Servicios Personalizados
Revista
Articulo
Links relacionados
Compartir
Ciencias Psicológicas
versión On-line ISSN 1688-4221
Cienc. Psicol. vol.6 no.2 Montevideo nov. 2012
EARLY APPEARANCE OF THE CHRONIC PAIN PATTERN IN SUBACUTE MUSCULOSKELETAL PATIENTS
APARICIÓN TEMPRANA DEL PATRÓN DE DOLOR CRÓNICO EN PACIENTES MUSCULOESQUELÉTICOS SUBAGUDOS
Leticia León
Rheumatology Unit, Hospital Clinico San Carlos, España
Universidad Camilo José Cela, España
Marta Redondo
Universidad Camilo José Cela, España
Miguel Ángel Pérez-Nieto
Universidad Camilo José Cela, España
Juan A. Jover
Rheumatology Unit, Hospital Clínico San Carlos, España
Lydia Abasolo
Rheumatology Unit, Hospital Clínico San Carlos, España
Resumen: El patrón de dolor crónico implica altos niveles de emociones negativas, dolor y discapacidad percibida. Pocos estudios han evaluado el patrón de aparición del dolor crónico y éste era nuestro objetivo. Método: fueron evaluados 146 participantes con 4 semanas la Baja Laboral por enfermedades musculoesqueléticas (DsMS) y 95 con artritis reumatoide (AR) mediante los siguientes instrumentos: el Cuestionario de Tristeza y Depresión (CTD), el Inventario de Situaciones y Respuestas de Ansiedad–forma breve-. (ISRA-B), Cuestionario de Evaluación de Salud (HAQ), una escala analógica visual para la intensidad del dolor y una escala tipo Likert para la frecuencia del dolor. Los análisis (descriptivos y bivariados) incluyeron una comparación de las puntuaciones de las pruebas entre los pacientes con baja laboral por EM en comparación con los pacientes con AR. Resultados: Los pacientes con Baja Laboral por enfermedades musculoesqueléticas y los pacientes con AR informaron de una percepción similarde su discapacidad, según el HAQ. Pacientes con Baja Laboral por enfermedades musculoesqueléticas informaron mayor frecuencia percibida y más intensidad de dolor que los pacientes con AR. En relación a las emociones negativas, ambos grupos presentaron niveles altos y similares, con algunos niveles más pobres de los pacientes con AR en comparación con Pacientes con Baja Laboral por enfermedades musculoesqueléticas para la ansiedad cognitiva, la ansiedad de evaluación y la de la vida cotidiana (en ISRA-B). Las puntuaciones en depresión presentan los mismos niveles en ambos grupos de pacientes.
Conclusión. Nuestro estudio muestra que los pacientes con dolor subagudo/discapacidad y dolor crónico/discapacidad reportan un patrón muy similar para las emociones negativas y la percepción del dolor y la discapacidad, lo que sugiere que estos factores aparecen en una etapa temprana y favorecen, por tanto, la transición de dolor agudo a crónico/discapacidad.
Palabras clave: dolor crónico; emociones negativas; discapacidad; enfermedades musculoesqueléticas.
Abstract: The chronic pain pattern implies high levels of negative emotions, pain and perceived disability disability perceived. Up to date few studies have assessed when this chronic pain pattern appears. This study is aimed at exploring this issue. Methods: were evaluated 146 subjects with 4 weeks sick leave due to musculoskeletal diseases (MSDs) and 95 with Rheumatoid Arthritis (RA). All patients completed the following assessment instruments: the Sadness and Depression Questionnaire (CTD), Anxiety situations and responses. Inventory –Brief form- (ISRA-B), Health Assessment Questionnaire (HAQ), a visual analogy scale for intensity of pain and a likert type scale for the frequency of pain. The analyses included a comparison on the scores of the tests between patients on sick leave due to MD compared to RA patients. Descriptive and bivariate analyses were performed. Results: Patients on sick leave due to MD and RA patients reported similar perception of their disability, showing a high HAQ score mean. Patients on sick leave due to MD reported more perceived frequency and intensity of pain than RA patients. In relation to negative emotions, both groups reported similar high levels with some poorer levels for RA patients compared to patients on sick leave due to MD for cognitive, evaluation and life situations anxiety. Depression scores presented the same levels for both patients groups. Conclusions: Our study shows that patients with subacute pain/disability and chronic pain/disability report very similar pattern for negative emotions and perception of pain and disability, suggesting that these factors appear in an early stage and contributing to the transition from acute to chronic pain/disability.
