Servicios Personalizados
Revista
Articulo
Links relacionados
Compartir
Odontoestomatología
versión impresa ISSN 0797-0374versión On-line ISSN 1688-9339
Odontoestomatología vol.18 no.27 Montevideo mayo 2016
Maxillary Sinus Mucocele: Review of case report
Demicheri, Gabriel*, Kornecki, Felipe **, Bengoa, Juan***, Abalde, Hector****, Massironi, Claudia*****, Mangarelli Garcia, Carolina******, Beovide, Verónica*******.
* Associate Professor, Grade 3. O.M.S. III Department and Emergency Clinic. School of Dentistry. Universidad de la República. Uruguay.
gdemicheri1@yahoo.com
** Associate Professor, Grade 5. O.M.S. III Department. Head of the Oral and Maxillofacial Surgery and Trauma Program. School of Dentistry. Universidad de la República. Uruguay.
*** Assistant Professor. Grade 2. O.M.S. III Department. School of Dentistry. Universidad de la República. Uruguay.
**** DDS. Honorary Assistant. O.M.S. III Department. School of Dentistry. Universidad de la República. Uruguay.
***** DDS. School of Dentistry. Universidad de la República. Uruguay.
****** Teaching Assistant. Removable Prosthodontics I and Gerodontology. School of Dentistry. Universidad de la República. Uruguay.
******* Associate Professor, Grade 5. Anatomic Pathology Department and Service. School of Dentistry. Universidad de la República. Uruguay. MA in Oral Pathology. Universidad de la República. Universidad Federal Rio Grande do Sul.
Abstract
Maxillary sinus mucocele is a benign cyst formation that originates within the sinus and is lined by epithelium (sinus mucosa) containing mucus. It is a rare condition for which it might be very difficult to find a suitable therapeutic approach, especially when it involves the orbit, leading to exophthalmos.
This study reports the case of a right maxillary sinus mucocele in a 68-year-old female patient. Through clinical examination, vestibular deformation from tooth 12 to tooth 16 was determined. Radiologic examination showed that the maxillary sinus was affected, with borders near the orbit. An excision biopsy was performed, which showed histopathological findings of maxillary sinus mucocele. Presentation and classic treatment are discussed.
Keywords: Maxillary sinus, Mucocele, Caldwell Luc.
Received on: 09 Jun 15 Accepted on: 18 Feb 16
Introduction
Maxillary mucocele is a benign cyst formation that originates within one of the paranasal sinuses, lined by epithelium (sinus mucosa) containing mucus, which is caused by the progressive accumulation of mucus. It presents a slowly expanding growth and is asymptomatic at the beginning. It develops as a result of an obstruction of the maxillary sinus and/or paranasal sinuses due to chronic sinusitis, polyps, bone tumors, trauma or after surgery (1-2). In general, mucus is aseptic and has a thick consistency (1). Maxillary sinus mucocele is caused by obstruction of the drainage ostium or a compartment of a septate sinus. The wall of the lesion is the sinus membrane and the maxillary sinus expands, resulting in remodeling of the bone walls (1-2). Clinically, it can be associated with swelling of the cheek, diplopia and dental problems. It is generally painless and, when present, pain indicates infection of the mucocele (3). Mucocele develops gradually, and has a higher incidence between the third and fourth decade of life, and there is no reported sex predilection (4-5). When the ostium is closed for a prolonged period of time, without any possibility of aeration and drainage, mucus accumulates slowly. This causes pressure that progressively dilates the sinus, which in the long term can result in bone deformation and destruction. Expansion takes place through the site of least resistance, which in the maxillary sinus is generally the medial and posterior walls (4). Mucoceles in the maxillary sinuses are exceptional, with prevalence ranging from 3 to 10% (6), and they are often secondary to cicatricial bridles from previous surgeries (Caldwell Luc-like) (7-9). A patient who undergoes a procedure in the maxillary sinus can develop a fibrous septum between the lateral margins of the surgical defect, on the anterior sinus wall and on the posterior sinus wall. If it grows to a certain size, it can extend to the zygomatic body and appear in the cheek as a mass of soft tissue, or progress to the inferolateral region of the orbit (11).
