to its consumption as social:
“Very little. On weekends…” (B0007, male, 16 years old)
Many of the participants gave a glimpse of the responses of their family group regarding the consumption of psychoactive substances, where two conflicting situations were reported. First, the naturalization of PAS use in the family:
“... they knew that I did drugs. I’d lie in bed with a plate of cocaine, I’d have a plate, and I’d always buy 50, 100 grams of drugs. It was hard for me to go to sleep and I’d take pills, and the next day I would get up and the things were there, and my mom had to go through my room to reach the bathroom. Maybe I’d gone to bed and left a joint there, or I’d be smoking a joint in my room and my dad would come in and all he would tell me was to spray deodorant when I was done smoking and turn on the fan and spray deodorant.” (K0022, male, 18 years old).
And second, a clear family disagreement over PAS use:
“They’d give me hell and tell me I was being a jerk, but they wouldn’t tell me to quit. But it’s not like they told me to stop using or to get my shit together. They always told me to stop fooling around... My mom, my dad... Not Cristian. If Cristian saw me smoking something, he would beat the shit out of me.” (B0007, male, 16 years old)
Discussion
From the perspective of Bordieu’s construction of reality33, every person has a set of existential conditions of cultural, social and economic nature with which they construct a scheme or structure (habitus) of practices and representations that they use to produce and regulate their actions and respond to the HDCP.
The personal and subjective construction of the complex HDCP can only be understood contextualized in the universe of beliefs, values and sociocultural environment of each person and also their material living conditions34. Currently, the HDCP is considered as the way in which subjects define health and disease based on the relationship they establish with society35. Health and disease are not analyzed as entities, whose definition is evident, but as a result of social processes, intellectual constructions and continuous exchanges of the community36.
In this sense, institutionalized youth define the HDCP as an individual state of their own, related to the absence of disease, evidenced mainly by pain. This is a similar meaning to that found in other studies with schoolchildren from different contexts of the City of Córdoba, where health is associated as a static situation and absence of disease25.
They also relate health to emotional and family well-being; here we can glimpse the affective ties linked to their families. On the other hand, they associate it with the non-use of psychoactive substances and healthy practices. Disease is described from the suffering, pain and symptoms, which motivate the use of health services.
Accessibility is how people reach health services; where there is a link between the supply of and demand for care. This association is influenced by different barriers: geographic (whether a landform or a man-made barrier), economic (such as lack of money, both for transport and for buying medicines, etc.), administrative (difficulty imposed by the organization such as opening hours or shifts) and symbolic, where the social imagination and representations could act as barriers37. In this study, young people mention that most of their neighborhoods have health centers within a 10-block radius, and if they are further away, they have the means to reach them. They are free services, and those attending private services have social welfare coverage (they are the minority). Although they perceive no geographic or economic impediments, the youth mention some difficulties, such as inadequate opening hours and/or long waits, among others.
Institutionalized youth recognize as unhealthy practices the use of psychoactive substances, the early onset of use and the ease of accessing them in their context of origin. They can describe the effects produced by the different substances, notably differentiated between “joint” and drugs, with pills and cocaine being the most dangerous for them. As in previous studies conducted with young people in school25, young people in conflict with the law naturalize marijuana consumption compared to cigarette consumption. Cocaine, referred to as “drug”, and “pills” (psychiatric drugs), are associated with violence and danger. Their consumption is considered a predisposing factor in the development of their criminal behavior. In turn, they associate PAS use with their eating habits, including a vicious circle they narrate in which food consumption decreases the effects of PAS use.
Tobacco smoking, through cigarettes, is also recognized as a harmful factor, but related differently depending on life circumstances. In confinement, boredom and anxiety lead them to consume, while if they go back to when they were not institutionalized, the motivation was social “when they walked the streets”.
As for alcohol consumption, they associate it with freedom and social activities, such as parties, dances and meetings with friends.
As for PAS, there are two strong positions regarding family response to consumption. One is the family naturalization of PAS use, since several members have or had such practices, and on the other hand the usual disagreement of the mother figure. Although the mother figure is idealized in the symbolic construction of these young people from the affective and containment perspective, it is not legitimized for setting limits.
To analyze the healthy practices of these young people, their beliefs, knowledge, and therapeutic pathways were considered38, where self-care emerges as a process of caring for the body and oral health condition. As already mentioned, self-care is one of the essential activities of the health-disease-care process.