Keywords: chronic pain; negative emotions; disability; musculoskeletal diseases.
Correspondencia: Prof. Leticia León, Universidad Camilo José Cela, Madrid. Correo Electrónico: lleon.hcsc@salud.madrid.org
Recibido: 07/2012
Revisado: 09/2012
Aceptado: 10/2012
INTRODUCTION
Chronic pain is a complex question with specific problems. Patients perceive a failure of treatment resources, both professional and patient-controlled, and no confidence that it can find a solution. Also appears a difficulty to discriminate and describe the elements of the problem because the information available and provided by the patient is confused and unclear. Moreover several sleep and mood disorders emerge, contributing to worsen the problem. In social interaction, there is a dominance of communication related to pain, generating problems with professionals and with the environment and finally, the main problem of chronic pain is the impaired quality of life mainly in terms of reduction in functional activity which usually leads a permanent disability in the employment field with all the economic and psychosocial problems associated.
Thus, chronic pain is a high impact problem in industrialized societies as social and individual level in terms of patient suffering, family consequences, lost working time, medical expenses, costs associated with the compensation for disability and the overuse of the health services.
Unlike happens in the acute pain, in the chronic pain there is not a positive value into an adaptative or preventive point of view (Sternbach, 1974; Pinsky, 1983) so its functional value is questionable and a biological usefulness does not exist (Vallejo & Comeche, 1999). Moreover, whereas the acute pain has a good response to the medical procedures, in the chronic pain syndrome results are poor, being this one of the definition criteria. In the course of the development of chronic pain the weighing of these physical, psychological, and social factors may change. For example, during the acute phase of the syndrome biological factors may dominate, but over time psychological and social factors may become the more dominant.
The distinction between acute and chronic pain refers to the duration of pain has a lot of categorizations, but in a recap mode, the pain is called acute the first three weeks, subacute between 4-12 weeks and chronic when the duration is longer than 12 weeks (Waddell, Feder & Lewis, 1997; von Korff, 1994; Nordeman et al., 2006; Schiltenwolf et al., 2006; Karjalainen et al., 2001).
Within the chronic pain are distinguished two types: benign and malignant. This classification has been done on the basis of severity and prognosis of the pathology of origin. Malignant chronic pain is associated with a neoplastic disease or AIDS, and chronic benign pain, would be represented by those processes, disorders or diseases that not directly engage the individual’s survival (Prieto, 1999). Rheumatic diseases of chronic type, such as Rheumatoid Arthritis, are included in this group.
Musculoskeletal diseases (MSDs), including rheumatic diseases are the main cause of restriction of mobility and long-term disability, with a high tendency to chronicity.
Musculoskeletal disabling pain usually follows a ladder that comprise in this order uncertainty, anxiety, blame, anger, helplessness, depression, withdrawal, loss of identity and finally sick role identity. In this final phase we could speak about a chronic pain pattern with elevate levels of negative emotions (mainly anxiety and depression) and a distorted perception of pain due to the low of the threshold and the change in cognitions (Hamilton, Nautra & Reich, 2005).
The anxiety appear after the original stimulus (injury) and response (pain and sympathetic activation) (Lenthem, Slade, Troup & Bentley, 1983; Philips, 1987), but over time, fear of pain may become conditioned through stimulus generalization to an expanding number of situations like simple motor behaviours, work, leisure activities, and sexual activity (Philips, 1987). Subsequently, patients may display maladaptive responses to many stimuli and reduce the frequency of their performance of many activities other than those that initially induced pain.