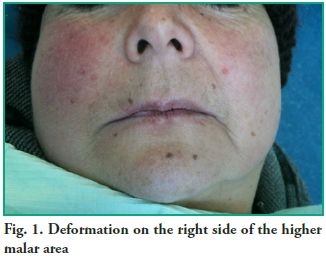
Clinical case A 68-year-old female patient who came to the Emergency Clinic of the School of Dentistry, Udelar, complaining of swelling in the right higher malar area and moderate pain. Intraoral drainage is performed in the vestibular area, near tooth 13, and the patient is prescribed antibiotics (Amoxicillin 875 mg every 8 h). The patient was referred to the Clinic of Oral and Maxillofacial Surgery III with persistence of the swelling but no pain. She has a medical history of controlled but uncompensated hypertension and hypercholesterolemia. She uses upper and lower full prostheses. A deformation in the right side of the face with obliteration of the nasolabial fold (Fig. 1) was observed in the clinical examination of the face. The intraoral examination showed that
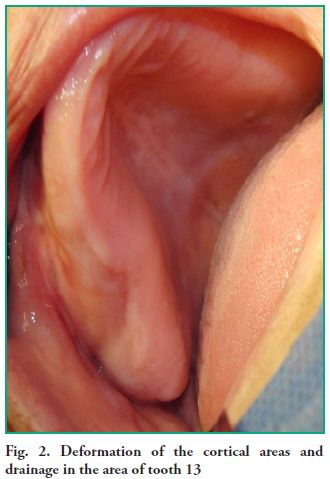
both cortical areas in the right upper quadrant area are deformed by the vestibular area, comprising from tooth 12 to tooth 16. This extends up to the bottom of the sulcus, where it meets the right inner side of the upper prosthesis made twenty months ago. It is worth noting that the color of the mucosa that lines the area and the crest is normal and free of lesions (Fig. 2). The deformation is hard and firm to the touch, both on the vestibular and palatal sides. A small drainage consistent with the therapeutic procedure conducted previously in the Emergency Clinic was found during this palpation.
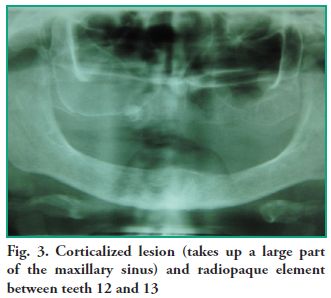
The clinical diagnosis reached was residual cyst, and the differential diagnosis was development cyst, odontogenic and non-odontogenic tumor, and mucocele. Periapical and occlusal radiographies, a teleradiography with a frontal Waters’ view, and an orthopantomography (OPG) were taken. The set of images showed a corticalized lesion measuring, on average, 25 mm in height and 35 mm in length, which is divided by a septum. There is a minor fenestration in the floor of the maxillary sinus, in the rearmost portion. There is also a radiopaque element near tooth 13 that is surrounded by a sharp, radiolucent halo (Fig. 3).
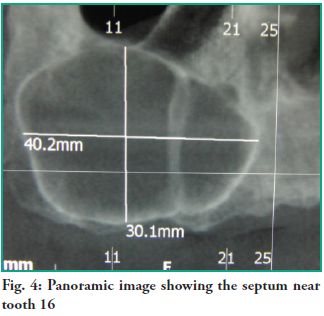
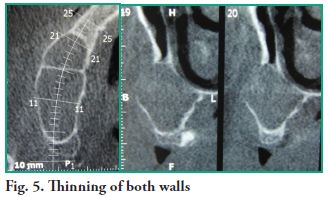
A computerized tomography (CT) scan is indicated for diagnostic purposes and to design a treatment plan. Images were obtained using single cone-beam x-ray CT and corroborated that the lesion measured 40.2 mm in the anterior-posterior direction by 30.1 mm in the vertical direction. All tomographic slices show that the right maxillary sinus is occupied by a lesion with septation near tooth 13, which has not deformed the nasal wall of the maxillary sinus (Figs. 4 and 5).
The initial radiological diagnosis was residual cyst, and the differential diagnosis was mucocele. Treatment plan indicated: prior medical assessment of the patient because of her medical history, approach to the lesion under local anesthesia in order to perform an incisional biopsy and exploratory surgery and/or, possibly, an excisional biopsy.