According to Menéndez32, self-care refers to the representations and practices that a subject and/or social group uses to diagnose, explain, attend to, control, endure, cure, solve or prevent health problems that affect their health, whether real or imaginary, without the direct intervention of health professionals.
The young people interviewed report having healthy practices for caring for the body and oral health status to avoid pain and disease, so that if there is no illness, there are no self-care habits. This type of care agrees with what Menéndez32 said, which considers it a broad level of self-care, including not only the care and prevention of suffering, but also the preparation and distribution of food, access to and use of water, household and body hygiene, among others. In this sense, the youth in our study say they were careless regarding their eating habits prior to being institutionalized in terms of distribution, quantity and type of food. They say they did not have four meals a day for various reasons, including PAS use, street activities, or simply not having the habit of having breakfast and tea, as if those meals were something magical or traditional, without being able to identify the causes that affected habit formation.
In turn, Menéndez32 describes restricted self-care, such as representations and practices that a subject intentionally applies to the health-disease-care process, where self-medication is included. This action refers to the decision to use certain pharmaceutical medications, other substances (herbal infusions, marijuana, alcohol, etc.), as well as other alternative activities (poultices, massages, etc.) that are used by subjects and microgroups autonomously to alleviate certain conditions. Likewise, the decision to see a health professional, as well as some actions after the appointment, are part of the self-care process32.
Regarding the restricted self-care reported by the young people in this study, they mention seeking care from professionals, consumption of prescribed drugs and other alternative activities. There also appear self-medication and marijuana as a pain reliever.
Within the family group, the person in charge of this process of self-care, diagnosing the condition, managing it and measuring the severity, is the woman in the role of mother, coinciding with what Menéndez mentions that young people ask their mothers for help when they are sick.
As for the oral health status, tooth loss is naturalized, dental care is sought in order to avoid embarrassment, where aesthetics acts as a factor to overcome the usual fears of seeking care. Here you can glimpse the influence of the context of origin, socialization scenario, where each component (family, peer group, school, and place of residence) plays a characteristic role in building the representations of these young people.
These representations are influenced by personal previous experiences, or of their families and/or close people, that characterize the process, leading them to minimize its importance, naturalize diseases and preventive care for children (programs for the control and development of healthy children). This, as Lucero25 suggests, could be linked to the emotional components associated with the disease. In this sense, the young people in our study do not report events that would cause negative feelings of illness and suffering
Referencias
1. Barnetche MM. Calidad de vida y proceso salud enfermedad atención a nivel del componente bucal en jóvenes alojados en centros socioeducativos del Área Penal Juvenil de la Provincia de Córdoba. Tesis doctoral; en línea. Facultad de Odontología. Universidad Nacional de Córdoba. 2017 (Fecha de acceso: 27 de octubre de 2017). Disponible en: Disponible en: https://rdu.unc.edu.ar/handle/11086/4994 . [ Links ]
2. Tuesca-Molina R, Centeno-Romero H, Salgado MO, García-Delgado N, Lobo- López J. Calidad de vida relacionada con la salud y determinantes sociodemográficos en adolescentes de Barranquilla (Colombia). Rev Sal Univ 2008; 24 (1):53-63. [ Links ]