Research suggests that about 40% to 50% of chronic pain patients suffer from depression (Turk, 1996). Some studies conclude in a review study that anxiety, fear and depression at the time of acute pain are clearly related to the development of chronic pain (Turk, 1997; Linton, 2000).
Finally, the patient´s own pain and disability perception is a key symptom in patients with musculoskeletal diseases, usually determining the patient’s adjustment to illness and his/her overall quality of life.
Within disability literature, we did not find a study that specifies the beginning of the chronification and the appearance of the chronic pain pattern. The purpose of this study was to assess if this pattern appear in an early stage, speeding up the transition from acute to chronic pain/disability.
1. METHODS
1.1. Design
We conducted a cross-sectional study.
1.2. Subjects
We had two sources for the data collection. First source was composed by subjects with work disability related to MSDs (International Classification of Diseases, Ninth Revision coding system, World Health Organization, 1980) lasting for at least four weeks, and followed in our early attention rheumatologic program (Abasolo et al, 2000) excluding subjects with Temporary Work Disability (TWD) due to MSDs lasting for more than eight weeks. Second source was composed by patients with Rheumatic Arthritis (RA) diagnosed according to the 1987 American College of Rheumatology criteria (Arnett et al, 1988), representing a chronic pain condition. We included only patients over 18 years.
All eligible subjects were invited to participate in the study and those who gave their consent were included for the study.
Finally, a total of 146 subjects with 4 weeks of work disability due to MD and 95 with RA were recruited. We excluded MD patients with more than 8 weeks of TWD in order to make a better distinction between subacute and chronic patients.
1.3.Variables
The following variables were analyzed in this study:
For the purposes of the study, sample was classified in two groups: MD patients and RA patients.
Depression was evaluated with the Sadness and Depression Questionnaire CTD (Jiménez García & Miguel Tobal, 2003). The questionnaire has four factors: cognitive scale, physiological scale, behavioral scale and suicidal trend scale, as well as the global level of depression. The psychometric properties for the scale shows a good internal reliability for the different scales (Cronbach´s α=0.95 for cognitive scale, α=0.88 for physiological scale, α=0.88 for behavioral scale, and α=0.97 for global score).
Anxiety was evaluated with the Anxiety situations and responses Inventory-Brief ISRA-B (Miguel-Tobal & Cano-Vindel, 1994). Within anxiety were measured the following components: responses (cognitive, physiological and behavioral), situations (evaluation, interpersonal, phobic and daily-life) and anxiety total responses. The scale shows high internal consistency for the total and each of its parts, ranging between 0.95 and 0.99 (Cronbach´s α=0.96 for cognitive scale, α=0.98 for physiological scale, α=0.95 for behavioral scale, and α=0.99 for global score).
Perceived disability was evaluated with the Health Assessment Questionnaire HAQ (Fries, Spitz & Young, 1982; Esteve, 1993) a 20-item self-administered questionnaire to assess physical self-perceived degree of difficulty to perform 20 activities of daily living grouped into 8 areas: a) dressing and grooming, b) rising , c) eat , d) walk, e) personal hygiene, f) achieve, g) grip and h) other activities. Each item is scored from 0 to 3 on the following scale: 0 = no difficulty, 1 = some difficulty, 2 = with much difficulty, 3 = unable to do so. The final score of the HAQ is an average of these 8 areas so that their movement ranges from 0 (no disability) to 3 (maximum disability). The questionnaire also has several correction questions, divided into two groups with the aim to assess the need for the assistance of another person or use tools/aids to perform the activities described in 20 items. The interest of these questions is that can modify (correct) score of the areas they affect. The Spanish HAQ version reliability (α= 0.89) is similar to other HAQ versions used in different countries.