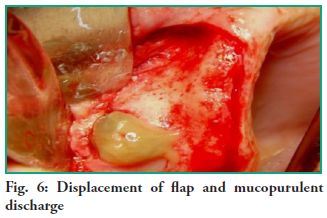
Surgical procedure After administering local anesthesia, a crestal incision was made from the tuberosity area up to around the midline, and a relieving incision near that area. An exploratory puncture, through which a purulent mucus-like content was obtained, was performed before the incision. A full-thickness flap was lifted from the front to the back, exposing a bone fenestration through which an abundant mucopurulent discharge is drained (Fig. 6).
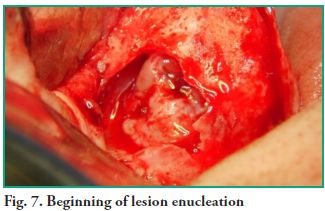
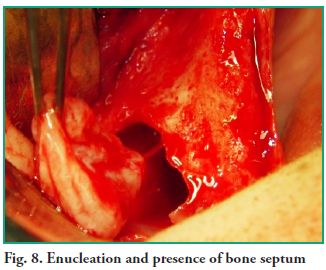
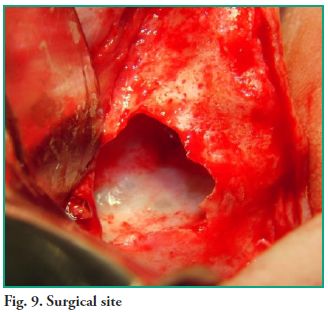
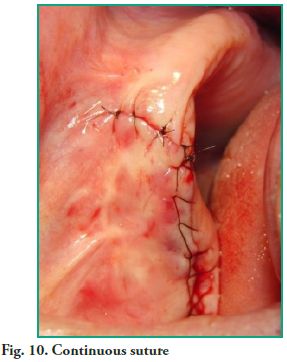
An ostectomy was performed using a rotary instrument and copious irrigation with normal saline is applied to enlarge the fenestration in order to improve visibility. The lesion was fully removed with sinus lift curettes using the enucleation and curettage technique, and the exeresis of the bone septum that divided the lesion was performed afterwards (Figs. 7, 8 and 9). Finally, closure was performed using continuous suture with 5-0 nylon thread (Fig. 10).
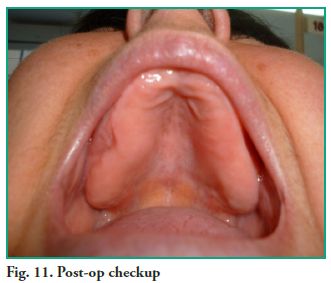
For the postoperative phase, the patient was prescribed Amoxicillin 500 mg every 8 hours for 10 days and Ibuprofen 400 mg every 6 hours for a period of 48 to 72 hours, as analgesic and anti-inflammatory agent. Since no counter opening was made in the inferior meatus, she was prescribed vasoconstrictive nasal drops to keep the ostium patent, for the purpose of facilitating drainage until discharge. The suture was removed ten days later, and the patient’s progress was checked every week for 2 months (Fig. 11).
Pathology report Macroscopic description: Soft, whitish, rounded piece measuring 15 x 15 x 4 mm, an amorphous and gelatinous solid appears when cut, the outer membrane is thin and measures 1 mm. (Fig. 11-bis).
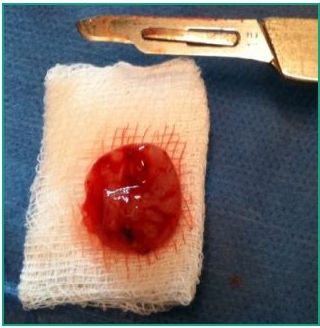
Fig. 11-bis. Enucleated membrane
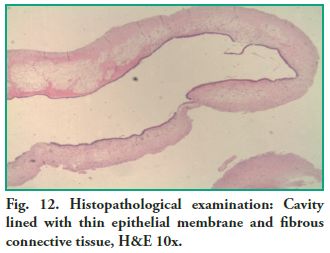
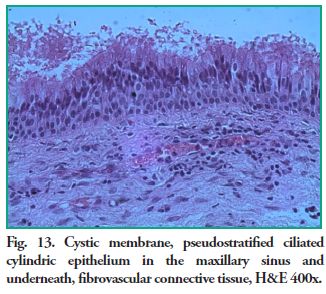
Microscopic description: Cystic cavity lined by a thin membrane made up of pseudostratified ciliated cylindrical epithelium (sinus mucosa), alternating with areas of hyperplasia, supported by fibrous connective tissue, with areas of edema, with plenty of capillaries, some of which are congestive and mixed inflammatory exudates. The content is amorphous and eosinophilic with inflammatory cells (lymphocytes and plasma cells) scattered in mucous material (Figs. 12 and 13).