3. Organización Mundial de la Salud. Documentos Básicos (en línea) 48a ed. Italia: Organización Mundial de la Salud; 2014.p.1. (Fecha de acceso: 20 de marzo de 2015). Disponible en: Disponible en: http://www.who.int/es [ Links ]
4. Luengas I. Tendencias en la formación de odontólogos en la universidad pública en México, en el contexto de la globalización, 1986-2001: una lectura ética. Tesis doctoral. Universidad Nacional Autónoma de México. 2004. [ Links ]
5. Organización Mundial de la Salud. Nota informativa N° 318 (en línea). 2012 (Fecha de acceso: 1 de febrero de 2016) Disponible en: Disponible en: http://www.who.int/mediacentre/factsheets/fs318/es . [ Links ]
6. Barnetche MM. Factores de riesgo de salud en adolescentes con restricción de la libertad en establecimientos correccionales de la Ciudad de Córdoba. Tesis de Maestría. Escuela de Salud Pública. Facultad de Ciencias Médicas. Universidad Nacional de Córdoba; 2009. (Fecha de acceso: 20 de diciembre de 2014) Disponible en: http://fcm.biblio.unc.edu.ar/cgi-bin/koha/opac-detail.pl?biblionumber=18625 [ Links ]
7. Pizarro R. La vulnerabilidad social y sus desafíos: una mirada desde América Latina. Chile: CEPAL (en línea); 2001.p.5-16. (Fecha de acceso: 19 de abril de 2016). Disponible en: Disponible en: http://repositorio.cepal.org/bitstream/handle/11362/4762/S0102116_es.pdf [ Links ]
8. San Martin H, Pastor V. Economía de la Salud. Mc Graw Hill; 1989.p.42-49. [ Links ]
9. Suarez R. Salud - enfermedad: una categoría a repensar desde la antropología. En: Suarez R. Reflexiones en salud: una aproximación desde la antropología. Bogotá: Universidad de los Andes; 2001. p. 11-21 [ Links ]
10. Lalonde, M. A new perspective on the health of Canadians. A working document. Ottawa: Governmet of Canada (en línea); 1981.p.5-7 (Fecha de acceso: 25 de agosto de 2012). Disponible en: Disponible en: http://www.phac-aspc.gc.ca/ph-sp/pdf/perspect-eng.pdf [ Links ]
11. Iriart C, Waitzkin H, Breilh J, Estrada A. Merhy EE . Medicina social latinoamericana: aportes y desafíos. Rev Panam Salud Publica (en línea). 2002 (Fecha de acceso: 27 de marzo de 2016); 12(2):128-36. Disponible en: Disponible en: http://www.unida.org.ar/Bibliografia/documentos/Salud%20Comunitaria/M4/BiblioM4/MEDICINASOCIAL.pdf [ Links ]
12. Granada Echeverry P. El campo de la salud como espacio de construcción simbólica. Rev. Ciencias Humanas. 1999; 6 (20): 1-8. [ Links ]
13. List T, Wahlum K, Wenneberg B, Dworkin S.TMD in children and adolescents prevalence of Pain Gender differences, and perceived treatment need. J. Orofacial Pain. (en línea) 1999; 13(1): 9-20. [ Links ]
14. Botero Gómez P. Representaciones y ciencias sociales: una perspectiva epistemológica y metodológica. Bs As: Ed. Espacio; 2008.p.15-61. [ Links ]
15. Vergara Quinteros MC. Representaciones Sociales en Salud que orientan la experiencia de vida de algunos grupos de jóvenes de la Ciudad de Manizales. Tesis Doctoral. (en línea) Universidad de Manizales- CINDE, Colombia; 2006 (Fecha de acceso: 20 de enero de 2016). Disponible en: Disponible en: http://repository.cinde.org.co/handle/20.500.11907/561 [ Links ]
16. Moscovisi S. Psychoanalyse: Its image and its public. (en línea) USA: Polity Press; 2008.p.54-69. [ Links ]
17. Rizo García M. La intersubjetividad como eje conceptual para pensar la relación entre comunicación, subjetividad y ciudad, en línea. Rev Razón y Palabra.2005. Fecha de acceso: 5 de marzo de 2016. Disponible en: Disponible en: http://razonypalabra.org.mx/anteriores/n47/mrizo.html [ Links ]
18. Winkler MI. Representaciones sociales y prácticas mágico-religiosas en una comuna urbana. Rev Psyche, en línea, 1999; 8(1): 83-91. Fecha de acceso: 2 de enero de 2016. Disponible en: Disponible en: http://www.psykhe.cl/index.php/psykhe/article/view/404/384 [ Links ]
19. Jodelet D. Seminario de Representaciones sociales. Centro Universitario de Ciencias de la salud. Universidad de Guadalajara; 1997 [ Links ]