Pain perception variables were also assessed. Intensity of pain was evaluated with a visual analogy scale measuring intensity of pain when the patient have it, in a scale between 0 (no pain) to 100 (the worse pain), and a likert type scale for the frequency of pain that patient usually have, ranging from 1 (continuously) to 6 (almost never).
We also collected demographic variables (age and gender) for the both groups.
1.4. Statistical analysis
We analyzed the differences between patients on sick leave due to MD compared to RA patients.
Descriptive and bivariate analyses using Student´s t test for continuous variables and chi-squared test for non-continuous variables were performed to examine differences between groups. Analyses were performed with Stata 9.0 software (Stata Corp,
1.5. Ethical approval and informed consent
The MD patients were selected from an intervention open study. The study protocol was approved by the Institutional Review Board of the Hospital Clínico San Carlos (Ethic Committee). The study was included in the “Clinical Controlled Trials” database with number ISRCTN 17984927. The RA sample was selected from AMAPAR (Madrileña Association of RA patients). A consent was obtained from all participants.
2. RESULTS
The mean age was 45 years (SD=10) for MD patients and 52 years (SD=13) for RA patients. Patients on sick leave due to MD were younger than RA patients (P=0.004). Both patients group have the same percentage of woman (77%). No gender differences were found between the study groups.
The main diagnoses were back pain, representing 43.16%, followed by neck pain (31.05%), and soft tissues problems (18.42%). The final 7.37% of the sample are composed by other diagnoses (including 25% osteoarthritis and 19% joint pain without arthritis, and 56% of inflammatory diseases, excluding RA).
We compared the scores in the questionnaires for the MD patients group versus the RA patients group.
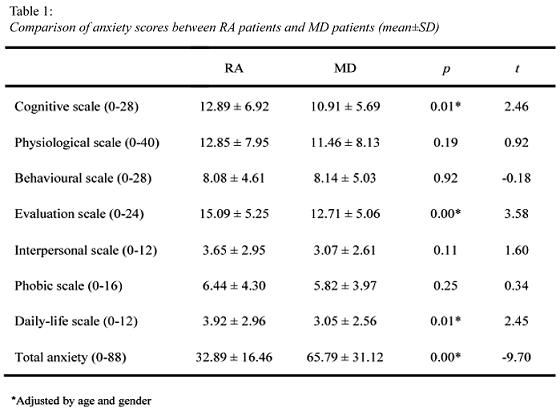
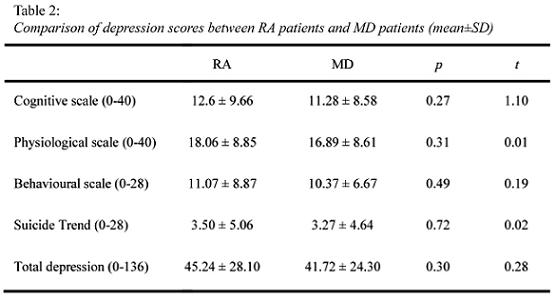
Attending to negative emotions, both groups reported similar high levels. For the anxiety scales, we found some higher levels for RA patients compared to patients on sick leave due to MD in three components, two responses scales, cognitive anxiety (p<0.001) and evaluation anxiety (p<0.001), and also a situation scale, daily-life situation anxiety (p<0.001), but the total score of anxiety (responses and situations) was significantly higher for the MD patients (p<0.001) (Table 1). Depression scores presented the same levels for both patients groups (Table 2).