Discussion
Clinically, the maxillary sinus mucocele can present swelling in the cheek, diplopia and teeth problems, although typically, without pain (3). In the early phases, diagnosis is fortuitous, taking place almost exclusively when a CT of the paranasal sinuses is taken (12). The cone beam computed tomography (CBCT) shows mucoceles as homogeneous, hypodense and isodense masses, as seen in a brain CT (13), and typically shows a rounded contour of bone (13-16), which makes the injection of a contrast medium unnecessary for diagnosis. This bone detail is an added advantage of the CBCT (15-17), since a radiopaque maxillary sinus, without bone erosion, would suggest a diagnosis of sinusitis, polyps and antral retention cysts (18). The typical maxillary sinus mucocele completely opacifies the antrum and expands the sinus cavity (10). During the early stages, it is not possible to differentiate a mucus-filled sinus with a temporary obstruction from a similar obstructed sinus, which will later form a mucocele. The definitive diagnosis can only be reached when there is sinus expansion (12, 19). If there is expansion and destruction of the bone, the differential diagnosis includes malignant conditions, such as adenoid cystic carcinoma, plasmacytoma, rhabdomyosarcoma, lymphoma, schwannoma and odontogenic tumors (14). Traditionally, bone erosion is not associated with maxillary sinus mucocele. In our patient it had thinned both the posterior and medial walls of the maxillary antrum, as described in the reference literature (4), with bone loss near tooth 16. We argue that a large mucocele can cause bone erosion, but the homogeneous nature of the maxillary lesion, together with the preservation of the layers of mucosa adjacent to the eroded bone, reveal the benign nature of the lesion. Histologically, the maxillary sinus mucocele is confined by an epithelial connective capsule made up of normal respiratory mucosa (pseudostratified ciliated cylindrical epithelium), with an underlying chorion that has fibrosis and chronic inflammation. Finding metaplastic squamous epithelium is rare, since the most common lining is ciliated respiratory mucosa (19-21). Many theories have been suggested to explain the mechanisms responsible for the formation and growth of mucoceles, including cystic degeneration of a seromucous gland, even though the histopathological and molecular examinations conducted by Lund et al. (22, 23) study a dynamic process of bone resorption, where inflammation takes part, through cytokines, which act between the bone and the epithelium releasing prostaglandins. These play a key role in the development of a mucocele, along with the sinus obstruction. Mucoceles, in turn, can be caused by a facial trauma or previous surgery which could result in compartmentalized areas such as the one our patient showed (8). Since the diagnosis in this case was uncertain, an incisional biopsy was initially planned, and when the procedure was performed and it was established that the lesion was clinically benign, it was completely removed. No nasal counter opening was made in the inferior meatus as indicated for this kind of procedure, therefore, nasal drops were prescribed to keep the ostium patent. To complement the surgical procedure, the patient was prescribed a dose of 500 mg of Amoxicillin every 8 hours for a period of no less than 7 days and a dose of 400 mg of Ibuprofen every 6 hours for a minimum of 48 hours, as an analgesic agent. The patient progressed favorably in the short term, in the two-month follow-up.
Conclusions
Maxillary sinus mucocele is a benign cyst formation that originates within the sinus and is lined by a cystic membrane made up of pseudostratified ciliated cylindrical epithelium (sinus mucosa) and connective tissue, which contains mucus. It is mainly caused by an obstruction of the sinus opening (ostium). In imaging studies, it has a hypodense appearance with a faint halo, with contours that are commonly crescent-shaped and starting in the paranasal sinuses, and has an expansive tendency defined by thinned bone margins. Recommended treatment for mucoceles of the maxillary sinus without extension is endoscopic drainage with a broad antrostomy of the middle meatus. A Caldwell Luc surgical approach may also be necessary in cases with extension into the soft tissues of the face or the pterygopalatine fossa, or when it has not been successfully drained through endoscopic surgery of the maxillary sinuses (24).