20. Sacchi M, Hausberguer M, Pereyra A. Percepción del proceso salud enfermedad atención y aspectos que influyen en la baja utilización del Sistema de Salud, en familias pobres de la Ciudad de Salta. Salud Colectiva. 2007; 3 (3):271- 283. [ Links ]
21. Burak SD. Adolescencia y juventud. Viejos desafíos en los albores del nuevo milenio. En: Burak SD (comp).Adolescencia y juventud en América Latina. Libro Regional Universitario. Costa Rica: Ed. Tecnológica; 2001.p.20-36. [ Links ]
22. Kleinman, A. Patients and healers in the context of culture (en línea). Berkeley University Press; 1980.p.24-70. (Fecha de acceso: 5 de enero de 2016). Disponible en: Disponible en: https://journals.google.com.ar [ Links ]
23. Castro R. The subjective experience of health and illness in Ocuituco: a case study. Soc Sci Med (en línea) 1995 [ Links ]
24. Moreno Altamirano L. Reflexiones sobre el trayecto salud-padecimiento-enfermedad-atención: una mirada socioantropológica Salud Pública de México (en línea) 2007 (Fecha de acceso: 20 de julio de 2015); 49(1):63-70. Disponible en: Disponible en: http://www.scielosp.org/pdf/spm/v49n1/a09v49n1.pdf [ Links ]
25. Lucero MF. Representaciones sobre salud/enfermedad/ atención construida por adolescentes de la Ciudad de Córdoba, Argentina. Tesis Doctoral. Facultad de Odontología. Universidad Nacional de Córdoba. 2013. [ Links ]
26. Consejo de Organizaciones Internacionales de las Ciencias Médicas (CIOMS)/OMS Pautas éticas internacionales para la investigación biomédica en seres humanos. Ginebra; 2002. [ Links ]
27. Yuni J, Urbano C. Técnicas para investigar y formular proyectos de investigación. Vol.2. 2ª ed. Córdoba. Brujas; 2006. [ Links ]
28. Strauss A, Corbin J. Grunded Theory Research: Procedures, Canonsm and Evaluative Criteria. Rev Qualitative Sociology (en línea) 1990; 13 (1):3-21. (Fecha de acceso: 17 de noviembre de 2014) Disponible en: Disponible en: http://med-fom-familymed-research.sites.olt.ubc.ca/files/2012/03/W10-Corbin-and-Strauss-grounded-theory.pdf [ Links ]
29. Barnetche MM, Cornejo LS. Experiencia de caries y calidad de vida de jóvenes en situación de encierro. Rev. Salud Pública (en línea) 2016; 18 (5): 816-826. (Fecha de acceso: 20 de julio de 2017)Disponible en: http://dx.doi.org/10.15446/rsap.v18n5.45565 [ Links ]
30. Barnetche MM, Cornejo LS. Impact of oral health on the quality of life of young people in confinement, Córdoba, Argentina: A mixed methods study. J Oral Res (en línea) 2017 (Fecha de acceso: 20 de julio de 2017). Disponible en: doi:10.17126/joralres.2017.xxx [ Links ]
31. Barnetche MM, Cornejo LS. Oral Health of institutionalizad youth in socio-educational centers of the department of corrections in Córdoba City, Argentina. Rev. Acta Odontol.Latinoam. (en línea) 2017, 30 (3) pp.129-140. [ Links ]
32. Menéndez E. De sujetos saberes y estructuras: introducción al enfoque relacional en el estudio de la salud colectiva. Buenos Aires: Lugar Editorial; 2009.p.25-72. [ Links ]
33. Huerta Alvarado SG. Reflexión medico antropológica, desde la perspectiva de Pierre Bordieu para la atención del enfermo renal. Rev Hospital Gral. M Gea Gónzalez. (en línea) 2001; 4(4): 127-129. (Fecha de acceso: 20 de enero de 2016) Disponible en: Disponible en: http://www.medigraphic.com/pdfs/h-gea/gg-2001/gg014i.pdf [ Links ]
34. Menéndez E. Modelos de atención de los padecimientos: de exclusiones teóricas y articulaciones prácticas. Ciência Saúde Coletiva. 2003; 8(1):185-207. [ Links ]
35. Herzlich C, Pierret J. De ayer y hoy: construcción social del enfermo. Cuadernos médicos sociales; 1988.p. 21-30. [ Links ]
36. Viveros M. La noción de representación social y su utilización en los estudios sobre salud y enfermedad. Revista Colombiana de Antropología. 1993; 30:237-260. [ Links ]
37. Comes Y. Tesis para Optar el Doctorado en Psicología - Universidad de Buenos Aires; 2006. [ Links ]
38. Menéndez E. Hacia una práctica médica alternativa. Hegemonía y autoatención (gestión) en salud. México: CIESAS, Colección Cuadernos de la Casa Chata; 1983. [ Links ]
Received: August 24, 2018; Accepted: February 20, 2019











 texto en
texto en