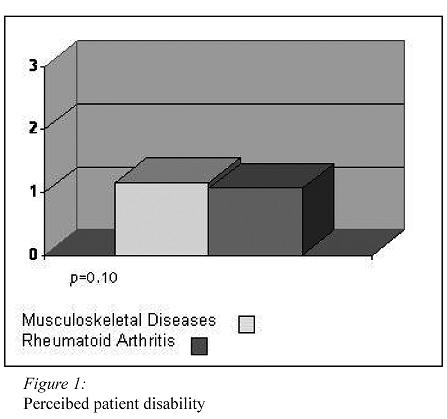
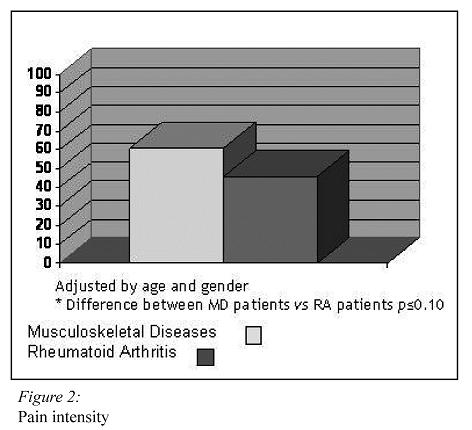
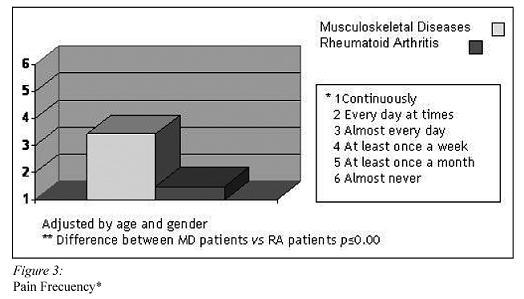
Patients on sick leave due to MD and RA patients reported similar perception of their disability, showing (all patients) a high HAQ score mean (Figure 1). Patients on sick leave due to MD reported more perceived frequency of pain (p<0.001), and more pain intensity (p<0.001) than RA patients (Figures 2 and 3).
3. DISCUSSION
In musculoskeletal diseases, chronicity occurs quickly and often has irreversible consequences. Chronic pain is associated with persistent or recurrent disability which results in high costs for society, and patient suffer.
Our study shows that patients with subacute pain disability and chronic pain disability report very similar pattern for negative emotions and perception of pain and disability, suggesting that these factors appear in an early stage contributing to the transition from acute to chronic pain disability.
Depression scores in these patient groups were twice than in general population, probably due to the strong link between pain and depression. A great deal of previous data is based on the association between pain and depression in patients with rheumatic chronic disease (Wolfe & Hawley,1993; Huyser & Parker, 1999). However, the important finding was that there depression scores have no difference between patient groups, so this link seems to be established in a fast form.
Regarding to anxiety scores, again patients have highest than usual, but when we analyzed in a separate form both patient groups, we can observe that MD group have higher scores, and so anxiety probably decreases over time with the adjustment to illness.
Our results may support the findings of Bronx et al (2005) about that patients with subacute low back pain show a very similar pattern than chronic pain patients, mainly related to negative affect, fear-behavior and work ability, suggesting that those factors appear in an early phase contributing to the low back pain transition acute to chronic. The results of our sample of patients with 4 weeks of TWD found that these patients already have an experience pain pattern similar to other chronic patients samples (Kerns, Turk & Rudy, 1985; Ferrer, Gonzalez & Manassero,1993), showing that pain and disability of 4 weeks of duration can be enough for develop high levels of negative affect and of pain impact and becoming on risk factors for not recovery.
A limitation of the study is probably consequence of the selected questionnaries. Some negative affect questionnaires have some items that overlap with some features of these diseases, so they are probably skewing the results.
Moreover, MD patients are younger than RA patients, because MD patients are people of working age, while RA could be retired.
Our results suggest a faster stepwise deterioration of impairment and disability, from healthy controls to patients with chronic pain, making subacute patients a main therapeutic goal in order to prevent irreversible states through multidisciplinary programs designed to manage pain and prevent disability.
In musculoskeletal diseases is important to perceive if underlying physical problem another job-related or personal problem exist, which may be the cause of the long duration of the problem in many cases. A personal problem that generates sadness makes that person can tolerate less pain. A subject to a high level of stress that does not control his muscle tension has more probability for recurrent muscle contractures.