References
1. Costan VV, Popescu E, Stratulat SI. A new approach to cosmetic/esthetic maxillofacialsurgery: surgicaltreatment of unilateral exophthalmosdue to maxillarysinusmucocele J CraniofacSurg. 2013 May; 24(3): 914–916.
2. Mohan S. Frontal Sinus Mucocele with Intracranial and Intraorbital Extension: A Case Report.J Maxillofac Oral Surg [en línea] 2012; 11(3):337–339. Citado 16 febrero 2016. Disponible en: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3428446/3.
3. Mendelsohn DB, Glass RBJ, Hertzanu Y. Giant maxillary antralmucocele. J LaryngolOtol. 1984; 98:305–310.
4. Fu CH, Chang KP, Lee TJ. The difference in anatomical and invasive characteristics between primary and secondary para-nasal sinus mucoceles. Otolaryngol Head Neck Surg 2007; 136:621–625.
5. Stiernberg CM, Bailey BJ, Calhoun KH, Quinn FB. Management of invasive frontoethmoidal sinus mucoceles. Arch Otolaryngol Head Neck Surg1986;112:1060–1063.
6. Natvig K, Larsen TE. Mucocele of the paranasal sinuses-a retrospective clinical and histological study. J LaryngolOtol1978; 2:1075–1082.
Demicheri, Gabriel*, Kornecki, Felipe **, Bengoa, Juan***, Abalde, Hector****, Massironi, Claudia*****, Mangarelli Garcia, Carolina******, Beovide, Verónica*******.
* Associate Professor, Grade 3. O.M.S. III Department and Emergency Clinic. School of Dentistry. Universidad de la República. Uruguay.
gdemicheri1@yahoo.com
** Associate Professor, Grade 5. O.M.S. III Department. Head of the Oral and Maxillofacial Surgery and Trauma Program. School of Dentistry. Universidad de la República. Uruguay.
*** Assistant Professor. Grade 2. O.M.S. III Department. School of Dentistry. Universidad de la República. Uruguay.
**** DDS. Honorary Assistant. O.M.S. III Department. School of Dentistry. Universidad de la República. Uruguay.
***** DDS. School of Dentistry. Universidad de la República. Uruguay.
****** Teaching Assistant. Removable Prosthodontics I and Gerodontology. School of Dentistry. Universidad de la República. Uruguay.
******* Associate Professor, Grade 5. Anatomic Pathology Department and Service. School of Dentistry. Universidad de la República. Uruguay. MA in Oral Pathology. Universidad de la República. Universidad Federal Rio Grande do Sul.
Abstract
Maxillary sinus mucocele is a benign cyst formation that originates within the sinus and is lined by epithelium (sinus mucosa) containing mucus. It is a rare condition for which it might be very difficult to find a suitable therapeutic approach, especially when it involves the orbit, leading to exophthalmos.
This study reports the case of a right maxillary sinus mucocele in a 68-year-old female patient. Through clinical examination, vestibular deformation from tooth 12 to tooth 16 was determined. Radiologic examination showed that the maxillary sinus was affected, with borders near the orbit. An excision biopsy was performed, which showed histopathological findings of maxillary sinus mucocele. Presentation and classic treatment are discussed.
Keywords: Maxillary sinus, Mucocele, Caldwell Luc.
Received on: 09 Jun 15 Accepted on: 18 Feb 16
Introduction
Maxillary mucocele is a benign cyst formation that originates within one of the paranasal sinuses, lined by epithelium (sinus mucosa) containing mucus, which is caused by the progressive accumulation of mucus. It presents a slowly expanding growth and is asymptomatic at the beginning. It develops as a result of an obstruction of the maxillary sinus and/or paranasal sinuses due to chronic sinusitis, polyps, bone tumors, trauma or after surgery (1-2). In general, mucus is aseptic and has a thick consistency (1). Maxillary sinus mucocele is caused by obstruction of the drainage ostium or a compartment of a septate sinus. The wall of the lesion is the sinus membrane and the maxillary sinus expands, resulting in remodeling of the bone walls (1-2). Clinically, it can be associated with swelling of the cheek, diplopia and dental problems. It is generally painless and, when present, pain indicates infection of the mucocele (3). Mucocele develops gradually, and has a higher incidence between the third and fourth decade of life, and there is no reported sex predilection (4-5). When the ostium is closed for a prolonged period of time, without any possibility of aeration and drainage, mucus accumulates slowly. This causes pressure that progressively dilates the sinus, which in the long term can result in bone deformation and destruction. Expansion takes place through the site of least resistance, which in the maxillary sinus is generally the medial and posterior walls (4). Mucoceles in the maxillary sinuses are exceptional, with prevalence ranging from 3 to 10% (6), and they are often secondary to cicatricial bridles from previous surgeries (Caldwell Luc-like) (7-9). A patient who undergoes a procedure in the maxillary sinus can develop a fibrous septum between the lateral margins of the surgical defect, on the anterior sinus wall and on the posterior sinus wall. If it grows to a certain size, it can extend to the zygomatic body and appear in the cheek as a mass of soft tissue, or progress to the inferolateral region of the orbit (11).
Clinical case A 68-year-old female patient who came to the Emergency Clinic of the School of Dentistry, Udelar, complaining of swelling in the right higher malar area and moderate pain. Intraoral drainage is performed in the vestibular area, near tooth 13, and the patient is prescribed antibiotics (Amoxicillin 875 mg every 8 h). The patient was referred to the Clinic of Oral and Maxillofacial Surgery III with persistence of the swelling but no pain. She has a medical history of controlled but uncompensated hypertension and hypercholesterolemia. She uses upper and lower full prostheses. A deformation in the right side of the face with obliteration of the nasolabial fold (Fig. 1) was observed in the clinical examination of the face. The intraoral examination showed that

both cortical areas in the right upper quadrant area are deformed by the vestibular area, comprising from tooth 12 to tooth 16. This extends up to the bottom of the sulcus, where it meets the right inner side of the upper prosthesis made twenty months ago. It is worth noting that the color of the mucosa that lines the area and the crest is normal and free of lesions (Fig. 2). The deformation is hard and firm to the touch, both on the vestibular and palatal sides. A small drainage consistent with the therapeutic procedure conducted previously in the Emergency Clinic was found during this palpation.

The clinical diagnosis reached was residual cyst, and the differential diagnosis was development cyst, odontogenic and non-odontogenic tumor, and mucocele. Periapical and occlusal radiographies, a teleradiography with a frontal Waters’ view, and an orthopantomography (OPG) were taken. The set of images showed a corticalized lesion measuring, on average, 25 mm in height and 35 mm in length, which is divided by a septum. There is a minor fenestration in the floor of the maxillary sinus, in the rearmost portion. There is also a radiopaque element near tooth 13 that is surrounded by a sharp, radiolucent halo (Fig. 3).

A computerized tomography (CT) scan is indicated for diagnostic purposes and to design a treatment plan. Images were obtained using single cone-beam x-ray CT and corroborated that the lesion measured 40.2 mm in the anterior-posterior direction by 30.1 mm in the vertical direction. All tomographic slices show that the right maxillary sinus is occupied by a lesion with septation near tooth 13, which has not deformed the nasal wall of the maxillary sinus (Figs. 4 and 5).


The initial radiological diagnosis was residual cyst, and the differential diagnosis was mucocele. Treatment plan indicated: prior medical assessment of the patient because of her medical history, approach to the lesion under local anesthesia in order to perform an incisional biopsy and exploratory surgery and/or, possibly, an excisional biopsy.
Surgical procedure After administering local anesthesia, a crestal incision was made from the tuberosity area up to around the midline, and a relieving incision near that area. An exploratory puncture, through which a purulent mucus-like content was obtained, was performed before the incision. A full-thickness flap was lifted from the front to the back, exposing a bone fenestration through which an abundant mucopurulent discharge is drained (Fig. 6).

An ostectomy was performed using a rotary instrument and copious irrigation with normal saline is applied to enlarge the fenestration in order to improve visibility. The lesion was fully removed with sinus lift curettes using the enucleation and curettage technique, and the exeresis of the bone septum that divided the lesion was performed afterwards (Figs. 7, 8 and 9). Finally, closure was performed using continuous suture with 5-0 nylon thread (Fig. 10).