Certainly, this field still needs more research about “yellow flags” or warning signs inform us that the process of patient disability is not being resolved in an appropriate (substance abuse, manual work with high risk) form, and the patient needs some additional care. Recently, it is beginning to identify patterns or prediction rules for identifying these yellow flags that include not only physical, but also social and psychological factors (Kuijpers et al, 2006; Shaw et al, 2009).
It is important to highlight the change that is being produced in the investigation about musculoskeletal problems focusing not so much in the pain of the patient, but in the disability and quality of life worse due to these problems, especially in the age range between 40 and 60 years (Daffner, 2003) and active workers (Leon, 2009). It is necessary also to work in an early way in these patients, since we as have seen the chronic pain pattern happens quickly and it is a main goal to avoid its development. Moreover there are a large percentage of patients who become chronic that never recovery to work, so it is very important to solve this problem at the beginning of it, to avoid patient suffering and achieve effective interventions for the prevention of chronic work disability.
4. CONCLUSIONS
Our study shows that patients with subacute pain/disability and chronic pain/disability report very similar pattern for negative emotions and perception of pain and disability, suggesting that these factors appear in an early stage and contributing to the transition from acute to chronic pain/disability.
5. REFERENCES
Abasolo, L.,Blanco, M., Bachiller, J., Candelas, G., Collado, P., Lajas, C.,...Jover J. A. (2005). A Health System Program To Reduce Work Disability Related to Musculoskeletal Disorders. Annals of Internal Medicine, 143(6), 404-414.
Arnett, F.C., Edworthy, S.M., Bloch, D.A., McShane, D.J., Fries, J.F., Cooper, N.S,... Hunder, G.G. (1988). The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum, 31, 315-324.
Brox, J. I., Storheim, K., Holm,
Daffner, S. D., Hilibrand, A. S., Hanscom, B. S., Brislin, B. T., Vaccaro, A. R. & Albert, T. J. (2003). Impact of neck and arm pain on overall health status. Spine, 17, 2030-2035.
Esteve, J., Batlle, E., Reig, A. & Grupo para la adaptación del HAQ a la población española. (1993). Spanish version of the health assessment questionnaire: reliability, validity and transcultural equivalency. J Rheumatol, 20, 2116-2122.
Ferrer, V. A., Gonzalez, R. & Manassero, M. A. (1993). El West Haven Yale Multidimensional Pain Questionnaire: Un instrumento para evaluar al paciente con dolor crónico. Dolor, 8, 153-160.
Fries, J. F., Spitz, P. W. & Young, D. Y. (1982). The dimensions of health outcomes: the Health Assessment Questionnaire disability and pain scales. J Rheumatol, 9, 789-793.
Hamilton, N.A., Zautra, A.J. & Reich, J.W. (2005). Affect and pain in rheumatoid arthritis: do individual differences in affective regulation and affective intensity predict emotional recovery from pain?. Ann Behav Med,29(3):216-24.
Huyser, B.A. & Parker, J.C. (1999). Negative affect and pain in arthritis. Rheum Dis Clin N Am, 1, 105-121.
Jiménez, García, G. I. & Miguel,Tobal, J. J. (2003). El cuestionario tridimensional para la depresión (CTD): un nuevo instrumento para medir la tristeza/depresión. Ansiedad y Estrés, 9 (1), 17-34.
Karjalainen, K., Malmivaara, A., van Tulder, M., Roine, R., Jauhiainen, M., Hurri, H. & Koes, B. (2001). Multidisciplinary biopsychosocial rehabilitation for subacute low back pain in working-age adults: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine, 26(3), 262-269.
Kerns, R. D., Turk, D. C., & Rudy, T. E. (1985). The West Haven-Yale Multidimensional Pain Inventory (WHYMPI). Pain, 23, 345-356.
von Korff, M. (1994). Studying the natural history of back pain. Spine,19,2041S-2046S.