For the postoperative phase, the patient was prescribed Amoxicillin 500 mg every 8 hours for 10 days and Ibuprofen 400 mg every 6 hours for a period of 48 to 72 hours, as analgesic and anti-inflammatory agent. Since no counter opening was made in the inferior meatus, she was prescribed vasoconstrictive nasal drops to keep the ostium patent, for the purpose of facilitating drainage until discharge. The suture was removed ten days later, and the patient’s progress was checked every week for 2 months (Fig. 11).

Pathology report Macroscopic description: Soft, whitish, rounded piece measuring 15 x 15 x 4 mm, an amorphous and gelatinous solid appears when cut, the outer membrane is thin and measures 1 mm. (Fig. 11-bis).

Fig. 11-bis. Enucleated membrane
Microscopic description: Cystic cavity lined by a thin membrane made up of pseudostratified ciliated cylindrical epithelium (sinus mucosa), alternating with areas of hyperplasia, supported by fibrous connective tissue, with areas of edema, with plenty of capillaries, some of which are congestive and mixed inflammatory exudates. The content is amorphous and eosinophilic with inflammatory cells (lymphocytes and plasma cells) scattered in mucous material (Figs. 12 and 13).


Discussion
Clinically, the maxillary sinus mucocele can present swelling in the cheek, diplopia and teeth problems, although typically, without pain (3). In the early phases, diagnosis is fortuitous, taking place almost exclusively when a CT of the paranasal sinuses is taken (12). The cone beam computed tomography (CBCT) shows mucoceles as homogeneous, hypodense and isodense masses, as seen in a brain CT (13), and typically shows a rounded contour of bone (13-16), which makes the injection of a contrast medium unnecessary for diagnosis. This bone detail is an added advantage of the CBCT (15-17), since a radiopaque maxillary sinus, without bone erosion, would suggest a diagnosis of sinusitis, polyps and antral retention cysts (18). The typical maxillary sinus mucocele completely opacifies the antrum and expands the sinus cavity (10). During the early stages, it is not possible to differentiate a mucus-filled sinus with a temporary obstruction from a similar obstructed sinus, which will later form a mucocele. The definitive diagnosis can only be reached when there is sinus expansion (12, 19). If there is expansion and destruction of the bone, the differential diagnosis includes malignant conditions, such as adenoid cystic carcinoma, plasmacytoma, rhabdomyosarcoma, lymphoma, schwannoma and odontogenic tumors (14). Traditionally, bone erosion is not associated with maxillary sinus mucocele. In our patient it had thinned both the posterior and medial walls of the maxillary antrum, as described in the reference literature (4), with bone loss near tooth 16. We argue that a large mucocele can cause bone erosion, but the homogeneous nature of the maxillary lesion, together with the preservation of the layers of mucosa adjacent to the eroded bone, reveal the benign nature of the lesion. Histologically, the maxillary sinus mucocele is confined by an epithelial connective capsule made up of normal respiratory mucosa (pseudostratified ciliated cylindrical epithelium), with an underlying chorion that has fibrosis and chronic inflammation. Finding metaplastic squamous epithelium is rare, since the most common lining is ciliated respiratory mucosa (19-21). Many theories have been suggested to explain the mechanisms responsible for the formation and growth of mucoceles, including cystic degeneration of a seromucous gland, even though the histopathological and molecular examinations conducted by Lund et al. (22, 23) study a dynamic process of bone resorption, where inflammation takes part, through cytokines, which act between the bone and the epithelium releasing prostaglandins. These play a key role in the development of a mucocele, along with the sinus obstruction. Mucoceles, in turn, can be caused by a facial trauma or previous surgery which could result in compartmentalized areas such as the one our patient showed (8). Since the diagnosis in this case was uncertain, an incisional biopsy was initially planned, and when the procedure was performed and it was established that the lesion was clinically benign, it was completely removed. No nasal counter opening was made in the inferior meatus as indicated for this kind of procedure, therefore, nasal drops were prescribed to keep the ostium patent. To complement the surgical procedure, the patient was prescribed a dose of 500 mg of Amoxicillin every 8 hours for a period of no less than 7 days and a dose of 400 mg of Ibuprofen every 6 hours for a minimum of 48 hours, as an analgesic agent. The patient progressed favorably in the short term, in the two-month follow-up.
Conclusions
Maxillary sinus mucocele is a benign cyst formation that originates within the sinus and is lined by a cystic membrane made up of pseudostratified ciliated cylindrical epithelium (sinus mucosa) and connective tissue, which contains mucus. It is mainly caused by an obstruction of the sinus opening (ostium). In imaging studies, it has a hypodense appearance with a faint halo, with contours that are commonly crescent-shaped and starting in the paranasal sinuses, and has an expansive tendency defined by thinned bone margins. Recommended treatment for mucoceles of the maxillary sinus without extension is endoscopic drainage with a broad antrostomy of the middle meatus. A Caldwell Luc surgical approach may also be necessary in cases with extension into the soft tissues of the face or the pterygopalatine fossa, or when it has not been successfully drained through endoscopic surgery of the maxillary sinuses (24).
References
1. Costan VV, Popescu E, Stratulat SI. A new approach to cosmetic/esthetic maxillofacialsurgery: surgicaltreatment of unilateral exophthalmosdue to maxillarysinusmucocele J CraniofacSurg. 2013 May; 24(3): 914–916.
2. Mohan S. Frontal Sinus Mucocele with Intracranial and Intraorbital Extension: A Case Report.J Maxillofac Oral Surg [en línea] 2012; 11(3):337–339. Citado 16 febrero 2016. Disponible en: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3428446/3.
3. Mendelsohn DB, Glass RBJ, Hertzanu Y. Giant maxillary antralmucocele. J LaryngolOtol. 1984; 98:305–310.
4. Fu CH, Chang KP, Lee TJ. The difference in anatomical and invasive characteristics between primary and secondary para-nasal sinus mucoceles. Otolaryngol Head Neck Surg 2007; 136:621–625.
5. Stiernberg CM, Bailey BJ, Calhoun KH, Quinn FB. Management of invasive frontoethmoidal sinus mucoceles. Arch Otolaryngol Head Neck Surg1986;112:1060–1063.
6. Natvig K, Larsen TE. Mucocele of the paranasal sinuses-a retrospective clinical and histological study. J LaryngolOtol1978; 2:1075–1082.
7. Garg AK, Mugnolo GM, Sasken H. Maxillary antralmucocele and its relevance for maxillary sinus augmentation grafting: a case report. Int J Oral Maxillofac Implants2000; 15(2):287-90.
8. Hasegawa M, KuroishikawaY.Protrusion of postoperative maxillary sinus mucocele into the orbit: case reports.Ear Nose ThroatJ1993; Nov,72(11):752-4.
9. Tuli I, Pal I, Chakraborty S, Sengupta S. Persistent deciduous molar as an etiology for a maxillary sinus mucocele. Indian J Otolaryngol Head NeckSurg [en línea] 2011; 63(Suppl 1): 6-8. Citado 16 febrero 2016. Disponible en: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3146690/
10. Som PM, Curtin HD. Head and neck imaging. 4ed. v1. St. Louis: Mosby, 2011. 204–230.
11. Bilnuk LT, Zimmerman RA. Computer assisted tomography: sinus lesions with orbital involvement. Head Neck Surg 1980; 2(4): 293–301.
12. Som PM, Curtin HD. Head and neck imaging. 4ed. v1. St. Louis: Mosby, 2011. 838–840.
13. Trimarchi M, Bertazzoni G, Bussi M. Endoscopic Treatment of Frontal Sinus Mucoceles with Lateral Extension. Indian J Otolaryngol Head NeckSurg [en línea] 2013;65(2):151–156. Citado 16 febrero 2016. Disponible en: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3649028/
14. Mendelsohn DB, Glass RBJ, Hertzanu Y. Giant maxillary antralmucocele. J Laryngol Otol1984;98:305–310.
15. Garg AK, Mugnolo GM, Sasken H. Maxillary antralmucocele and its relevance for maxillary sinus augmentation grafting: a case report. Int J Oral Maxillofac Implants 2000; 15(2):287-90.











 texto en
texto en 