Kuijpers, T., van der Windt, D., van der Heijden, G., Twisk, J., Vergouwe, Y. & Bouter, L. (2006). A prediction rule for shoulder pain related sick leave: a prospective cohort study. BMC Musculoskeletal Disorders, 7, 97.
Leon, L., Jover, J.A., Candelas, G., Lajas, C., Vadillo, C., Blanco, M.,...Abasolo, L. (2009). Effectiveness of an early cognitive behavioral treatment for work disability due to musculoskeletal disorders. Arthritis Care & Research, 61 (7), 996–1003.
Lenthem, J., Slade, P. O., Troup, J. P. G., & Bentley, G. (1983). Outline of a fear-avoidance model of exaggerated pain perception. Behav Res Ther, 21, 401-408.
Linton, S. J. (2000). A review of psychological risk factors in back and neck pain. Spine 25:1148-56.
Miguel-Tobal, J. J. & Cano-Vindel, A. (1994). Inventario de situaciones y respuestas de ansiedad (ISRA): Manual. / Inventory of Situations and Responses of Anxiety (ISRA). Manual (3. rev. ed.).
Nordeman, L., Nilsson, B., Möller, M. & Gunnarsson, R. (2006). Early acces to physical therapy treatment for subacute low back pain in primary health care. Clin J Pain, 22(6), 505-511.
Philips, H. C. (1987). Avoidance behaviour and its role in sustaining chronic pain. Behav Res Ther, 25, 273-279.
Pinsky, J. J. (1983). Aspects of the psychology of pain. In B. L. Crue (Ed.), Chronic Pain.
Prieto, V. J. (1999). El dolor crónico. Aspectos psicoevolutivos en la edad adulta. Ed.
Schiltenwolf M, Buchner M, Heindl B, von Reumont J, Müller A & Eich W. (2006). Comparison of a biopsychosocial therapy (BT) with a conventional biomedical therapy (MT) of subacute low back pain in the first episode of sick leave: a randomized controlled trial. European Spine Journal, 15, 1083-1092.
Shaw WS, Pransky G, Winters T, Tveito TH, Larson SM & Roter DL. (2009). Does the presence of psychosocial „yellow flags“ alter patient-provider communication for work-related, acute low back pain? J Occup Environ Med, 51(9),1032-1040.
Sternbach, R. A. (1974). Pain patients. Traits and treatment.
Turk, D.C. (1996). Biopsychosocial perspective on chronic pain. In R. J. Gatchel and D. C. Turk (Eds.), Psychological approaches to pain management: A practitioner’s handbook (pp.3-32).
Turk, D. C. (1997). The role of demographic and psychosocial factors in the transition from acute to chronic pain. In T. S. Jensen, T. A. Turner and Z. & Wiesenfeld-Hallin (Eds.), Proceedings of the 8th World Congress on Pain, progress in pain research and management, (Volume 8).Seattle: IASP Press.
Vallejo, M. A & Comeche, M. I. (1999). Depresión, ansiedad y dolor crónico. En G. Fernández-Abascal y F. Palmero (Eds), Emociones y salud.
Waddell, G., Feder, G., & Lewis, M. (1997). Systematic reviews of bed rest and advice to stay active for acute low back pain. Br J Gen Pract, 47, 647-652.
Wolfe F, Hawley DJ. (1993). The relationship between clinical activity and depression in rheumatoid arthritis. J Rheumatol, 12, 2032-2037.
World Health Organization (1980). International Classification of Diseases, Ninth Revision, Clinical Modification. Washington, DC: Superintendent of Documents, US Printing office. 1980; 1-3.
Para citar este artículo:
León, L., Redondo, M., Pérez-Nieto, M. A., Jover J. A., Abasolo, L. (2012). Early appearance of the chronic pain pattern in subacute musculoskeletal patients. Ciencias Psicológicas VI (2): 175-182.